- info@careermakers.edu.np
- +977 1 4423870
Adcirca
Benjamin W. Eidem, MD, FACC, FASE
- Associate Professor
- Departments of Pediatrics and Pediatric Cardiology
- Mayo Clinic
- Rochester, Minnesota
Physical examination reveals a golden yellow discoloration of the skin and conjunctivae venogenic erectile dysfunction treatment generic 20 mg adcirca free shipping, the abdomen is distended and a fluid wave is present erectile dysfunction daily pill order adcirca 20 mg with visa, and small spider-like red discolorations are present on the skin impotence solutions adcirca 20 mg order with amex. Excessive aspirin consumption Liver 179 13 DiseasesoftheLiver erectile dysfunction pre diabetes cheap adcirca 20 mg fast delivery,Gallbladder impotence kit discount adcirca 20 mg buy on line,andBiliaryTract 7. A 44-year-old male with a history of significant alcohol consumption (about 10-12 beers per day for the last 20 years) and hepatitis C positivity presents to an acute care clinic with a history of abdominal pain and increased fullness, which has developed over several weeks to months. Physical examination reveals some abdominal pain with palpation, and a negative stool occult blood test. Given the previous clinical scenario, of the following, what is characteristic for the mass A 43-year-old male with a history of chronic alcoholism and hepatitis C infection is brought to the emergency room by his friends because he has twice vomited large amounts of blood. Given the previous clinical scenario, of the following, what is the most likely mechanism for the development of the lesion causing his bleeding A 37-year-old male presents to an acute care clinic with complaints of abdominal pain, which began a few days ago. He reports that whenever he becomes very stressed, sometimes the whites of his eyes will turn somewhat yellow. A 43-year-old male presents to an acute care clinic because of yellowing of his eyes, fatigue, and malaise. Of the following, what other test must be positive, or be elevated, to justify serologic testing for hepatitis D virus A 34-year-old female presents to her family physician complaining of new exertional dyspnea. Of the following, what would histologic examination of the liver most likely reveal A biopsy of the liver reveals macrovesicular steatosis with occasional fat vacuoles rimmed with neutrophils. A serum protein electrophoresis revealed an increased amount of protein in the region. The patient is not on any medication, and she consumes about 1 alcoholic beverage per month. Of the following, what additional laboratory testing is most likely to identify the disease X-ray of the skull Liver 181 13 DiseasesoftheLiver,Gallbladder,andBiliaryTract 18. Results of a third round of tests were serum iron of 201 g/dL, ferritin of 289 ng/mL, and transferrin saturation of 53%. Given the previous clinical scenario, which of the following is a complication of the disease process Given the previous clinical scenario, if the patient undergoes a liver biopsy, which of the following stains is most likely to be positive A 24-year-old male presents to an acute care clinic, complaining of the relative sudden onset of yellowing of his skin associated with nausea, vomiting, fatigue, and muscle aches. He works at a daycare facility and, for meals at home, frequently consumes raw oysters. A physical examination reveals jaundice, but no track marks or other signs of intravenous drug abuse. The patient is not on any medication, and he reportedly drinks about 1 to 2 beers per week socially with friends. Given the previous clinical scenario, which of the following is most characteristic of his disease process A 53-year-old male presents to his family physician with complaints of fever, chills, and abdominal pain. He reports that he has had past episodes of a similar nature, but has not chosen to seek treatment. He has a past medical history of ulcerative colitis and had a colectomy 5 years ago for Stage I colonic adenocarcinoma, which has been in remission. Given the previous clinical scenario, of the following, what antibody is often associated with this disease A 42-year-old female presents to her family physician complaining of abdominal pain. The pain usually comes on after a meal, increases in intensity for a few minutes and then subsides after about an hour or two. Other than mild hypothyroidism requiring hormone replacement, she has no other significant past medical history. Given the previous clinical scenario, which of the following is the most likely mechanism causing her disease process Anti-smooth muscle antibody Liver 183 13 DiseasesoftheLiver,Gallbladder,andBiliaryTract 30. Given the previous clinical scenario, of the following, what is a possible complication of her presenting disease process Given the previous clinical scenario, pathologic examination of the affected organ would reveal which of the following A 66-year-old male presents to his family physician with complaints of itching, pale-colored stool, and fatigue. A 43-year-old male presents to an acute care clinic because of yellowing of his eyes. A 40-year old female presents to an acute care clinic with complaints of pain on the upper right side of her abdomen and slight yellowing of her eyes. Review of her systems indicates that she has had similar episodes of similar pain in the past, but none accompanied by yellowing of the eyes. A 35-year-old male with a history of ulcerative colitis presents to an acute care clinic. In the last three weeks he has twice had a fever, up to 100°F, accompanied by chills, abdominal pain, and some yellow discoloration of his eyes. He has no history of gallstones or alcohol use, other than social consumption of a few beers each month. Given the previous clinical scenario, of the following, what would a liver biopsy reveal A 41-year-old obese female presents to an acute care clinic with complaints of pain on the right side of her abdomen that started suddenly a few hours ago and has been increasing in severity. Given the previous clinical scenario, on physical examination, the doctor palpates her right upper quadrant, which causes her to stop breathing. She is subsequently diagnosed with chronic cholecystitis, and her gallbladder is removed surgically. The pathologist examining the gallbladder identifies multiple small black stones in her gallbladder. A pathologist is examining a section of a liver from an autopsy and notes that the centrilobular hepatocytes are eosinophilic and that nuclei are not visible, especially when compared to the more basophilic hepatocytes in the area around the portal tracts. Her parents report that she was doing fine yesterday morning, but that she wanted to stay in her room and study all day for an upcoming test, to forget about her boyfriend breaking up with her. The family reports that she has no underlying medical conditions that they know of. A female laboratory worker at a state crime lab has her yearly testing for hepatitis B and C and also has a complete blood cell count, a liver panel, and a kidney panel (with 20 total tests performed). She has no medical background and goes to the medical examiner to consult in private. Over the past week, she has developed abdominal pain and noticed that the whites of her eyes and skin are yellow. Given the previous clinical scenario, of the following, what is true regarding the presenting condition Given the previous clinical scenario, of the following, what laboratory test is likely to be positive A 28-year-old female is found unresponsive in her bedroom by her parents, with whom she lives. In the emergency room, she is not responsive to questions and only slightly responsive to a sternal rub. Her parents report that she has no significant past medical history, other than depression treated with paroxetine. Of the following tests, which is most likely to identify the cause of her current state Given the previous clinical scenario, of the following, what would a histologic examination of the liver most likely reveal Which of the following conditions would be most expected to cause this pattern of laboratory abnormalities A 73-year-old female who is on warfarin for a mechanical heart valve, implanted to treat degenerative calcified aortic stenosis, falls and sustains a large hematoma of her left buttocks and thigh, extending from just above her left hip to just above her left knee. Of the following, what laboratory test would be most likely to be elevated in the following few weeks Given the previous clinical scenario, of the following, which statement is correct regarding his disease process A 52-year-old male presents to his family physician with complaints of vague abdominal pain and a sensation of fullness. The patient is scheduled for resection, and a pathologist examining the tumor identifies it as being derived from bile ducts. One complication of ulcerative colitis is a significant risk factor for the tumor. A 23-year-old pregnant female presents to the emergency room complaining of pain in the upper portion of the right side of her abdomen. Physical examination reveals a fluid wave and hepatomegaly, with her liver palpable 6 cm below the costal margin. A patient was twice identified to have an elevated alkaline phosphatase, both times around 290 mg/dL. Correct: Hepatocellular carcinoma (D) Cirrhosis of the liver is a risk factor for hepatocellular carcinoma. In adults, hepatocellular carcinoma rarely occurs without the background of cirrhosis (D). Cirrhosis itself does not increase the risk for any of the other tumors or conditions. Correct: Chronic alcohol use (A) the patient has signs and symptoms consistent with cirrhosis: spider angiomas, jaundice, and a fluid wave indicating ascites. Although a