- info@careermakers.edu.np
- +977 1 4423870
Clozapine
Spyridon Stavros Marinopoulos, M.B.A., M.D.
- Director, University Health Services
- Assistant Professor of Medicine
https://www.hopkinsmedicine.org/profiles/results/directory/profile/0017097/spyridon-marinopoulos
The organism also appears with a single mood disorder bipolar 2 discount clozapine online, black nucleus and a thick anxiety jittery feeling clozapine 50 mg buy visa, slightly asymmetric depression hurts test clozapine 100 mg buy low cost, refractile wall mood disorder therapy discount clozapine 50 mg mastercard. It grows on most routine mycologic media depression definition in history cheap 100 mg clozapine with amex, but cycloheximide will suppress growth of Prototheca spp. The use of fluorescent antibody reagents permits the rapid and reliable identification of Prototheca spp in culture and tissue. Voriconazole, posaconazole, itraconazole, and fluconazole have been successful in individual cases. As host immunity develops, the skin test becomes positive, and the number of organisms on biopsy diminishes. Age: About 25% of scrofuloderma cases and most cases of lichen scrofulosorum occur in children. Nutritional status: Tuberculous abscesses and scrofuloderma are associated with malnutrition. Unfortunately, unlike in Hansen disease, these categories do not correlate perfectly to host immunity. The test becomes positive 210 weeks after infection and remains positive for many years, although it may wane with age. The intradermal, or Mantoux, test is the standard and offers the highest degree of consistency and reliability. If induration is more than 15 mm, it is positive in all others; 0- to 4-mm induration is negative. Reactivity to the tuberculin protein is impaired in certain conditions in which cellular immunity is impaired. Results are variable with respect to the sensitivity and specificity of these assays, but they are valuable in certain settings. Disseminated infection is seen in 14 cases per 1 million infants vaccinated and is associated with high mortality. Lupus vulgaris can occur rarely at the vaccination site or at a distant site and will respond to appropriate antituberculous treatment. Clinically, the lesion begins as a small papule, which becomes hyperkeratotic, resembling a wart. The inoculation can occur during tattooing, medical injections, nose piercing, or external physical trauma. The earliest lesion, appearing 24 weeks after inoculation, is a painless brown-red papule that develops into an indurated nodule or plaque that may ulcerate. Prominent regional lymphadenopathy appears 38 weeks after infection and, occasionally, suppurative and draining lesions may appear over involved lymph nodes. Primary tuberculous complex occurs on the mucous membranes in about one third of patients. Spontaneous healing usually occurs within 1 year, with the skin lesion healing first, then the lymph node, which is often persistently enlarged and calcified. Simultaneously, with the appearance of epithelioid cells, the number of tubercle bacilli decreases rapidly. Lupus vulgaris may appear at sites of inoculation, in scrofuloderma scars, or most frequently at distant sites from the initial infectious focus, probably by hematogenous dissemination. Lupus vulgaris typically is a single plaque composed of grouped red-brown papules, which, when blanched by diascopic pressure, have a pale, brownish yellow or "apple jelly" color On dermoscopy a yellowish-orange patch may indicate the presence of dermal granulomas secondary to lupus vulgaris, sarcoidosis, a foreign body reaction, or cutaneous leishmaniasis. Lesions are almost always solitary, and regional adenopathy is usually present only if secondary bacterial infection occurs. Local scarring, as seen in lupus vulgaris, can occur Although sometimes separated by exudative or suppurative areas, the lesions seldom ulcerate and may heal spontaneously. Histologically, there is pseudoepitheliomatous hyperplasia of the epidermis and hyperkeratosis. Suppurative and granulomatous inflammation is seen in the upper and middle dermis, sometimes perforating through the epidermis. It must also be distinguished from North American blastomycosis, chromoblastomycosis, verrucous epidermal nevus, hypertrophic lichen planus, halogenoderma, and verruca vulgaris. Multiple erythematous papules in a generalized distribution appear a month or more after the illness. These lesions evolve to small papules and plaques, clinically and histologically resembling lupus vulgaris. Uniform hyperplasia of the ear pinna and lobe may closely mimic "turkey ear," as described in sarcoidosis. When the mucous membranes are involved, the lesions become papillomatous or ulcerative. On the tongue, irregular, deep, painful fissures occur, sometimes associated with microglossia to the degree that nutrition is compromised. The rate of progression of lupus vulgaris is slow, and a lesion may remain limited to a small area for several decades. In some patients, the lesions become papillomatous, vegetative, or thickly crusted, with a rupioid appearance. Caseation within the tubercles is seen in about half the cases and is rarely marked. Colloid milia, acne vulgaris, sarcoidosis, and rosacea may simulate lupus vulgaris. Differentiation from tertiary syphilis, chronic discoid lupus erythematosus, Hansen disease, systemic mycoses, and leishmaniasis may be more difficult, and biopsy and tissue cultures may be required. The