- info@careermakers.edu.np
- +977 1 4423870
Finasteride
Elizabeth Jones, MT, ABHI (CHT), ASPT (CPT)
- Instructor
- Medical Laboratory Program
- Community Technical and Adult Education Center
- Allied Health Department
- Ocala, Florida
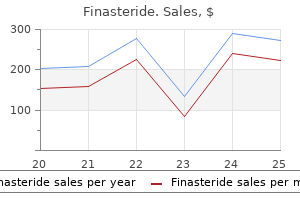
Higher doses of arginine may be employed in patients with citrullinemia and arginosuccinic aciduria and none in argininemia hair loss specialist buy generic finasteride canada. Water and electrolytes are provided intravenously hair loss herbs cheap 5 mg finasteride, and anabolism is promoted by the administration of glucose hair loss with lupus buy finasteride 5 mg low price. Pharmacologic approaches to therapy include the provision of arginine to keep the urea cycle supplied with sufficient ornithine to keep it running and the provision of alternate pathways for the excretion of waste nitrogen hair loss talk forum generic 5 mg finasteride mastercard, such as sodium benzoate and sodium phenylacetate/-butyrate hair loss cure 2015 images cheap finasteride 1 mg buy online. Extracorporeal methods, such as hemodialysis, are often required in the acutely hyperammonemic newborn. The most effective treatment of the acute hyperammonemic crisis that occurs in the classic neonatal disease is continuous veno-venous hemodiaflitration [811]. Exchange transfusion is not an effective modality in such an infant, but it may reduce levels sufficiently to buy some time while the hemodialysis is being prepared, and it has been effective in some patients with transient hyperammonemia of the newborn [3]. Peritoneal dialysis is sometimes recommended for hyperammonemic patients, and we would agree that it is effective in an older infant, child, or adult with hyperammonemia but, in our experience, it has been unsatisfactory in the neonatal period [12]. Hemodiaflitration and hemodialysis have been shown to be more effective than exchange transfusion, peritoneal dialysis or arteriovenous hemofiltration, but the logistics are such in most hospitals that this modality can seldom be mobilized promptly to meet the needs of a newly diagnosed newborn. This is an argument for early transport of such an infant to an institution with experience in the rescue of such infants. Even though continuous veno-venous hemodiaflitration is the optimal modality for extracorporeal ammonium detoxification [8], prognosis is not related to dialysis modality but primarily to the duration of coma before the start of treatment confirming the necessity for rapid and aggressive management. A number of patients with various urea cycle disorders have received partial or total orthotopic liver transplants to provide enzyme replacement or somatic gene therapy, respectively [14]. In all successful cases, this has cured the hyperammonemia and permitted a normal protein intake. However, its effectiveness is hampered by expense, limited availability of donor organs, and significant morbidity and mortality from complication of transplantation or immunosuppression. Liver transplantation does not normalize citrulline concentrations, which is primarily produced in the intestine; thus, following transplantation, supplementation with citrulline or arginine may need to be continued. Ideally, orthotopic liver transplantation should be carried out between 36 and 12 months of age before irreversible neurologic damage has occurred, in patients with severe neonatal-onset disease, and patients suffering from recurrent severe decompensations despite intensive medical treatment [9]. The pharmacologic approach to the provision of alternate methods of waste nitrogen excretion represents a major advance in the management of hyperammonemia (Table 25. The principle is that benzoate is effectively conjugated with glycine to form hippurate, which is efficiently excreted in the urine, and similarly phenylacetate is conjugated to form phenylacetylglutamine, and this compound is excreted in the urine; both provide pathways for getting rid of nitrogen that cannot be excreted as urea and would otherwise accumulate as ammonia. These measures have been employed along with exchange transfusion or peritoneal dialysis [3], but we have found pharmacologic therapy effective in patients in whom exchange transfusion and peritoneal dialysis were having little or no effect [6, 13]. This provides an essential amino acid in a patient with a complete block in arginine synthesis and provides ornithine substrate for any patient in whom there is not a complete block at carbamylphosphate synthetase or ornithine transcarbamylase. It may be particularly useful as an effector of acetylglutamate synthetase and hence activator of carbamylphosphate synthetase. It is particularly useful in patients with citrullinemia (Chapter 28) or argininosuccinic aciduria (Chapter 29). Supplies of benzoate, phenylacetate, and arginine should ideally be kept on hand and available to the neonatal intensive care unit in anticipation of the diagnosis of