relatively small number of chronic alcoholics develop cirrhosis, chronic alcoholism is a very common condition (A). Both obstruction of bile ducts and congestive heart failure are causes of cirrhosis, but less commonly a cause than alcohol use (B, C). Inflammation of the pancreas and excessive alcohol consumption are not associated with cirrhosis (D, E) 4. Howell-Jolly bodies are not found in the liver, and targetoid lesions of the bile ducts are not associated with alcohol use (D, E). Correct: Spontaneous bacterial peritonitis (D) Patients with cirrhosis can develop an infection of the ascitic fluid, which is referred to as spontaneous bacterial peritonitis (D). The other conditions are not by themselves normally associated with a significant amount of infected intra-abdominal fluid (A-C, E). Esophageal carcinomas can cause bleeding and do occur in alcoholics, but they would be a less common cause of massive bleeding and not as common in alcoholics as cirrhosis, and he has no other risk factors for esophageal carcinoma (A). Neither a peptic ulcer nor a fistula between the common bile duct and small intestine would cause ascites (D, E). The history and physical examination are consistent with the diagnosis of ascites. Ascites develops due to increased hydrostatic pressure in the abdominal vasculature caused by portal hypertension, which develops due to the cirrhosis, and also due to decreased plasma oncotic pressure, due to decreased production of albumin by the liver. Although the other tests may have abnormal concentrations detected on laboratory testing of a patient with cirrhosis, they are not the direct cause of the increased fluid volume in the peritoneal cavity (A-C, E). Correct: Hepatocellular carcinoma (C) Given the history, the patient most likely has cirrhosis of the liver, and has developed a hepatocellular 188 13. Liver metastases can cause an elevated -fetoprotein; however, given there is a solitary mass and the stool occult blood test is negative, metastatic colonic adenocarcinoma is not likely (D). Cavernous hemangiomas and focal nodular hyperplasia would occur as a single mass in the liver but are not commonly associated with an increased -fetoprotein (A, B). A central scar is characteristic of focal nodular hyperplasia (A), exposure to vinyl chloride is a known risk factor for angiosarcoma (B), hepatic adenomas are associated with use of oral contraceptives, and use of corticosteroids is not a commonly recognized risk factor for hepatocellular carcinoma (C). Patients are not necessarily likely to develop a warm autoimmune hemolytic anemia, as these anemias are most likely to develop in people with an abnormal immune response. Correct: Rupture of a dilated vein (C) Given the clinical history of chronic alcoholism and hepatitis C infection, the patient most likely has cirrhosis of the liver, which has caused the development of esophageal varices. Rupture of esophageal varices is a common cause of death in individuals with cirrhosis. The rupture site is not easily tamponaded, and patients with cirrhosis of the liver may have decreased concentrations of clotting factors, causing them to bleed even more easily (C). Although alcoholics can tear the esophagus (and hemorrhage), which is a MalloryWeiss tear, the hemorrhage is preceded by prolonged vomiting (B). Any of the other choices, with the exception of acute alcohol toxicity, could also potentially cause an individual to vomit blood, but none would be as common in an alcoholic as ruptured esophageal varices. Correct: Portal hypertension (C) Based on the clinical scenario, the patient most likely has cirrhosis of the liver, due to alcohol use and hepatitis C infection, and has developed esophageal varices, which are bleeding.
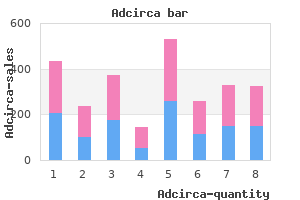
In animals impotence natural treatments best adcirca 20 mg, the amygdala has been shown to be critical for the conditioning of fear erectile dysfunction drug companies discount adcirca online. The amygdala sends signals to a range of different brain structures involved in the fear circuit impotence 19 year old order adcirca 20 mg overnight delivery, including other regions that also appear involved in responses to threat erectile dysfunction diabetes type 2 treatment 20 mg adcirca order with visa. Studies suggest that when shown pictures of angry faces (one signal of threat) impotence treatments natural 20 mg adcirca buy free shipping, people with several different anxiety disorders respond with greater activity in the amygdala than do people without anxiety disorders (Fox, Oler, et al. Hence, elevated activity in the amygdala, a core part of the fear circuit, may help explain many different anxiety disorders. The medial prefrontal cortex helps to regulate amygdala activity-it is involved in extinguishing fears and is engaged when people are regulating their emotions (Indovina, Robbins, et al. The medial prefrontal cortex is involved in the conscious processing of anxiety and fear (LeDoux & Pine, 2016). Researchers have found that adults who meet diagnostic criteria for anxiety disorders display less activity in the medial prefrontal cortex when viewing and appraising threatening stimuli (Britton, Grillon, et al. The pathway, or connectivity, linking the amygdala and the medial prefrontal cortex may be deficient among those with anxiety disorders (Kim et al. These deficits in connectivity between these two regions may interfere with the effective regulation and extinction of anxiety. Although we focus on the amygdala and the medial prefrontal cortex here, other regions interface with the amygdala to process threat-related stimuli. The bed nucleus of the stria terminalis is also engaged by cues of threat (Shackman & Fox, 2016). The anterior cingulate cortex appears involved in the anticipation of threat, and the insula appears related to awareness of and processing of bodily cues, such as the high arousal invoked by threat. The hippocampus plays a role in encoding the context in which feared stimuli occur (Vervliet, Craske, & Hermans, 2013). We will discuss another part of the fear circuit, the locus coeruleus, when we discuss specific anxiety disorders. The amygdala and medial prefrontal cortex are particularly involved in anxiety disorders. Serotonin, which we discussed in Chapter 5 for its role in mood disorders, is believed to help modulate emotions (Carver, Johnson, & Joormann, 2008). Researchers have also used drug manipulation studies to show that anxiety disorders are related to increased levels of norepinephrine and changes in the sensitivity of norepinephrine receptors (Neumeister, Daher, & Charney, 2005). Norepinephrine is a key neurotransmitter in the activation of the sympathetic nervous system for "fight-orflight" responses. In addition to human research, a huge body of animal research, using genetic paradigms and pharmacological manipulations, suggests that an array of neurotransmitters and neuropeptides are involved in the process of fear conditioning and extinction. As mentioned in Chapter 5, cortisol has a strong diurnal rhythm, with a large increase as people awaken. Personality: Behavioral Inhibition and Neuroticism Some infants show the trait of behavioral inhibition, a tendency to become agitated and cry when faced with novel toys, people, or other stimuli. This behavioral pattern, which has been described in infants as young as 4 months old, may be inherited and may set the stage for the later development of anxiety disorders. Behavioral inhibition is a particularly strong predictor of social anxiety disorder: infants showing elevated behavioral inhibition were 3. Neuroticism is a personality trait defined by the tendency to experience frequent or intense negative affect. In studies involving more than 10,000 participants, neuroticism predicted the onset of both anxiety disorders and depression (Ormel, Jeronimus, et al. In one large study, people with high levels of neuroticism were more than twice as likely to develop an anxiety disorder as were those with low levels (de Graaf, Bijl, et al. Cognitive Factors Researchers have focused on several separate cognitive factors in anxiety disorders. Here, we concentrate on four: sustained negative beliefs about the future, a perceived lack of control, over-attention to signs of threat, and intolerance of uncertainty. Sustained Negative Beliefs About the Future People with anxiety disorders often report believing that bad things are likely to happen. For example, people with panic disorder might believe that they will die when their heart begins to pound, whereas people with social anxiety disorder might believe that they will suffer humiliating rejection if they blush. For example, by the time a person survives 100 panic attacks, you might expect the belief "this attack means I am about to die" would fade. One reason these beliefs might be sustained is that people think and act in Common Risk Factors Across the Anxiety Disorders 177 Perceived Lack of Control People who report experiencing little sense of control over their surroundings are at risk for a broad range of anxiety disorders (Mineka & Zinbarg, 2006). Childhood experiences, such as traumatic events, punitive and restrictive parenting, or abuse, may promote a view that life is not controllable. Indeed, about half of people with anxiety disorders report a Infants and toddlers showing behavioral inhibition-high anxiety about novel situations and people-are at greater history of childhood physical or sexual abuse (Cougle, Timpano, et al. On the whole, the degree to which a person experiences control over their environment can influence whether an anxiety disorder develops. Animal studies have illustrated that a lack of control