disease is destructive, frequently causes ulceration, and on involution leaves deforming scars as it slowly spreads peripherally over the years. Lupus vulgaris lesions of the head and neck can be associated with lymphangitis or lymphadenitis in some cases. If lesions involve the nose or the earlobes, these structures are shrunken and scarred, as if nibbled away. The tip of the nose may be sharply pointed and beaklike, or the whole nose may be destroyed, with only the orifices and the posterior parts of the septum and turbinates visible. The upper lip, a site of predilection, may become diffusely swollen and thickened, with fissures, adherent thin crusts, and ulcers. On the trunk and extremities, lesions may be annular or serpiginous or may form gyrate patterns. On the hands and feet and around the genitals or buttocks, lesions may cause mutilation by destruction, scar formation, warty thickenings, and elephantiasic enlargement. Scrofuloderma is tuberculous involvement of the skin by direct extension from an underlying focus of infection. It occurs most frequently over the cervical lymph nodes but also may occur over bone or around joints if these are involved. Clinically, the lesions begin as subcutaneous masses, which enlarge to form nodules. They may be erythematous or skin colored, and usually the skin temperature is not increased over the mass. Surgical procedures may incite lesions of scrofuloderma over joints or the abdominal cavity, apparently by releasing the loculated focus and contaminating the track along which instruments are inserted. Scrofuloderma heals with characteristic cordlike scars, frequently allowing the diagnosis to be made many years later. Histologically, in scrofuloderma, the tuberculous process begins in the underlying lymph node or bone and extends through the deep dermis. At the periphery, more typical ok sf re Cutaneous Tuberculosis From Endogenous Source by Direct Extension (Scrofuloderma and Periorificial Tuberculosis). Scrofuloderma should be differentiated from atypical mycobacterial infection, sporotrichosis, actinomycosis, coccidioidomycosis, and hidradenitis suppurativa. Lesions ulcerate from the beginning and extend rapidly, with no tendency to spontaneous healing. Classically, this begins with a distal lesion, and new lesions appearing more proximally. Less often, a proximal lesion is present initially, and new lesions appear distally (retrograde lymphatic spread). Lesions are symmetrically distributed on the extensor extremities, especially on the tips of the elbows and on the knees; dorsal surfaces of the hands and feet; buttocks; face and ears; and glans penis. Two thirds of cases occur before age 30, and females are affected 3: 1 over males. Associated clinical phenomena have included tuberculous arteritis with gangrene in young adult Africans and development of lupus vulgaris from the lesions. A palisaded collection of histiocytes surrounds an ovoid or wedge-shaped area of dermal necrosis. Well-formed ubercles are not seen, except in nonhealing lesions evolving into lupus vulgaris. Vascular changes are prominent, ranging from a mild lymphocytic vasculitis to fibrinoid necrosis and thrombotic occlusion of vessels. This is not a neutrophilic leukocytoclastic vasculitis, but rather a chronic granulomatous, small-vessel vasculitis. Tuberculids represent cutaneous lesions induced by hematogenous dissemination of tubercle bacilli to the skin Lupus vulgaris may develop at the sites of tuberculids, and M. This results in rapid destruction of the bacilli and autoinvolution of individual lesions in many cases. New lesions continue to appear, however, because hematogenous dissemination from the underlying focus continues. Tuberculids tend to be bilaterally symmetric eruptions because they result from hematogenous dissemination. Tuberculous mastitis may closely resemble breast cancer, so biopsies are frequently done. The consequence of the ongoing inflammation, destroying the fat of the breast, and the surgical procedures can be a severely disfigured breast. Less often, a string of deep nodules may become fluctuant, drain to the surface, or ulcerate, forming linear scrofuloderma-like lesions. The draining lymph node may be enlarged (more often than in sporotrichoid atypical mycobacterial infection). The lesions are 24 mm, follicular or parafollicular, and yellow-pink to reddish brown. They are firm and flat topped or surmounted by a tiny pustule or thin scale the lesions are arranged in nummular or discoid groups, where they persist unchanged for months and cause no symptoms. Histologically, lichen scrofulosorum shows noncaseating tuberculoid granulomas just beneath the epidermis, between and surrounding hair follicles. Normally, tubercle bacilli are not seen in the pathologic specimens and cannot be cultured from biopsy material. Lichen nitidus, lichen planus, secondary syphilis, and sarcoidosis should be considered in the differential diagnosis. They resolve spontaneously, with or without ulceration, over several months and can heal with scarring. In addition, a granulomatous vasculitis of arterioles can be present in the fat and is the apparent cause of the fat necrosis. Biopsies of nodular granulomatous phlebitis show thrombosis of and granulomatous inflammation centered around veins in the deep dermis. The histology of nodular tuberculid may be identical or very similar to polyarteritis nodosa. Erythema induratum must be