such an infant. Often, a patient is first recognized in a community hospital where benzoate and phenylacetate are not available, but arginine is. The arginine infusion should be started and the patient then transported to the tertiary care center. Operationally, for arginine as well as benzoate and/or phenylacetate, a priming infusion is followed by a regimen of continuous infusion until the ammonia has reached the normal range (Table 25. The use of mannitol for cerebral edema may also provide nitrogen excretion through diuresis in patients treated with benzoate, phenylacetate, and arginine. The pharmacologic regimen is started on diagnosis in the acute neonatal hyperammonemic crisis and can be pursued while the dialysis team is being assembled. It is usually effective in the management of recurrent episodes of hyperammonemia that occur in patients under therapy [9, 17] at times of infection or other cause of catabolism, or vomiting, leading to an inability to continue oral treatment, because therapy of these episodes is generally initiated more promptly. It is also true that many patients successfully treated initially have died in later episodes of intercurrent hyperammonemia. The ideal approach to management is very early diagnosis so that hyperammonemia is prevented or treated before there is major elevation of the serum concentration of ammonia. The drugs are supplied as concentrated solutions which would cause hyperosmolarity if infused directly. Later, the drugs are diluted in the 24-hour maintenance fluids, which are also 10% with respect to glucose, providing extra calories to spare catabolism. As the main concept for long-term management catabolism must be avoided as much as possible. In addition to intercurrent illnesses, especially if associated with high fever and decreased intake of food and fluids, very dangerous triggers are severe exercise, seizures, trauma, burns, steroid administration, chemotherapy, and gastrointestinal hemorrhage. Furthermore, drugs especially steroids, valproate, haloperidol and L-asparaginase/pegaspargase and the postpartum period (due to catabolism and the involution of the uterus) are important triggers for lateonset hyperammonemia [9]. The infant or child usually requires a combination of pharmacologic therapy and restriction of the intake of protein. Oral sodium phenylbutyrate has been employed as a source of phenylacetate in doses of 0. It may be used as a substitute for benzoate, but many of our patients have found it unpalatable. Also, phenylbutyrate may deplete branched chain amino acids levels and cause menstrual dysfunction/amenorrhea in up to 25% of postpubertal females [9]. Acute toxicity of benzoate and phenylbutyrate has been rare, but severe overdoses (2 to 10 times recommended) have led to symptoms that may be clinically mistaken for hyperammonemic episodes, including lethargy, hyperventilation, metabolic acidosis, cardiopulmonary collapse, and death [18]. Dietary treatment is an essential anchor point of long-term management and requires the knowledge of a specialist metabolic dietitian. For infants and older children, nutritional management involves the use of a high-caloric, low-protein diet supplemented with essential amino acids and, if necessary, vitamins and minerals. This is most readily accomplished by using small amounts of natural protein, an essential amino acids formula, and supplemental calories provided by a formula that does not contain protein. We have felt that the optimal intake of whole protein should be determined in each patient and have found supplementation with relatively small amounts of alanine to be effective [19], but in urea cycle defects, extra essential amino acids are often necessary. Especially in young infants and children, fasts should be avoided and snacks given to reduce the possibility of (overnight) catabolism. Periodic measurement of plasma amino acids (which include glutamine) and blood ammonia may permit adjustment of therapy before clinical symptoms appear. Chronic management of patients with urea cycle defects has also been effective using mixtures of the keto and hydroxy-acid analogs of essential amino acids [20]. These mixtures are no longer available in the United States, but there may still be a place for this anabolic approach to the removal of nitrogen, and long-term therapy in which keto acids were combined with benzoate in the successful treatment of a 30-month-old infant who at report was developing normally [15]. In this patient, nocturnal gavage was useful in the administration of the keto acids, arginine and benzoate. N-acetylglutamate is an essential cofactor of the carbamoyl phosphate synthase enzyme, and a small number of patients have been found with N-acetylglutamate synthase deficiency [21]. Carbamylglutamate is a structural analog of N-acetylglutamate, and Santiago Grisolía first suggested its use in hyperammonemia, caused by N-acetylglutamate synthetase deficiency (Nyhan, personal