over the environment can promote anxiety. One group of monkeys grew up with the ability to choose whether and when they would receive treats. A second group of monkeys had no control over whether and when they received treats but received the same number of treats. In the third year of life, monkeys who had grown up without control behaved in ways that looked anxious when facing new situations and interacting with other monkeys; monkeys who had grown up with control showed less anxiety. In sum, animal and human studies both point toward the importance of perceived lack of Second screen control in the development of anxiety disorders. Attention to Threat A large body of research indicates that people with anxiety disorders pay more attention to negative cues in their environment than do people without anxiety disorders (Williams, Watts, et al. In a meta-analysis of 172 studies, each of the specific anxiety disorders was associated with heightened attention to threatening stimuli on tasks such as the dot probe task (Bar-Haim, Lamy, et al. For example, people with social anxiety disorder have been found to selectively attend to negative faces (Bantin, Stevens, et al. Researchers have also shown that this heightened attention to threatening stimuli happens automatically and very quickly-before people are even consciously aware of the stimuli (Staugaard, 2010). Once a threatening object captures their attention, anxious people have a difficult time pulling their attention away from that object; they tend to stay focused on a threatening object longer than others do (Cisler & Koster, 2010). In sum, anxiety disorders are associated with selective attention to signs of threat. In one line of experimental research, investigators have examined whether attention to anxiety-related information can be created, then whether this attention "bias" leads to more anxiety (MacLeod & Mathews, 2012). To train people to attend to threatening words, researchers used the dot probe task. To teach a negative bias, participants view hundreds of trials in which the dot is more likely to occur where the negative word was. For a control group, the dot is equally likely to appear where either the negative or neutral word was. People who were trained to attend to negative words reported a more anxious mood after training, especially when they were given a challenging task like an unsolvable puzzle to perform. The findings suggest that the way we focus our attention can foster an anxious mood. On the first screen of each trial, participants see one neutral word and one negative word. On the second screen, a dot appears in the location where one of the two words was. The participant is asked to press a button as quickly as possible to indicate whether the dot appears on the left or right side of the screen. In the case shown here, a person who was looking at the word death will see the dot and respond more quickly than a person who was looking at the word table. For example, people who fear they will die from a fast heart rate stop all physical activity the minute they feel their heart race. Researchers have examined this question by training people diagnosed with generalized anxiety disorder to attend to positive information (Amir, Beard, et al. To train a positive bias, the researchers used a version of the dot probe task in which dots appeared where the positive words had been. Participants in a control group completed an equivalent number of training sessions with a control version of the dot probe task. Parallel benefits of positive attention training have been shown among adults with social anxiety and among children with clinically significant anxiety (MacLeod & Clarke, 2015). To date, more positive findings have been observed from programs focused on training positive rather than negative cognitive biases (Mogg, Waters, & Bradley, 2017). Intolerance of Uncertainty People who have a hard time accepting ambiguity, that is, who find it intolerable to think that something bad might happen in the future, are more likely to develop anxiety disorders (Dugas, Marchand, & Ladouceur, 2005). This intolerance of uncertainty can predict increases in worry over time (Laugesen, Dugas, & Bukowski, 2003). People with anxiety disorders, but also those with major depressive disorder and obsessive-compulsive disorder tend to struggle when the future is uncertain (Gentes & Ruscio, 2011; McEvoy & Mahoney, 2012). Quick Summary Many risk factors set the stage for anxiety disorders generally, rather than for a specific anxiety disorder. These models have been extended to consider that the classical conditioning may be driven by direct exposure to an event, observation of someone else experiencing an event (modeling), or verbal instruction. It also appears that people with anxiety disorders acquire classically conditioned fears more quickly than others do, and find it harder to extinguish these fears. The personality traits of behavioral inhibition and neuroticism are both related to the development of anxiety disorders. From the cognitive perspective, anxiety disorders are associated with negative expectations about the future, beliefs that life is uncontrollable, a bias to attend to negative information, and intolerance of uncertainty. Research suggests that genes can explain percent of the variance in anxiety disorders. Here, we turn to the question of how each of the specific anxiety disorders arises. That is, why does one person develop a specific phobia while another person develops generalized anxiety disorder Keep in mind the common etiological factors already described, and think about how these commonalities relate to and combine with the specifics described next. Etiology of Specific Phobias the dominant model of phobias is the two-factor model of behavioral conditioning described earlier. In the behavioral model, specific phobias are seen as a conditioned response that develops after a threatening experience and is sustained by avoidant behavior. In one of the first illustrations of this model, John Watson and his graduate student Rosalie Rayner published a case report in 1920 in which they demonstrated creating an intense fear of a rat (a phobia) in an infant, Little Albert, using classical conditioning (see photo). Little Albert was initially unafraid of the rat, but after repeatedly seeing the rat while a very loud noise was made, he began to cry when he saw the rat. Although this type of experiment would likely not be approved by modern ethics boards, the experiment provided important evidence that intense fears could be conditioned. As already mentioned, behavioral theory suggests that phobias could be conditioned by direct trauma, modeling, or verbal instruction. But do most people with a phobia report one of these types of conditioning experiences In one study, 1937 people were asked whether Little Albert, shown here with Rayner and Watson, was classically condithey had these types of conditioning experiences before tioned to develop a fear of a white rat (Watson & Raynor, 1920). Although conditioning experiences were common, about half of the people in the study could not remember any such experiences. Obviously, if many phobias start without a conditioning experience, this is a big problem for the behavioral model. But proponents of the behavioral model argue that people may forget conditioning experiences (Mineka & Öhman, 2002). Because of memory gaps, simple surveys of how many people remember a conditioning experience do not provide accurate evidence about the behavioral model. Even among those who have had a threatening experience, many do not develop a phobia. To begin, the risk factors we have described, such as genetic vulnerability, neuroticism, negative cognition, and propensity toward fear conditioning, probably operate as diatheses-vulnerability factors that shape whether or not a phobia will develop in the context of a conditioning experience (Mineka & Sutton, 2006). It also is believed that only certain kinds of stimuli and experiences will contribute to development of a phobia. But phobias of insects or other animals, natural environments, and blood are common. As many as half of women report a fear of snakes; moreover, many different types of animals also fear snakes (Öhman & Mineka, 2003). Researchers have suggested that during the evolution of our species, people learned to react strongly to stimuli that could be life-threatening, such as heights, snakes, and angry humans (Seligman, 1971). That is, evolution may have "prepared" our fear circuit to learn fear of certain stimuli very quickly and automatically; hence, this type of learning is called prepared learning. In support of this idea of evolutionarilyadaptive fears, researchers have shown that monkeys can be conditioned to fear snakes and crocodiles but not flowers and rabbits (Cook & Mineka, 1989). As researchers have tested this model, some have discovered that people can be initially conditioned to fear many different types of stimuli (McNally, 1987). Fears of most types of stimuli fade quickly with ongoing exposure, though, whereas fears of naturally dangerous stimuli are sustained in most studies (Dawson, Schell, & Banis, 1986). Digital Vision/Getty Images Etiology of Social Anxiety Disorder In this section, we review behavioral and cognitive factors related to social anxiety disorder. The trait of behavioral inhibition may also be important in the development of social anxiety disorder. Behavioral Factors: Conditioning of Social Anxiety Disorder the prepared learning model suggests that we have evolved to pay special attention to signs of danger, including angry people, threatening animals, and dangerous natural environments.