distinguished from erythema nodosum, nodular vasculitis, polyarteritis nodosa, tertiary syphilis, and other infectious and inflammatory panniculitides. Erythema nodosum is of relatively short duration, develops rapidly, and chiefly affects the anterior rather than the posterior calves. It produces tender, painful, scarlet or contusiform nodules that appear simultaneously and do not ulcerate. In erythema induratum patients, the pain is less severe, and the lesions tend to evolve serially or in crops. A syphilitic gumma is usually unilateral and single or may appear as a small, distinct group of lesions. Three-drug or four-drug regimens are usually recommended for initial empiric treatment. Failure to respond within this period should result in reconsideration of the diagnosis, assessment for compliance, and concern about drug resistance. Culture remains the gold standard and provides the means to determine antibiotic sensitivity and response to treatment. An updated evidence-based assessment of the value of screening and monitoring tests when using systemic biologic agents to treat psoriasis and psoriatic arthritis. Cantini F, et al: Guidance for the management of patients with latent tuberculosis infection requiring biologic therapy in rheumatology and dermatology clinical practice. Kumar U, et al: Psoriasiform type of lichen scrofulosorum: Pediatr Dermatol 2011; 28: 532. Liu Y, et al: Analysis of 30 patients with acupuncture-induced primary inoculation tuberculosis. Medicine (Baltimore) 2017; 95: e5875 Pescitelli L, et al: Tuberculosis reactivation risk in dermatology. Regnier S, et al: Cutaneous military resistant tuberculosis in a patient infected with human immunodeficiency virus. Singal A, et al: Ulcerated lupus vulgaris at the site of bacille Calmette-Guérin vaccination. Identification of specific Mycobacterium species is now made using molecular techniques; however, the growth rates have some utility in considering a practical classification.
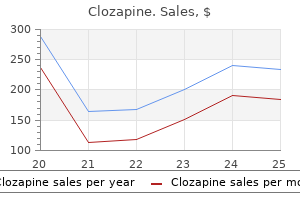
Four main subtypes of Sweet syndrome have been described depression test francais buy discount clozapine 25 mg on-line, based on their pathogenesis: the classic type (majority of cases) bipolar depression 0f 100 mg clozapine purchase amex, cases associated with neoplasia (3%35% of cases) mood disorder treatment centers cheap clozapine online, cases associated with inflammatory disease (3%16%) depression economic buy clozapine 100 mg with mastercard, and cases associated with pregnancy (1%4%); druginduced cases exist as well (1%26%) mood disorder centre hong kong effective clozapine 100 mg. The primary skin lesion is a sharply marginated, rapidly extending, tender, erythematous or violaceous, painful, elevated plaque, 210 cm in diameter. The surface of the plaques may develop pseudovesiculation or pustulation as a result of an intense dermal ee ne oo ks sf fre e fre. Clinical morphologic variants more recently described include immunocompromised patients with deep necrosis simulating necrotizing fasciitis and patients whose lesions were extremely large and described as giant cellulitislike in appearance. Other ocular manifestations include periorbital inflammation, dacryoadenitis, limbal nodules, peripheral ulcerative keratitis, glaucoma, iritis, and choroiditis. Oral lesions resembling aphthae occur in 2% or 3% of classic cases, but in 10% or more of those associated with hematologic malignancy. Pulmonary infiltrates and effusions are often seen on chest radiographs of such patients. Qiao J, et al: Flame figures associated with eosinophilic dermatosis of hematologic malignancy Int J Clin Exp Pathol 2013; 6: 1683. Rajpara A, et al: Recurrent paraneoplastic Wells syndrome in a patient with metastatic renal cancer. Laboratory findings include an elevated sedimentation rate (90%), neutrophilia (70%), leukocytosis (60%), and a left shift (increased bands; 50%). Persistent cases, with new lesions erupting before the old lesions resolve, may continue for many years. The histologic hallmark of Sweet syndrome is a nodular and diffuse dermal infiltrate of neutrophils with karyorrhexis and massive papillary dermal edema. Leukocytoclastic vasculitis may be present focally, and this does not exclude a diagnosis of Sweet syndrome. Leukemic cells may be present in the infiltrate, and clonal restriction of neutrophils has even been seen in Sweet syndrome not associated with malignancy. Histologic variants described as histiocytic or lymphocytic Sweet syndrome have been reported. These entities are somewhat controversial, as Sweet syndrome is by definition a neutrophilic dermatosis. Occasionally, the main infiltrating cell resembles histiocytes, but in some studies with immunohistochemical stains, they are found to be immature myeloid cells, with positive myeloperoxidase stains. Patients with histiocytoid Sweets are more likely to have an underlying hematologic disorder or malignancy concurrent or shortly after the diagnosis is made. Other associated conditions include infections with Yersinia, toxoplasmosis, histoplasmosis, salmonellosis, tuberculosis, tonsillitis, vaccination, and vulvovaginal infections. Hematologic malignancies or solid tumors are present in about 10% (3%35% range) of reported cases. Sweet syndrome often presents early in the course of the cancer, but may present months to years before a diagnosis of malignancy is made. Sweet syndrome may occur with myelodysplastic syndromes or with