communication). This has turned out to be the case; treatment reduced levels of ammonia in the blood [22] and increased the incorporation of 15N-ammonium chloride into urea [23]. Carbamylglutamate has also been used successfully to treat the acute hyperammonemia of methylmalonic and propionic acidemia [24]. Inhibition of N-acetylglutamate synthase is the mechanism by which propionylCoA and similar compounds cause hyperammonemia [25]. Carbamylglutamate is available in Europe in 200 mg tablets for oral use, which limits its availability in acute hyperammonemic coma. In the chronic management of N-acetylglutamate synthetase deficiency, doses of 10100 mg/kg per day have been effective. This has slowly changed with the widespread availability of ammonia measurement in hospitals, growing knowledge about the disease and the use of alternate pathway therapy. A recent study demonstrated that the early-onset disease manifestation, a peak-blood ammonia level >1000 µmol/L and coma on admission are associated with the highest risk of mortality during a hyperammonemic episode [28]. Infants who are more than 5 days in hyperammonemic coma are invariably handicapped developmentally. While Bachmann suggested that neurocognitive outcome does essentially depend on the initial peak-blood ammonia level [31], surprisingly Ah Mew and coworkers could not correlate the peak-blood ammonia level with poor cognitive outcome [30]. Overall 214 Introduction to hyperammonemia and disorders of the urea cycle hyperammonemia and encephalopathy due to urea cycle disorders and organic acidemias. Treatment of inborn errors of urea synthesis: activation of alternative pathways of waste nitrogen synthesis and excretion. Restoration of urea genesis in N-acetylglutamate synthase deficiency by N-carbamylglutamate. Inhibition by propionylcoenzyme A of N-acetylglutamate synthetase in rat liver mitochondria. A possible explanation for hyperammonemia in propionic and methylmalonic acidemia. Kido J, Nakamura K, Mitsubuchi H, Long-term outcome and intervention of urea cycle disorders in Japan. Intellectual, adaptive, and behavioral functioning in children with urea cycle disorders. In this group, 18% died in the initial episode, but none once the diagnosis was established. Comparison of exchange transfusion, peritoneal dialysis and hemodialysis for the treatment of hyperammonemia in an anuric newborn infant. The management of life-threatening hyperammonemia: a comparison of several therapeutic modalities. Intestinal obstruction due to peritoneal adhesions as a complication of peritoneal dialysis for neonatal hyperammonemia. Onset is in the neonatal period with coma and/or convulsions, and in the absence of effective intervention, it is rapidly fatal. A sizable number of males have variant enzymes and a milder and later presentation, but hyperammonemia can still be fatal, even in adulthood. Females who have two X chromosomes have varying phenotypes mainly depending on the proportion of active and inactive X chromosomes. The enzyme is a trimer in which identical subunits have a molecular weight of about 38 kDa [2, 3]. The protein synthesized contains an N-terminal signal peptide that is specifically recognized by a receptor complex in the outer mitochondrial membrane [4]. After translocation across the membranes, proteolytic processing by two peptidases yields the mature protein [5]. Defective activity of the enzyme is readily demonstrable in a biopsied liver [6, 7]. The gene on the X-chromosome codes for the precursor protein that is imported after translation into mitochondria. The genes for glycerol kinase, adrenal insufficiency, chronic granulomatous disease, Norrie disease, and retinitis pigmentosa are all in this area, and a number of contiguous gene syndromes have resulted from deletions. Patients with these large deletions may have up to five severe genetic diseases making them extremely difficult to manage [10]. Many other mostly private point mutations have established an enormous heterogeneity. The site of a Tenckoff catheter that had been unsuccessfully used for peritoneal dialysis is evident on the abdomen. According to new data, this accounts for approximately one third of all patients respectively 50 percent of males with this disease [1517]; however, neonatal-onset male patients might be underrepresented in statistical analyses because of early and undiagnosed death. Prior to the development of pharmacologic approaches to the removal of waste nitrogen using benzoate and phenylacetate, this disorder was always fatal and usually within just a few days of birth. Occasionally, the diagnosis of hyperammonemia is made once blood culture is found to be negative. On the other hand, we have encountered neonates with urea cycle defects who have actually had sepsis, further confusing the diagnosis. The infant appears normal at birth and remains so during a period of hiatus, which may be as short as a few hours and is seldom longer than 