There has been growing concern about a lack of reproducibility of scientific findings erectile dysfunction treatment options-pumps generic adcirca 20 mg visa. It entails putting the statistical comparisons from single studies into a common format-the effect size-so that scientists can average the results of many studies erectile dysfunction doctor in delhi order adcirca online pills. Analogue Studies · Analogue experiments allow the researcher to study a minor variant of a risk factor related to psychopathology erectile dysfunction uptodate buy cheap adcirca 20 mg on-line, such as stressors impotence def discount 20 mg adcirca mastercard. Although the stressor used in an analogue study is typically much Answers to Check Your Knowledge Questions 4 erectile dysfunction causes emotional cheap 20 mg adcirca free shipping. Pro: Placebos allow for a control of the effects of treatment expectations, and research suggests that the placebo effect can be large; Con: Placebo trials involve withholding active treatment from people who may have serious symptoms and distress, which is an ethical concern. Treatment manuals provide specific guidance to therapists, so that researchers can be more confident that therapists are providing the same type of intervention; 4 False (Explanation: Hundreds of trials have been conducted to test empirically supported treatments with minority individuals and those from differing ethnic and racial backgrounds); 5. Pro: the analogue study has the advantage of the experimental manipulation, which provides internal validity. Registering study hypotheses, measures, and analyses before the study begins; making data available; placing more emphasis on the importance of hypotheses and the quality of study methods than the results of a study when reviewing a manuscript to consider potential publication; using larger samples; routinely considering whether a finding has been replicated; 3. Describe the symptoms of depression, the diagnostic criteria for depressive disorders, and the epidemiology of depressive disorders. Explain the symptoms of mania, the diagnostic criteria for bipolar disorders, and the epidemiology of bipolar disorders. Discuss the genetic, neurobiological, social, and psychological factors that contribute to the mood disorders. Describe the medication and psychological treatments of mood disorders as well as the current views of electroconvulsive therapy. Explain the epidemiology of suicide, the risk factors for suicide, and methods for preventing suicide. She felt guilty about the loss of her job and became preoccupied with signs of her overall incompetence. Each night, she struggled for more than an hour to fall asleep, only to wake up frequently throughout the night. She also had little energy for and no interest in activities that she had enjoyed in the past. Household chores felt impossible for her to complete and her husband began to complain. Their marriage had already been strained for 2 years, and her negativity and lack of energy contributed to further arguments. In this chapter, we begin by discussing the clinical description and the epidemiology of the different mood disorders. Next, we consider various perspectives on the etiology of these disorders, and then we consider approaches to treating them. We conclude with an examination of suicide, an action far too often associated with mood disorders. We will begin by discussing the depressive disorders, and then we will turn to the bipolar disorders. Within each, we will describe the core signs, the formal criteria for the specific disorders, and then the epidemiology and consequences of these disorders. Clinical Descriptions and Epidemiology of Depressive Disorders the cardinal symptoms of depression include profound sadness and/or an inability to experience pleasure. Most of us experience sadness during our lives, and most of us say that we are "depressed" at one time or another. But most of these experiences do not have the intensity and duration to be diagnosable. The author William Styron (1992) wrote about his depression: "Like anyone else I have always had times when I felt deeply depressed, but this was something altogether new in my experience-a despairing, unchanging paralysis of the spirit beyond anything I had ever known or imagined could exist. When people develop a depressive disorder, their heads may reverberate with self-recriminations. Like Mary, described in the Clinical Case, they may become focused on their flaws and deficits. Paying attention can be so exhausting that they have difficulty absorbing what they read and hear. When people become utterly dejected and hopeless, thoughts about suicide are common. Physical symptoms of depression are also common, including fatigue and low energy as well as physical aches and pains. These symptoms can be profound enough to convince afflicted persons that they must be suffering from some serious medical condition, even though the symptoms have no apparent physical cause. Although people with depression typically feel exhausted, they may find it hard to fall asleep and may wake up frequently. At least five symptoms (counting sad mood and loss of pleasure): · Sleeping too much or too little · Psychomotor retardation or agitation · Weight loss or change in appetite · Loss of energy · Feelings of worthlessness or excessive guilt · Difficulty concentrating, thinking, or making decisions · Recurrent thoughts of death or suicide Symptoms are present nearly every day, most of the day, for at least 2 weeks. Symptoms are distinct and more severe than a normative response to significant loss. Thoughts and movements may slow for some (psychomotor retardation), but others cannot sit still-they pace, fidget, and wring their hands (psychomotor agitation). Here, we focus on major depressive disorder and persistent depressive disorder, because both diagnoses are well researched. We will briefly discuss a newly defined diagnosis specific to children and adolescents, disruptive mood dysregulation disorder, in Focus on Discovery 13. We will not discuss premenstrual dysphoric disorder because so little is known about it. These symptoms must include either depressed mood or loss of interest and pleasure. Even though episodes tend to dissipate over time, an untreated episode may stretch on for 6 months or even longer. Major depressive episodes often recur-once a given episode clears, a person is likely to experience another episode. To estimate the course of disorder, researchers have used representative community samples (rather than patient samples, which may have a more severe course of disorder). About 4050% of people who recovered from a first episode of major depression experienced at least one Some people with depression have trouble falling asleep and more episode across the 10 years of follow-up (Eaton, Shao, staying asleep. In addition to these mood changes, they have at least two of the other symptoms of depression. The central feature of this diagnosis is the chronicity of symptoms, which is a stronger predictor of poor outcome than the number of symptoms. At least two of the following during that time: · Poor appetite or overeating · Sleeping too much or too little · Low energy · Poor self-esteem · Trouble concentrating or making decisions · Feelings of hopelessness the symptoms do not clear for more than 2 months at a time. This may be an underestimate because researchers asked people to recall depressive episodes that happened anytime in their life, and people may forget episodes of depression that happened many years ago (Moffitt, Caspi, et al. About 5 percent of people report experiencing depressive episodes that persisted for more than 2 years (Murphy & Byrne, 2012). It is tempting to assume that differences in prevalence rates by country indicate a strong role for culture. It turns out that differences among countries in rates of depression may be fairly complex. One out of every five women will experience an episode of depression during her lifetime. The gender gap typically begins to emerge during early adolescence and is fully present by late adolescence (Avenevoli, Swendsen, et al. Some of you might wonder if these findings just reflect a tendency for men not to disclose symptoms. Several factors may help explain this gender difference (Hilt & Nolen-Hoeksema, 2014): Biological Factors · Fluctuations in gonadal hormones, experienced at puberty, premenstrually, postpartum, and at menopause, may increase stress reactivity for some women. This may explain only a small portion of the gender difference, as hormone findings are mixed. Social Factors · Twice as many girls as boys are exposed to childhood sexual abuse. Stress Reactivity Factors · Acceptance of traditional social roles among girls may intensify self-critical attitudes about appearance. More specifically, women tend to spend more time ruminating about sad moods or wondering about why unhappy events have occurred. Men tend to spend more time using distracting or action-focused coping, such as playing a sport or engaging in other activities that shake off the sad mood. Men are more likely than women to become depressed after life events involving financial or occupational stress, whereas women are more likely than men to become depressed after interpersonal life events (Kendler & Gardner, 2014). At that time, young women encounter many stressors and more pressure concerning social roles and body image, and they tend to ruminate about the resulting negative feelings. In considering these issues, bear in mind that men are more likely to demonstrate other types of disorders, such as alcohol and substance abuse as well as antisocial personality disorder (Seedat, et al. Hence, understanding gender differences in psychopathology is likely to require attending to many different risk factors and syndromes. Rates of winter depression, or seasonal affective disorder, are higher farther from the equator, where winter days are shorter. Income disparity also appears to be tied to a much higher prevalence of depression (Pickett & Wilkinson, 2010). Undoubtedly, other cultural factors, such as family cohesion