hemoproliferative malignancies including leukemias (usually acute myelogenous) and lymphomas. Solid tumors are of any type but are most often genitourinary, breast (in women), or gastrointestinal (in men). Anemia is found in 93% of men and 71% of women with malignancy-associated Sweet syndrome. Thrombocytopenia is seen in half Solitary, bullous, or ulcerative lesions are more frequently associated with malignancy, as is the histiocytoid histopathologic pattern. Pregnancy-associated Sweet syndrome typically presents in the first or second trimester with lesions on the head, neck, trunk, and less often on the upper extremities. The condition may resolve spontaneously or clear with topical or systemic corticosteroids. It may recur with subsequent pregnancies, but there seems to be no risk to the fetus. Induction of the skin lesions appears to be related to the desired pharmacologic effect of the medication. The two major criteria for the diagnosis of Sweet syndrome are the presence of red edematous plaques and a biopsy demonstrating neutrophils, karyorrhexis, and marked papillary dermal edema. Minor criteria include associated symptoms or conditions, laboratory findings, and response to therapy. Patients should have both major criteria and two of the four minor criteria for diagnosis (Box 7. Sweet syndrome is a diagnosis of exclusion, and often tissue culture is necessary to exclude infection. Bowel bypass syndrome has skin lesions that, on histologic examination, are identical to those of Sweet syndrome; fever and arthritis also accompany bowel bypass syndrome. In both, fever and arthritis may occur, along with leukocytosis with neutrophilia. A search for an underlying cause should be undertaken, especially in persons over age 50 and those with anemia, thrombocytopenia, histiocytoid pathology, or lesions that are bullous or necrotic. The standard treatment is systemic corticosteroids, with approximately 12 mg/kg/day of oral prednisone this will result in resolution of fever and skin lesions within days. Topical or intralesional steroids may be tried for mild disease but are often ineffective. Abnormal laboratory findings 3 of the following: · Erythrocytesedimentationrate>20 mm/hr · C reactiveproteinelevated · Leukocytosis>8000/mm3 · Leftshiftwith>70% neutrophils 4. Histologically, papillary dermal edema and a nodular and diffuse neutrophilic infiltrate with karyorrhexis are noted Leukocytoclastic vasculitis may be present focally. Cheraghi N, et al: Azathioprine hypersensitivity presenting as neutrophilic dermatosis and erythema nodosum. Costa-Silva M, et al: Neutrophilic dermatosis of the dorsal hands: a restrictive designation for an acral entity. Small red papules expand to urticarial, targetoid plaques with hypopigmented centers. Histologic evaluation of the skin lesions usually shows a neutrophilic dermatosis virtually identical to Sweet syndrome. The lesions resolve with destruction of the elastic tissue at the site, producing soft, wrinkled, skin-colored protuberant plaques that can be pushed into the dermis. Elastic tissue in other organs may also be affected, especially the heart and lungs. There are five clinical subtypes, with ulcerative the most common; others include bullous, vegetative, pustular, and peristomal. Approximately 20% 30% of patients may exhibit pathergy, development of lesions from mild trauma. Satellite violaceous papules may appear just peripheral to the border of the ulcer and break down to fuse with the central ulcer, or multiple small erosions may develop concurrently and run together, resembling "cheese cloth" initially. These lesions have considerable overlap with "bullous Sweet syndrome" and are usually seen in patients with hematologic disorders (leukemia or myelodysplasia), and some argue whether these patients should not simply be diagnosed with Sweet syndrome. Lesions present as chronic, superficial, cribriform ulcerations, usually of the trunk, that enlarge slowly and have elevated borders and clean fre fre fre. Ghoufi L, et al: Histiocytoid Sweet syndrome is more frequently associated with myelodysplastic syndromes than the classical neutrophilic variant. Peroni A, et al: Histiocytoid Sweet syndrome is infiltrated predominantly by M2-like macrophages. The lesions are rarely painful, generally respond to relatively conservative treatments, and are usually not associated with under ying systemic disease. As the lesions evolve, they demonstrate suppurative inflammation in the dermis and subcutaneous fat. Massive dermal edema and epidermal neutrophilic abscesses are present at the violaceous, undermined border. Clinical and pathologic correlation, coupled with extensive testing to exclude alternative etiologies, is essential. The initial workup of the patient includes studies necessary to ensure that the proper diagnosis is made, as well as to investigate possible associated diseases. Multiple infections, including mycobacteria, deep fungi, gummatous syphilis, sy ergistic gangrene, and amebiasis, must be excluded with cultures and special studies. The clinical lesions may be strikingly similar, evolving from small papulopustules to form ulcerations that do not heal. Histologic evaluation will often simply show suppurative dermatitis, because the injected or applied caustic substance may not be identifiable (urine, disinfectants, drain cleaner). Pyoderma gangrenosum may be misdiagnosed as a spider bite if there is only a solitary lesion