48 hours. Grunting or rapid respirations may occur, and there may be a respiratory alkalosis. The infant may have hypertonia, but there is progression to a deep coma that is indistinguishable from surgical anesthesia. Ultimately, the infant stops breathing, and unless intubated and artificially ventilated, he dies. Despite initial improvement following dialysis or other interventions, which decrease ammonia concentrations, most of these patients have died [17]. Those surviving because of successful pharmacologic therapy have usually had severely impaired mental development, if the initial hyperammonemic coma has been profound and prolonged. Most have had recurrent hyperammonemic crises at times of catabolism induced by intercurrent illness, and each further episode appears to worsen the prognosis for mental development. In a few successfully managed patients, there were subsequent early liver transplantations, which prevent further metabolic decompensations. Patients who survive the neonatal attack remain at high risk of dying in infancy in a subsequent hyperammonemic episode that accompanies an acute infection. Levels found in the classic neonatal form of the disease are usually over 700 µmol/L (1000 µg/dL). In infants dying of the disease, levels may range from 400 to 1700 µmol/L (6002500 µg/dL). In the presence of levels over 300 µmol/L (500 µg/dL), one sees fixed dilated pupils and complete apnea. Normal neonatal ammonia is <100 µmol/L, but levels up to 180 can be observed in sick infants without an inherited metabolic disease.
Whenever possible hair loss magnesium cheap finasteride on line, the least restrictive methods should be used to de-escalate aggressive behavior hair loss jared gates finasteride 1 mg purchase without a prescription, or to calm agitated or disruptive individuals hair loss jared gates cheap finasteride 5 mg mastercard, such as a quiet and low-stimulation environment hair loss in men messenger finasteride 1 mg buy fast delivery, reasonable bargaining hair loss mirena 5 mg finasteride purchase visa, redirection of the patient, involvement of family, reality orientation, talk down, or a show of force. It is a gray area, indeed, as to when, or to what extent, any intervention is considered necessary to restrain a patient, or to protect a patient or medical personnel from harm. Effective measures are usually initiated by the emergency physician because psychiatric evaluation on such short notice is impractical or unavailable and important decisions must be made immediately with limited data. In that study there was a reduction in personnel injury rates and the contention that one suicide was averted. Standards for restraint and seclusion: Joint Commission on Accreditation of Healthcare Organizations. Fassler D, Cotton N: A national survey on the use of seclusion in the psychiatric treatment of children. Zun lS: A prospective study of the complication rate of use of patient restraint in the emergency department. Joint Commission on Accreditation of Healthcare Organizations: Preventing Restraint Deaths, 1998. A series of 30 cases from the Dade and Broward County Florida Medical Examiner Offices from 1982 to 1990. Ross Dl: An analysis of in-custody deaths and positional asphyxiation, Police Marksman 1996; March/April:1618. Khan A, levy P, DeHorn S, et al: Predictors of mortality in patients with delirium tremens. Sorrentino A: Chemical restraints for the agitated, violent, or psychotic pediatric patient in the emergency department: controversies and recommendations. Thomas H, Jr, Schwartz E, Petrilli R: Droperidol versus haloperidol for chemical restraint of agitated and combative patients. Battaglia J, Moss S, Rush J, et al: Haloperidol, lorazepam, or both for psychotic agitation Breier A, Meehan K, Birkett M, et al: A double-blind, placebo-controlled dose-response comparison of intramuscular olanzapine and haloperidol 1498. Meehan K, Zhang F, David S, et al: A double-blind, randomized comparison of the efficacy and safety of intramuscular injections of olanzapine, lorazepam, or placebo in treating acutely agitated patients diagnosed with bipolar mania. Spina E, de leon J: Metabolic drug interactions with newer antipsychotics: a comparative review. Reich Dl, Silvay G: Ketamine: an update on the first twenty-five years of clinical experience. Bourgoin A, Albanese J, Wereszczynski N, et al: Safety of sedation with ketamine in severe head injury patients: comparison with sufentanil. Melamed E, Oron Y, Ben-Avraham R, et al: the combative multitrauma patient: a protocol for prehospital management. Alexander J, Tharyan P, Adams C, et al: Rapid tranquillisation of violent or agitated patients in a psychiatric emergency setting. Martel M, Sterzinger A, Miner J, et al: Management of acute undifferentiated agitation in the emergency department: a randomized double-blind trial of droperidol, ziprasidone, and midazolam. Zimbroff Dl: Pharmacological control of acute agitation: focus on