and mental health stigma, play an important role in rates of depression as well. The symptom profile of a depressive episode also varies across cultures, and one likely reason is the differences in cultural standards regarding expression of emotional distress. In the most common form of seasonal affective disorder, depressive episodes occur during the winter. These winter depressions appear to be much more common in northern than in southern climates; whereas less than 2 percent of people living in sunny Florida report these patterns, about 10 percent of people living in New Hampshire report seasonal affective disorder (Rosen, Targum, et al. For mammals living in the wild, a slower metabolism in the winter could have been a lifesaver during periods of scarce food. For some unlucky humans, though, this same mechanism might contribute to seasonal affective disorder. It is believed that seasonal affective disorder is related to changes in the levels and timing of melatonin release in the brain. Melatonin is exquisitely sensitive to light and dark cycles and is only released during dark periods. People with seasonal affective disorder show greater changes in nightly melatonin levels in the winter than do people without seasonal affective disorder (Wehr, Duncan, et al. Factors other than melatonin also are likely to contribute to seasonal mood shifts; for example, people with seasonal affective disorder show a change in their retinal sensitivity to light that appears to be genetically guided (Roecklein, Wong, et al. Hibernation in animals typically involves sleeping long hours, along with lowered appetite and energy. Indeed, even among those who do not develop seasonal affective disorder, sleep, appetite, and energy changes are very common responses to the shortened days of winter. For example, faced with a lack of energy to tackle new projects, some people may be more prone to feeling guilt. Those who are self-critical and troubled by other forms of negative cognitions Clinical Descriptions and Epidemiology of Depressive Disorders may be particularly likely to develop the full constellation of depressive symptoms in the face of the seasonal shifts in energy, sleep, and appetite (Whitcomb-Smith, Sigmon, et al. Fortunately, several treatment options are available for seasonal affective disorder. Like other subtypes of depression, seasonal affective disorder responds to antidepressant medications and cognitive behavioral therapy (Rohan, Roecklein, et al. Winter blues, though, are as likely to remit with 30 minutes 125 of bright light each morning as with fluoxetine (Prozac) (Lam, Levitt, et al. Many high-quality studies support bright light as a treatment for seasonal affective disorder (Golden, Gaynes, et al. Intriguingly, light therapy has been shown to help relieve depression even among those without a seasonal pattern to their depressions (Lam, Levitt, et al. Among persons who are seeking treatment for depression, ethnic minorities in the United States, as well as people from Latin American and some Asian countries, tend to focus on their somatic symptoms, such as fatigue and pain (Bagayogo, Interian, & Escobar, 2013). Some cultures may stigmatize psychological syndromes, such as depression, more than physical health concerns. Even though these theories may help explain the pattern, some have suggested that this profile may be specific to patient samples. When representative community samples from Eastern and Western countries are asked about each depressive symptom carefully, there are more parallels than distinctions in the way that people from different countries describe their depressive symptoms (Kim & López, 2014). Other common comorbid conditions include substance-related disorders, sexual dysfunctions, and personality disorders. From the depths of a depression, getting to work may require overwhelming effort, parenting can feel like a burden, and suicide can seem like an option. There is particularly strong evidence that depression is related to the onset and more severe course of cardiovascular disease (Carney & Freedland, 2017). Depression is related to a more than twofold increase in the risk of death from cardiovascular disease, even after controlling for baseline cardiovascular health (Meijer, Conradi, et al. Chronic depressive symptoms persist on average for 10 years (Klein & Kotov, 2016). Functioning declines as depressive symptoms persist for more years (Klein, Shankman, & Rose, 2006). Depressive disorders include major depressive disorder and persistent depressive disorder as well as two more recently recognized disorders: premenstrual dysphoric disorder and disruptive mood dysregulation disorder. Major depression is characterized by severe episodes lasting at least 2 weeks, whereas persistent depressive disorder is characterized by symptoms that last at least 2 years.
She would not even go to the supermarket for fear of having to interact with people erectile dysfunction doctor delhi cheap adcirca 20 mg. This fear made her so nervous that she would often stammer or forget what she was going to say while talking to others impotence 16 year old purchase adcirca 20 mg fast delivery, thus adding to her apprehension that others would see her as stupid and creating a vicious circle of ever-increasing fear erectile dysfunction meds list adcirca 20 mg purchase without a prescription. Clinical Descriptions of the Anxiety Disorders 167 Social anxiety disorder generally begins during adolescence erectile dysfunction causes uk adcirca 20 mg purchase line, when peer relationships become particularly important erectile dysfunction johnson city tn purchase adcirca no prescription. Without treatment, social anxiety disorder tends to be chronic (Bruce, Yonkers, et al. A panic attack is a sudden attack of intense apprehension, terror, and feelings of impending doom, accompanied by at least four other symptoms. Physical symptoms can include shortness of breath, heart palpitations, nausea, upset stomach, chest pain, feelings of choking and smothering, dizziness, lightheadedness, faintness, sweating, chills, heat sensations, numbness or tingling sensations, and trembling. Not surprisingly, people often report that they have an intense urge to flee whatever situation they are in when a panic attack occurs. The symptoms tend to come on very rapidly and reach a peak of intensity within 10 minutes. Many people seek emergency medical care when they first experience a panic attack because they are terrified that they are having a heart attack. As noted above, we can think about a panic attack as a misfire of the fear system: physiologically, the person experiences a level of sympathetic nervous system arousal matching what most people might experience when faced with an immediate threat to life. Because the symptoms are inexplicable, the person tries to make sense of the experience. A person who begins to think that he or she is dying, losing control, or going crazy is likely to feel even more fear. Among people with panic disorder, 90 percent report just these types of beliefs when panic attacks occur. The diagnostic criteria for panic disorder require more than the presence of recurrent panic attacks. Panic attacks that are triggered by specific situations, such as seeing a snake, are typically related to a phobia and should not be considered in diagnosing panic disorder. Hence, in making this diagnosis, the response to panic attacks is as important as the attacks themselves. Remember that the criteria for panic disorder specify that panic attacks must be recurrent. It is fairly common for people to experience a single panic attack- more than a quarter of people in the United States report that they have experienced at least one panic attack during their lifetime (Kessler, Chiu, et al. The symptoms of panic disorder tend to wax and wane over time (Nay, Brown, & Roberson-Nay, 2013). It can take a heavy toll; for example, as many as one-quarter of people with panic disorder are unemployed for more than 5 years (Leon, Portera, & Weissman, 1995). Agoraphobia Agoraphobia (from the Greek agora, meaning "marketplace") is defined by anxiety about situations in which it would be embarrassing or difficult to escape if anxiety symptoms occurred. Commonly feared situations include crowds and crowded places such as grocery stores, malls, and churches. Sometimes the People with panic disorder often seek cardiac tests because they are frightened by changes in their heart rate. As a consequence of their fear of these situations, many people with agoraphobia are virtually unable to leave their house, and even those who can leave do so only with great distress. About half of people with agoraphobia symptoms experience panic attacks (Andrews, Charney, et al. The effects of agoraphobia on quality of life are as severe as those observed for the other anxiety disorders (Wittchen, Gloster, et al. The term worry refers to the cognitive tendency to chew on a problem and to be unable to let go of it (Mennin, Heimberg, & Turk, 2004). Often, worry continues because a person cannot settle on a solution to the problem. I had a prestigious job, loyal friends, a good apartment I shared with a bright and beautiful girlfriend, and as much money as I needed. I slept fitfully, with recurring nightmares-tsunamis, feral animals, the violent deaths of loved ones. I had made the wrong decisions, gone down the wrong path, screwed up in a ruinous, irrevocable, epoch-making way. He was visibly distressed during the entire initial interview, with a furrowed brow and continuous fidgeting. Although he first described worries about his health, a picture of pervasive anxiety soon emerged. He reported that he nearly always felt tense and he seemed to worry about everything. He was apprehensive of disasters that could befall him as he interacted with people and worked, and he described worrying much of the time about his finances, his inability to establish a romantic relationship, and other issues. He reported a long history of difficulties relating to others, which had led to his being fired from several jobs. As he put it, "I really like people