on an extremity. Spider bites tend to evolve more rapidly and may be associated with other systemic symptoms or findings, such as disseminated intravascular coagulation. Local treatment includes both proper wound care and medication to reduce inflammation; compresses or whirlpool baths are followed by the use of ointment or hydrophilic occlusive dressings. In solitary lesions or slowly progressive cases, application of potent topical corticosteroids, intralesional steroid injections, topical dapsone, or topical tacrolimus may be beneficial, although pathergy may be seen at sites of injection. The absorption of tacrolimus in large or multiple wounds may lead to systemic blood levels. Systemic corticosteroids can be extremely effective, with initial doses in the range of 12 mg/kg. Infliximab has been shown to be effective in randomized trials, and is given in doses of about 5 mg/kg at weeks 0, 2, and 6 and then every 68 weeks. Sulfapyridine, sulfasalazine, salicylazosulfapyridine dapsone, methotrexate, azathioprine, and minocycline generally are somewhat less effective but may be useful adjuncts or tried for patients with either mild disease, or contraindications/ comorbidities that preclude more po ent agents. Patients typically show response within 12 weeks of initiation of therapy, with reduced pain, decreased exudate, and less erythema and edema. Often patients have a large wound, but the inflammation is under control-ongoing high-dose immunosuppression may not be necessary in these cases. Optimal wound care is essential, including compression if edema is present, though caution should be used to avoid compression-induced pathergy. Most wound care consists of keeping the wound clean and avoiding colonization, biofilm, or infection; Vaseline and impregnated nonstick gauze may help avoid trauma with dressing changes. Alginates or other absorptive dressings may be required for very exudative wounds. Pathergy is rarely noted at the donor site when patients are receiving adequate immunosuppressive therapy. These generally cause hereditary periodic fevers along with clinical and laboratory evidence of inflammation. Peritonitis, pleuritis, arthritis, and vasculitis, including Henoch-Schönlein purpura, may also occur in these patients, who usually present before the teenage years. Febrile episodes of 13 weeks are accompanied by periorbital edema, abdominal pain, myalgia, and a painful, distally migrating erythematous or urticarial-like plaques often overlying areas of myalgia. Bone lesions, oral ulcers, and other findings are all reversed dramatically by anakinra, though steroids and traditional psoriasis treatments, including retinoids, have been used. Two thirds of patients manifest various morbilliform or urticarial eruptions and may develop aphthous stomatitis or genital ulcerations. Familial cold autoinflammatory syndrome is characterized by fever, cold urticaria, conjunctivitis and arthralgia elicited by generalized exposure to cold. Patients with Muckle-Wells syndrome manifest most often in adolescence with acute febrile inflammatory episodes comprising abdominal pain, arthritis, urticaria, hearing loss, and multiorgan amyloidosis. Neonatal-onset multisystem inflammatory disease is characterized by fever, chronic meningitis, uveitis, sensorineural hearing loss, urticarial rash, and a deforming arthritis. Patients may also have dysmorphic facial appearance, clubbing of the fingers, mild mental retardation, and papilledema. Blau syndrome is an autosomal dominant disease with arthritis, uveitis, granulomatous inflammation, and camptodactyly. This disease was dubbed "neutrophilic urticaria with systemic inflammation," which is differentiated from prior reports of neutrophilic urticaria. These are very rare, but the list of identified gene mutations and syndromes is growing. Clearing of the central region may occur, and lesions may coalesce, producing an annular or polycyclic pattern. When angioedema is not present, and fever, malaise, and joint/bone pain coexist, an autoinflammatory or autoimmune condition should be considered. Chia J, et al: Failure to thrive, interstitial lung diseases, and progressive digital necrosis with onset in infancy. Jain A, et al: Vasculitis and vasculitis-like manifestations in monogenic autoinflammatory syndromes. Rheumatol Int 2017; ePub Manthiram K, et al: the monogenic autoinflammatory diseases define new pathways in human innate immunity and inflammation. Patients present in the newborn period with fever; swollen purplish red eyelids; red and purplish papules and plaques of the trunk, neck, and extremities; and lipodystrophy of the face, along with other systemic findings. The skin biopsy most often reveals a predominant neutrophilic perivascular and interstitial infiltrate, although about one third of cases are mononuclear. In some patients, the IgM gammopathy progresses to neoplasia, especially Waldenström macroglobulinemia. Effective therapy for patients with Schnitzler syndrome has included anakinra, rituximab, tocilizumab, rilonacept, and canakinumab. Acute urticaria evolves over days to weeks, producing evanescent wheals that, individually, rarely last more than 12 hours, with complete resolution of the urticaria within 6 weeks of onset. Daily episodes of urticaria and/or angioedema lasting more than 6 weeks are designated chronic urticaria. Chronic urticaria predominantly affects adults and is twice as common in women as in men.