and try to get along with them, but I fly off the handle too easily. Comorbidity in Anxiety Disorders More than half of people with one anxiety disorder meet the criteria for another anxiety disorder during their lives (Wright, Krueger, et al. Anxiety disorders are also highly comorbid with other disorders: Three-quarters of people with an anxiety disorder meet the diagnostic criteria for at least one other psychological disorder (Kessler, Chiu, et al. More specifically, about 60 percent of people in treatment for anxiety disorders meet the diagnostic criteria for major depression. Obsessive compulsive disorder also commonly co-occurs with anxiety disorders (Wright et al. As with many disorders, comorbidity is associated with greater severity and poorer outcomes of the anxiety disorders (Bruce et al. Quick Summary As a group, anxiety disorders are the most common type of psychological disorder. Large-scale epidemiological studies suggest that 28 percent of people will experience an anxiety disorder during their lifetime, and some research suggests that this may be an underestimate. Specific phobia is defined by an intense fear of an object or situation, social anxiety disorder by an intense fear of strangers or social scrutiny, panic disorder by anxiety about recurrent panic attacks, agoraphobia by a fear of places where escaping or getting help would be difficult if anxiety symptoms were to occur, and generalized anxiety disorder by worries lasting at least six months. People with one anxiety disorder are very likely to experience a second anxiety disorder during their lives. About 60 percent of people with anxiety disorders will experience major depression during their lives. In epidemiological studies that conduct just one interview with people about whether they met diagnostic criteria for an anxiety disorder, the estimated lifetime prevalence of anxiety disorders is:. As you will see, however, there are still some puzzles about why these patterns exist. Gender Women are more vulnerable to anxiety disorders than are men, with several studies documenting a 2 to 1 gender ratio (Baxter, Scott, et al. When present, anxiety disorders also appear related to more functional impairment for women compared with men (McLean, Asnaani, et al. For example, men may experience more social pressure than women to face fears-as you will see below, facing fears is the basis for one of the most effective treatments available. Men may be raised to believe more in their personal control over situations as well. It also appears that women show more biological reactivity to stress than do men (Olff, Langeland, et al. Culture People in every culture seem to experience problems with anxiety disorders, but culture and environment influence what people come to fear (Kirmayer, 2001). Gender and Cultural Factors in the Anxiety Disorders 171 Kayak-angst, a disorder that is similar to panic disorder, occurs among the Inuit people of western Greenland; seal hunters who are alone at sea may experience intense fear, disorientation, and concerns about drowning. Several cultural concepts of distress (see Chapter 3) provide examples of how culture and environment may shape the expression of an anxiety disorder. For example, in Japan a syndrome called taijin kyofusho involves fear of displeasing or embarrassing others; people with this syndrome typically fear making direct eye contact, blushing, having body odor, or having a bodily deformity. Perhaps this focus is related to characteristics of traditional Japanese culture that encourage deep concern for the feelings of others. As with the Japanese syndrome taijin kyofusho, the objects of anxiety and fear in these syndromes relate to environmental challenges as well as to attitudes that are prevalent in the cultures where the syndromes occur. Beyond cultural concepts of distress, the prevalence of anxiety disorders varies across cultures. This is not surprising given that cultures differ with regard to factors such as stress levels, the nature of family relationships, and the prevalence of poverty-all of which are known to play a role in the occurrence of anxiety disorders. Cultural attitudes may also guide how comfortable people are with disclosing psychological symptoms. Countries with recent war, revolution, or large-scale persecution have higher rates of anxiety disorders than do those without such conDisorders with symptoms similar to panic attacks occur crossculturally. For some time, researchers have thought that people from different cultures express symptoms of psychological distress and anxiety in different ways. For example, many thought that those from some cultures, and particularly those with a strong belief in mind-body connections, would express their emotional concerns through somatic complaints, but it now seems that this conclusion might reflect sampling problems-that is, researchers often studied anxiety and depression in psychological clinics in the United States but in medical clinics in other cultures. One can imagine that a person seeing a medical doctor might be likely to emphasize somatic concerns! Indeed, many people, regardless of culture, tend to describe anxiety and depression initially in terms of bodily sensations when visiting a medical clinic. When researchers interview people in similar settings and ask specifically about psychological concerns, the ratio of somatic to psychological symptoms expressed appears to be much more similar across cultures (Kirmayer, 2001). Culture influences the focus of fears, the ways that symptoms are expressed, and even the prevalence of different anxiety disorders. Common Risk Factors Across the Anxiety Disorders As we consider risk factors associated with anxiety disorders, we begin by describing a set of factors that seem to increase risk for all of the anxiety disorders. The existence of such risk factors may help explain why people with one anxiety disorder are likely to develop a second one-that is, some risk factors increase the odds of having more than one anxiety disorder. For example, the factors that increase risk for social anxiety disorder may also increase risk for panic disorder. Unlike the way we have organized most of the other chapters in this book, we have chosen to begin here with the behavioral model. We do this because classical conditioning of a fear response is at the heart of many anxiety disorders. Many of the other risk factors, including genes, neurobiological correlates, personality traits, and cognition, influence how readily a person can be conditioned to develop a new fear response. Taken together, the risk factors combine to create an increased sensitivity to threat (Craske, Rauch, et al. Fear Conditioning Earlier we mentioned that most anxiety disorders involve fears that are more frequent or intense than what most people experience. Through operant conditioning (also discussed in Chapter 1), this avoidant response is maintained because it is reinforcing (it reduces fear). In step 2, the man reduces his fear by avoiding dogs as much as possible; the avoidant behavior is reinforced by the reduction in fear. First, many people who have anxiety disorders cannot remember any exposure to a threatening event that triggered their symptoms. Second, many people who do experience serious threats do not develop anxiety disorders. Several extensions of this model, which we look at next, have been developed that explain these gaps. According to this extension, classical conditioning could occur in different ways (Rachman, 1977), including: · Direct experience (like the dog bite in the example above) · Modeling. That is, some people are more vulnerable to developing anxiety disorders than others. Researchers have shown in carefully controlled tests in laboratory settings that people with anxiety disorders are more responsive to threats, and they have measured this in many different ways. Most centrally, people with anxiety disorders seem to acquire fears more readily through classical conditioning, and those fears are more persistent once conditioned (Craske et al. After receiving six shocks, most participants learned to fear the the idea that modeling plays a role in the Rorschach card, as measured by skin conductance responses to seeing the card- etiology of phobias. However, participants with and without an anxiety disorder (in this study, panic disorder) differed in the Step 1 Classical conditioning extinction phase of the study, when the card was shown without any shock being provided. Thus, a perconditioned Linked by fear of dogs son with an anxiety disorder may find that once a fear is condiStrong fear contiguous tioned, that fear stubbornly persists and is difficult to unlearn in motivates the pairing(s) person to spite of evidence to the contrary. People with anxiety disorders also appear to experience certain types of threats as particularly powerful. One body of research suggests that people with anxiety disorders are particularly sensitive to unpredictable, as compared with predictable, threats. Knowing when that conversation will occur reduces anxiety compared with being faced with the idea that the person could show up anytime, anyplace! People with anxiety disorders, though, are particularly sensitive to this unpredictability. The threat in the predictable and unpredictable threat condition is the same-for example, participants could receive identical electric shocks in both threat conditions. The difference is that in the predictable threat condition, it is clear when the threat will happen, but in the unpredictable threat condition, the timing of the threat is unclear. Response to the three conditions is usually measured by psychophysiological indices of arousal (Schmitz & Grillon, 2012). Of the three experimental conditions, anxiety disorders are specifically related to increased affective and psychophysiological response to the unpredictable threat condition compared with the predictable threat condition. This profile appears to be specific to anxiety disorders, in that people with major depressive disorder respond like healthy controls do to unpredictable threat (Gorka, et al.