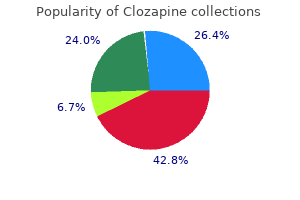
Other associated changes may be seen depression symptoms in guys buy cheap clozapine 100 mg online, such as increased inflammation depression test for disability generic clozapine 100 mg online, histiocytes depression economic purchase clozapine 100 mg line, parakeratosis bipolar depression en espanol clozapine 25 mg purchase amex, degenerated cells bipolar depression episode buy generic clozapine, and granular debris. I n atrophy, the basal cells may have an increased N /C ratio secondary to focal nuclear enlargement. I n addition, features such as hyperchromasia and nuclear membrane irregularities can be seen in benign atrophic samples, which may cause concern for squamous dysplasia. Atrophic squamous cells have dense cytoplasm F and enlarged nuclei (2-3 times the size of an intermediate cell nucleus) with high N /C ratios. The round uniform nuclei, retained polarity, and association with background single parabasal cells are a clue to the benign nature of a cluster of basal cells. This fragment has a syncytial appearance as the borders between cells are difficult to identify. The nuclei are small and uniform in size but are dark and have mild nuclear border irregularities. However, the nuclei in this fragment are well organized, and some cells have a reassuring amount of cytoplasm (Pap stain). The numerous squamous cells in this large fragment have indistinct cellular borders, making assessment of the nuclear to cytoplasmic (N/C) ratio difficult. The nuclei are somewhat dark but are uniform in size and have only mild nuclear contour irregularities; the nuclear to cytoplasmic (N/C) ratios are low. A n additional challenging problem in atrophic smears is the occasional presence of granular debris, acute inflammation, and apoptotic bodies. This cell and its pink cytoplasm, along with the presence of degenerated cells ("blue blobs") and granular material in the background, may cause initial concern for a keratinizing squamous cell carcinoma (Pap stain). Note the necrotic debris attached to viable tumor cells ("clinging diathesis") as well as present in the background. A single keratinizing cell with pink cytoplasm and an irregularly shaped, dark nucleus can be seen in the center of the field (Pap stain). A nswer: D istinguishing dysplasia within atrophic smears can be one of the most challenging diagnostic problems on the Pap test. The cells have high nuclear to cytoplasmic ratios, which is concerning despite the small nuclear sizes. Tubal Metaplasia O ccasionally, endocervical cells undergo tubal metaplasia and adopt the characteristics of the glandular cells lining the fallopian tubes. Most notably, these cells are columnar and characteristically contain a terminal bar with cilia at the luminal end. This fragment contains crowded, dark cells with enlarged nuclei and high nuclear to cytoplasmic (N/C) ratios. However, at the fragment edges, the columnar nature of the cells can be seen along with terminal bars and cilia. Once tubal metaplasia is identified in a specimen, one must consider whether other hyperchromatic crowded groups in a the specimen simply represent tubal metaplasia lacking identifiable cilia versus a second cell type. A strip of endocervical cells with basally oriented nuclei and ciliated terminal bars. Finding a field such as this can be reassuring if other fields contain metaplastic cells that appear more hyperchromatic and lack definitive cilia or terminal bars (Pap stain). I nconspicuous nucleoli may be seen on some preparations, although typically the chromatin has a powdery or coarse appearance. The chromatin is even but coarsely granular, giving a hyperchromatic appearance (Pap stain). The neoplastic cells in this small cluster have high nuclear to cytoplasmic ratios and overlapping nuclei. Note the marked variation in size and nuclear overlap seen in these cells (Pap stain). While the cells appear well organized within the tissue fragment, the projection of elongated nuclei beyond the fragment edge (creating a ragged appearance i. The cells have powdery, dark chromatin, anisonucleosis, and irregular nuclear contours. The nuclei palisade in some areas and are disorganized in other areas within the fragment (Pap stain). The cells are disorganized and have nuclear contour irregularities and anisonucleosis (Pap stain). Compare this fragment with the organized honeycomb pattern found in reactive endocervical cells. Here, the organized honeycomb arrangement is disrupted and nuclei project out from the fragment edges (Pap stain). Unlike what is seen in benign endocervical cells, the nuclei are located at different levels within the cytoplasm and appear pseudostratified (Pap stain). Note the irregular stratification of the nuclei within columnar