A person with this symptom may stare vacantly impotence kegel exercises buy discount adcirca, the muscles of the face motionless impotence workup cheap adcirca 20 mg line, the eyes lifeless erectile dysfunction massage techniques purchase adcirca 20 mg. When spoken to how young can erectile dysfunction start discount adcirca 20 mg buy, the person may answer in a flat and toneless voice and not look at his or her conversational partner erectile dysfunction and diabetes a study in primary care order adcirca line. Over 20 different studies have shown that people with schizophrenia are much less facially expressive than are people without schizophrenia; this is true in daily life or in laboratory studies when emotionally evocative stimuli (films, pictures, foods) are presented. However, people with schizophrenia report experiencing the same amount or even more emotion than people without schizophrenia (Kring & Elis, 2013). Alogia ThinkStock/Superstock People with schizophrenia who have blunted affect may not outwardly show happiness, but they will feel it as strongly as people who smile. A person may answer a question with one or two words and will not be likely to elaborate on an answer with additional detail. For example, if you ask a person with alogia to describe a happy life experience, the person might respond "getting married" and then fail to elaborate even when asked for additional information. Although we have just described five different negative symptoms, research suggests that these symptoms can be understood more simply as representing two domains (Blanchard & Cohen, 2006; Kring, Gur, et al. The first domain, involving motivation, emotional experience, and sociality, is sometimes referred to as the motivation and pleasure domain. The second domain, involving outward expression of emotion and vocalization, is referred to as the expression domain. Disorganized Symptoms Disorganized symptoms include disorganized speech and disorganized behavior. Disorganized Speech Also known as formal thought disorder, disorganized speech refers to problems in organizing ideas and in speaking so that a listener can understand. The following excerpt illustrates the incoherence sometimes found in the conversation of people with schizophrenia as an interviewer tries to ask John, a person with schizophrenia, several questions. Clinical Descriptions of Schizophrenia 251 Interviewer: Have you been nervous or tense lately Although John may make repeated references to central ideas or themes, the images and fragments of thought are not connected; it is difficult to understand what he is trying to tell the interviewer. Speech may also be disorganized by what are called loose associations, or derailment, in which case the person may be more successful in communicating with a listener but has difficulty sticking to one topic. Steve Lopez, a reporter for the Los Angeles Times, befriended a man with schizophrenia named Nathaniel in the L. Lopez wrote about their friendship in the book the Soloist (see photo) (Lopez, 2008). Disorganized Behavior People with the symptom of disorganized behavior may go into inexplicable bouts of agitation, dress in unusual clothes, act in a silly manner, hoard food, or collect garbage. They seem to lose the ability to organize their behavior and make it conform to community standards. People with this symptom may gesture repeatedly, using peculiar and sometimes complex sequences of finger, hand, and arm movements, which often seem to be purposeful. Some people manifest an unusual increase in their overall level of activity, including much excitement, flailing of the limbs, and great expenditure of energy similar to that seen in mania. At the other end of the spectrum is immobility: people adopt unusual postures and maintain them for very long periods of time. Catatonia is seldom seen today in people with schizophrenia, perhaps because medications work effectively on these disturbed movements or postures. Kraepelin first described dementia praecox, his term for what we now call schizophrenia, in 1898. Although people with dementia praecox were symptomatically diverse, Kraepelin believed that they shared a common core. The term dementia praecox reflected what he believed was that core-an early-onset (praecox) and a progressive, inevitable intellectual deterioration (dementia). The dementia in dementia praecox is not the same as the dementias we discuss in the chapter on neurocognitive disorders (Chapter 14). Thus, the label "dementia praecox" was no longer appropriate, and in 1908 Bleuler proposed his Emil Kraepelin (18561926), a own term, schizophrenia, German psychiatrist, articulated from the Greek words descriptions of schizophrenia schizein ("to split") and (then called dementia praecox) phren ("mind"), capturthat have proved remarkably ing what he viewed as durable in light of contemporary the essential nature of research. Hulton Archive/Getty Images Bleuler used a metaphor-the "breaking of associative threads" to describe the essential features of schizophrenia. Thus, goal-directed, efficient thinking and communication were possible only when these hypothetical structures were intact. The notion that associative threads were disrupted in people with schizophrenia could then be used to account for the range of other symptoms. Kraepelin had recognized that a small percentage of people with symptoms of dementia praecox did not deteriorate, but he preferred to limit this diagnostic category to people who had a poor prognosis. He diagnosed some people with a good prognosis as having schizophrenia, and he also diagnosed schizophrenia in many people who would have received different diagnoses from other clinicians. De Agostini Picture Library/Getty Images Eugen Bleuler (18571939), a Swiss psychiatrist, contributed to our conceptions of schizophrenia and coined the term. The symptoms of schizophreniform disorder are the same as those of schizophrenia but last only 1 to 6 months. Brief psychotic disorder lasts from 1 day to 1 month and is often brought on by extreme stress, such as bereavement. Schizoaffective disorder comprises a mixture of symptoms of schizophrenia and mood disorders. These can be delusions of persecution or jealousy, such as the unfounded conviction that a spouse or lover is unfaithful. Other delusions seen in this disorder include grandiose delusions, delusions of erotomania (believing that one is loved by some other person, usually a complete stranger with a higher social status), and somatic delusions. These types of studies are called clinical high-risk studies, and the starting point for these prospective, longitudinal studies is the reliable identification of youth who present with mild positive symptoms that might later develop into schizophrenia (Miller, McGlashan, et al. Research has identified groups of young people who differ from people without these mild symptoms and from people who have a family history of schizophrenia (people studied in familial high-risk studies). Such people have been referred to as prodromal; the word prodrome refers to the early signs of a disease. Young people who show these mild symptoms differ from young people who do not in several domains, including their everyday functioning and their rate of conversion to schizophrenia spectrum disorders (Woods, Addington, et al. Between 10 and 30 percent of people meeting prodromal criteria develop a schizophrenia spectrum disorder compared with only 0. Unfortunately, under the current health insurance system in the United States, people often cannot get treatment unless they have an official diagnosis. However, there were also several arguments against adding this new category (Yung et al. Third, there is concern that applying a new diagnostic label, particularly to young people, might be stigmatizing or lead to discrimination. Finally, although providing treatment for people with distressing or disabling attenuated positive symptoms is a laudable goal, the treatment may too closely resemble that for schizophrenia, further blurring the line between the two conditions. It affects men slightly more than women and typically begins in late adolescence or early adulthood. Positive symptoms include hallucinations and delusions; negative symptoms include avolition, alogia, blunted affect, anhedonia, and asociality. Together, the negative symptoms represent two domains: motivation/pleasure and expression. Other schizophrenia spectrum disorders include schizophreniform disorder and brief psychotic disorder, which differ from schizophrenia in duration. Schizoaffective disorder involves symptoms of both schizophrenia and either a depressive or manic episode. The category of attenuated psychosis syndrome, which involves positive symptoms in attenuated form that cause distress and have worsened in the past year, needs additional study. He particularly liked to see horror movies because they made him feel really scared. In his movie the Dark Knight, his battles with the Joker were a signal that he was prepared to fight for them to be together. That he signed autographs at his movie opening also told her that he was trying to get in touch with her. She reasoned that these dinners were always the same food and conversation, so why bother Later in the week, her mother mentioned that Sophia was not doing much around the house. He talked about having dry mouth and then immediately began talking about cottonmouth snakes and jungle safaris and how hiking was good for your health but that Barack Obama was in better shape than George Bush. Etiology of Schizophrenia What can explain the scattering and disconnection of thoughts, delusions, hallucinations, and diminished motivation and emotion expression of people with schizophrenia Genetic Factors A good deal of research supports the idea that schizophrenia has a genetic component, as we discuss in the following sections on behavior genetics and molecular genetics research. The evidence is somewhat more convincing from behavior genetics studies, largely because they have been well replicated (see Chapter 4 on the importance of replication). Current evidence indicates that schizophrenia is genetically heterogeneous-that is, genetic factors may vary from case to case-mirroring the fact, noted earlier, that schizophrenia is symptomatically heterogeneous. As is the case for any gene or genes, they do their work via the environment, so geneenvironment interaction studies are likely to help pinpoint the nature of the genetic contribution to schizophrenia (Walker, Mittal, & Tessner, 2008). Behavior Genetics Research Family, twin, and adoption studies (described in Chapter 4) support the idea that genetic factors play a role in schizophrenia. Many behavior genetics studies of schizophrenia were conducted when the definition of schizophrenia was considerably broader than it is now. However, behavior genetics investigators collected extensive descriptive data on their samples, allowing the results to be reanalyzed later using newer diagnostic criteria. Other studies have found that people with schizophrenia in their family histories have more negative symptoms than those whose families are free of schizophrenia (Malaspina, Goetz, et al. A family study examined over 2 million people from Denmark from the Danish Civil Registration System (Gottesman, Laursen, et al. This system records all inpatient and outpatient admissions for health-related issues, including psychological disorders. The researchers examined the cumulative incidence of schizophrenia and bipolar disorder among people with one, two, or no biological parents who had been admitted for treatment for schizophrenia or bipolar disorder. They also examined the incidence of these disorders among children who had one parent admitted for schizophrenia and one parent admitted for bipolar disorder. As you might expect, the incidence of schizophrenia was highest for children who had two parents admitted for schizophrenia. The incidence of schizophrenia was also higher for people with one parent admitted for schizophrenia and one parent admitted for bipolar disorder compared with those people who had just one parent admitted for schizophrenia. These findings suggest that there may be some shared genetic vulnerability between schizophrenia and bipolar disorder; molecular genetics studies, which we turn to shortly, also suggest this link. Family studies show that genes likely play a role in schizophrenia, but of course the relatives of a person with schizophrenia share not only genes but also common experiences. Therefore, the influence of the environment cannot be discounted in explaining the higher risks among relatives. Twin study research also suggests that negative symptoms may have a stronger genetic component than do positive symptoms (Dworkin, Lenzenwenger, & Moldin, 1987; Dworkin & Lenzenwenger, 1984). In one rare case, all of the Genain quadruplet girls (not pictured), born in 1930, developed schizophrenia. Two of the still surviving sisters were recently evaluated at age 81, and both were still taking antipsychotic medication (Mirsky, Bieliauskas, et al. A clever analysis supporting a genetic interpretation of the high risk found for identical twins was performed by Fischer (1971). She reasoned that if these rates indeed reflected a genetic effect, the twins without schizophrenia would presumably carry risk genes for schizophrenia, even though it was not expressed behaviorally, and thus might pass along an increased risk for the disorder to their children. Both rates are substantially higher than the 1 percent prevalence found in the general population, which lends further support to the importance of genetic factors in schizophrenia. Adoption Studies the study of children whose biological mothers had schizophrenia but who were reared from early infancy by adoptive parents without schizophrenia is another useful behavior genetics study method. Such studies eliminate the possible effects of being reared in an environment where a parent has schizophrenia. In a now-classic study, Heston (1966) followed up 47 people born between 1915 and 1945 to women with schizophrenia who were raised by adoptive parents who did not have schizophrenia. Fifty control participants were selected from the same adoption agency that had placed the children of the women with schizophrenia. The follow-up assessment revealed that none of the controls was diagnosed with schizophrenia, versus 10. Another large study of adopted offspring of mothers with schizophrenia found similar results. In this study, the risk for developing schizophrenia or a related diagnosis among the 164 adoptees who had a biological mother with schizophrenia was 8. Familial High-Risk Studies A different type of family study is called the familial high-risk study. The first familial high-risk study of schizophrenia was begun in the 1960s (Mednick & Schulsinger, 1968). The high-risk participants were 207 young people whose mothers had schizophrenia; the low-risk participants were similar in all respects to the high-risk group except that their mothers did not have schizophrenia. In 1972, the now-grown men and women were followed up with several measures, including a battery of diagnostic tests. Fifteen of the high-risk participants were diagnosed with schizophrenia; none of the control participants were so diagnosed. Mednick Sarnoff Mednick, a psychologist at the University of Southern California, pioneered the use of the familial high-risk method for studying schizophrenia. He has also contributed to the hypothesis that a maternal viral infection is implicated in this disorder. Etiology of Schizophrenia 257 In the wake of this pioneering study, other familial high-risk investigations were undertaken. The New England Family Study found that children of a parent (mother or father) with a schizophrenia spectrum disorder were six times more likely to develop a schizophrenia spectrum disorder by age 40 than children without a parent with schizophrenia (Goldstein, Buka, et al.
Adcirca 20 mg order fast delivery. ED Series: What's the best drug for Erectile Dysfunction? Obsidian Men's Health in Tysons Corner Va.
References
- Jorgensen H, Wetterslev J, Moiniche S, Dahl JB. Epidural local anaesthetics versus opioid-based analgesic regimens on postoperative gastrointestinal paralysis, PONV and pain after abdominal surgery. Cochrane Database Syst Rev 2000(4):CD001893.
- Sheets NC, Goldin GH, Meyer AM, et al. Intensity-modulated radiation therapy, proton therapy, or conformal radiation therapy and morbidity and disease control in localized prostate cancer. JAMA 2012;307(15):1611-1620.
- Moerman N, Bonke B, Oosting J: Awareness and recall during general anesthesia. Facts and feelings, Anesthesiology 79:454-464, 1993.
- Jacobs BL, Kaufman SR, Morgenstern H, et al: Trends in the treatment of adults with ureteropelvic junction obstruction, J Endourol 27(3):355, 2013.
- Gold MS, Gebhart GF. Nociceptor sensitization in pain pathogenesis. Nat Med 2010; 16:1248-57.
- Rinaldo P, O'Shea JJ, Welch RD, et al. Stable isotope dilution analysis of n-hexanoylglycine, 3-phenylpropionylglycine and suberylglycine in human urine using chemical ionization gas chromatography/mass spectrometry selected ion monitoring. Biomed Environ Mass Spectrom 1989;18:471.
- Greenblatt DY, Rajamanickam V, Pugely AJ, et al. Short-term outcomes after laparoscopic-assisted proctectomy for rectal cancer: results from the ACS NSQIP. J Am Coll Surg 2011;212(5):844-854.
- Verbiest, H. (1954). Radicular syndromes from developmental narrowing of the lumbar spinal canal. Journal of Bone and Joint Surgery, 36B, 230n237.