cytoplasm (Pap stain). This group is hyperchromatic and crowded to a level where the cytomorphology is difficult to assess. Note the powdery appearance to the chromatin, which contains small coarse granules as well as smaller speckles (Pap stain). Key Features of Adenocarcinoma In Situ Columnar cells can be present in sheets, strips, or rosette formations. Nuclei are often irregularly stratified between adjacent cells ("pseudostratified" appearance), crowded, and overlapping. A denocarcinoma often have greater variation in nuclear size, irregularly coarse chromatin (or sometimes chromatin clearing), and marked nuclear contour irregularities. Features of invasive adenocarcinoma include the presence of necrosis (which may be seen as "clinging diathesis" on liquid-based preparations) and an increased number of sca ered single atypical cells. Note the marked overlapping of the cells and background of fibrinous material, which also clings to some of the cells ("clinging diathesis"). Note that at the periphery the cells have a wispy cytoplasm characteristic of endocervical origin. At the edges of the fragments, cytoplasm can be seen, indicating glandular differentiation. Key Features of Endocervical Adenocarcinoma Abnormal cells are often present in three-dimensional structures and/or singly dispersed. Nuclei are crowded, overlapping, enlarged, and hyperchromatic with coarse chromatin and prominent nucleoli. Clinging diathesis is indicative of invasion and is characterized by necrotic debris attached to the periphery of a group of malignant cells. Endometrial Adenocarcinoma Endometrial adenocarcinoma is the most common malignancy of the gynecologic tract. Endometrial cancer predominantly affects postmenopausal women in their sixth decade. The presence of endometrial carcinoma on a Pap test is associated with more advanced disease. The most common subtype is endometrioid adenocarcinoma, which has been associated with hyperestrogenism. Most commonly carcinoma appears as tight groups of haphazardly arranged, hyperchromatic cells with pleomorphic nuclei. The cells contain variable amounts of cytoplasm, and sca ered large cytoplasmic vacuoles are frequently seen. The presence of nucleoli is variable and ranges from inconspicuous to prominent, with prominent nucleoli generally associated with higher grade neoplasms. I ntracytoplasmic aggregates of neutrophils are commonly present ("bag of polys"). This fragment is three-dimensional and contains cells with enlarged nuclei, coarse chromatin, highly irregular nuclear contours, and high nuclear to cytoplasmic (N/C) ratios-all features of carcinoma. Some cells have a columnar shape and foamy cytoplasm, indicating a glandular origin. The presence of neutrophils within the fragment suggests but does not confirm an endometrial origin (Pap stain). This loosely cohesive cluster contains cells with large, irregular-s haped nuclei with coarse chromatin. Note the presence of intracytoplasmic neutrophils, which is characteristic of endometrial origin (Pap stain). Note the subtle clinging necrosis at the periphery of the cluster, associated with neutrophils. Reactive endometrial cells arising from endometrial polyps and other benign processes can also appear quite atypical; in equivocal cases. A small cluster of neoplastic endometrial cells with prominent nucleoli and intracytoplasmic neutrophils are seen in the center of this field (Pap stain). Key Features of Endometrial Adenocarcinoma Necrotic granular debris may be present in the background, indicating an invasive process, also known as diathesis. Nuclei are enlarged and hyperchromatic with coarse chromatin; nuclear pleomorphism increases with nuclear grade. Examination of three-dimensional, crowded clusters is challenging as the cells of interest shield one another from examination. The cells have high nuclear to cytoplasmic (N/C) ratios, anisonucleosis, and nuclear membrane irregularities. The cytoplasm is dense, favoring a squamous rather than glandular origin (Pap stain). The cells are hyperchromatic with high nuclear to cytoplasmic (N/C) ratios and marked nuclear border irregularities. The nuclei are also disorganized within the tissue fragment, a finding not seen in benign squamous metaplasia or reparative changes (Pap stain). The cells have highly irregular nuclear contours, which is further evidenced by the presence of nuclear grooves (Pap stain). These atypical squamous cells in this cluster demonstrate high nuclear to cytoplasmic (N/C) ratios, irregular nuclear membranes, and irregularly distributed chromatin (Pap stain). A cluster of atypical squamous cells with high nuclear to cytoplasmic (N/C) ratios, markedly irregular nuclear membranes, and coarse chromatin is seen adjacent to benign squamous cells (Pap stain). These atypical squamous cells have high nuclear to cytoplasmic (N/C) ratios, hyperchromasia, and nuclear membrane irregularities. The cells have dense cytoplasm and a small gap can be seen where the cells meet, suggesting that these cells may be atypical metaplastic cells. A small cluster of hyperchromatic cells with high nuclear to cytoplasmic (N/C) ratios and irregular nuclear membranes is seen. As is typically seen in carcinoma, the cells form a three-dimensional tissue fragment. The cells are hyperchromatic and have coarse chromatin, anisonucleosis, and irregular nuclear borders. The cytoplasm is polygonal and dense, favoring a squamous rather than glandular differentiation (Pap stain). Key Features of High-Grade Squamous Intraepithelial Lesion the lesional ells have scant cytoplasm and high N/C ratios. Nuclei are hyperchromatic an contain coarse chromatin with variable nuclear size and shape. Nonkeratinizing Squamous Cell Carcinoma Cervical cancer remains one of the main causes of death in women worldwide. Cervical cancer disproportionally affects women who do not have access to adequate screening programs and/or follow-up. This large fragment contains malignant cells with high N/C ratios, irregular nuclear borders, and anisonucleosis. Granular debris and neutrophils are present along some edges, suggesting the presence of necrosis. The amount of atypia is beyond what is seen in most high-grade squamous intraepithelial lesions (Pap stain). The fragment is also three-dimensional, a characteristic more commonly seen in carcinomas as compared to high-grade squamous intraepithelial lesions (Pap stain). Rare atypical cells with hyperchromasia, convoluted nuclear membranes, and coarse chromatin. The cells in this fragment have very dark nuclei and form a three-dimensional structure. The cells also have high N/C ratios, irregular nuclear contours, and anisonucleosis. The high level of atypia seen in this fragment, combined with the three-dimensional structure formed by these cells, favor a squamous cell carcinoma over a high-grade squamous intraepithelial lesion (Pap stain). Key Features of Nonkeratinizing Squamous Cell Carcinoma Hyperchromatic crowded groups contain malignant cells with prominent nucleoli and/or unevenly distributed, coarse chromatin. The malignant cells are pleomorphic and have dense, squamous cytoplasm and/or high N/C ratios (basaloid appearance). Tumor diathesis (necrotic debris) may be present as "clinging diathesis" in liquid-b ased preparations (necrotic debris adherent to cells). Glandular Pattern While the Pap test focuses primarily on the detection of squamous lesions, glandular cells are often present in Pap test specimens and may represent benign background cells as well as clinically important lesions. Therefore, the glandular component of a Pap test cannot be ignored and should be assessed as carefully as the squamous component. The presence or absence of glandular cells, specifically endocervical cells, is reported as a quality indicator in Pap test specimens, although the presence of glandular cells is not required for specimen adequacy. I n some instances, cells with squamous differentiation may have a glandular appearance, and this should be kept in mind when developing a differential diagnosis for atypical-appearing glandular cells. Endocervical cells may demonstrate marked reactive changes, resulting in strikingly enlarged nuclei. O n occasion, reactive endocervical cells may even become multinucleated (described below under the "Multinucleated Pa ern").
Buy clozapine 25 mg on line. 5 Types of Depressive Disorders.
References
- Goodstadt L, Ponting CP. Sequence variation and disease in the wake of the draft human genome. Hum Mol Genet 2001;10:2209-14.
- Bogart JA, Sagerman RH. High-dose hemithorax irradiation in a patient with recurrent thymoma: a study of pulmonary and cardiac radiation tolerance. Am J Clin Oncol 1999;22(5):441-445.
- Fang J, Alderman MH. Trend of stroke hospitalization, United States, 1988-1997.
- Toyoda K, Imamura T, Saku Y, et al. Medial medullary infarction: analyses of eleven patients. Neurology 1996;47(5):1141-7.
- Ginsberg, D., Huffman, J.L., Lieskovsky, G. et al. Urinary tract stones: a complication of the Kock pouch continent urinary diversion. J Urol 1991;145:956-959.
- Schulze M, Beck R, Igney A, et al. Computed tomography findings of human polyomavirus BK (BKV)-associated cystitis in allogeneic hematopoietic stem cell transplant recipients. Acta Radiol. 2008;49(10):1187-1194.
- Mehta S: Transtracheal illumination for optimal tracheal tube placement. A clinical study. Anaesthesia 44:970, 1989.
- Barbero-Marcial M, Verginelli G, Ward M, et al: Surgical treatment of Ebsteinis anomaly. J Thorac Cardiovasc Surg 1979; 78:416-422.