intramuscular preparations. Brook S: Intramuscular ziprasidone: moving beyond the conventional in the treatment of acute agitation in schizophrenia. Kaloostian P, Tran H: Intracranial taser dart penetration: literature review and surgical management. In addition to medical management, troubleshoot the device and remove it in cases of uncertainty or emergency. To remove the catheter, simply peel off the adhesive and embedded catheter together to discontinue the flow of injected medication into the patient. There are a variety of proprietary pump manufacturers, each with their own device programming. Peabody n addition to cardiac pacemakers and defibrillators, a number of noncardiac devices have been developed for electronic neuromodulation and drug delivery. By 2007, there were more than 375,000 external insulin infusion pumps in use in the United States. Ziconotide is a non-opioid calcium channel blocker, but its use may be complicated by confusion, somnolence, and other neurologic side effects. Although limited data demonstrate efficacy of intrathecal morphine and ziconotide in relieving refractory pain69 and efficacy of intrathecal baclofen in reducing spinal cord injury-induced spasticity,10 more quality clinical evidence is needed. Other medications used include bupivacaine, hydromorphone, fentanyl, sufentanil, clonidine, midazolam, and meperidine. There is minimal data comparing various medications and current regimens have been empirically derived. For intrathecal morphine infusions, approximately 1% of the total daily morphine dose is a standard starting point. Such small intrathecal doses reduce systemic concentrations and minimize side effects. The implanted catheter site varies, but it is commonly placed in the subcutaneous tissue of the abdomen in adults and the buttocks in young children. Similar findings were reported in a 2014 prospective study, in which the most clinically significant adverse events related to insulin infusion devices were hyperglycemia and ketosis. In 29 deaths, problems with the device that were identified included overinfusion, bent cannulas, disconnection, pump alarming, failure to deliver, suspected electromagnetic interference, and display failure. To discontinue the flow of insulin into the patient, simply peel off the adhesive and embedded catheter together. B, the pump is usually implanted in a subcutaneous pocket in a lower abdominal quadrant, with the catheter tunneled subcutaneously to an appropriate lumbar interspace. Severe and difficult to treat withdrawal may occur if opioids or baclofen infusions are interrupted by a drained drug reservoir or pump malfunction. Normal refill intervals vary based on usage, typically on the order of every few months. To place an intrathecal catheter, a small incision is made in the back and the catheter tip is placed into the cerebrospinal fluid. The catheter is then tunneled around the abdomen, placed in the lower abdominal wall, and attached to the subcutaneous pump. The pump has a port in the center that can be accessed by a needle placed through the skin. Continuous infusion devices, such as those made by Codman, are regularly refilled via manual bolus injections. Programmable devices are interrogated and programmed via an external manufacturer-specific device. Internal device programming errors that cause underdosing or overdosing are less common. If the drug supply is depleted, systemic symptoms related to acute drug withdrawal will occur. This is characteristic for the specific drug being delivered and should be anticipated. Although respiratory depression is uncommon, ziconotide may be associated with rare cases of rhabdomyolysis and psychosis. It is more common to have an underdose of medication due to pump malfunction or a break or dislodgement of the catheter than to have an overdose. In patients experiencing opioid, baclofen, or other medication withdrawal, treatment may be quite difficult because large doses of systemic medications are required to equal the effects of intrathecal medications. Acute intrathecal baclofen withdrawal, which may resemble alcohol or benzodiazepine withdrawal can be serious and difficult to manage. As withdrawal is due to loss of medication at the spinal level, it may not be possible to safely deliver enough 1. Palpate and locate the pump on the patient (typically in the lower abdominal subcutaneous layer). Attach the 20-ml syringe to the 22-gauge needle and insert the needle through the skin into the center of the reservoir fill port until the needle touches the metal needle stop. Intrathecal drug delivery systems vary in their reservoir capacity from 15 to 50 ml. A propofol infusion has been suggested to treat baclofen withdrawal, but the patient may need to be intubated to facilitate a sufficient amount of propofol. Specialty consultation is required to address most complications of intrathecal pumps. Procedure for Treating Medication Overdose When there is concern for medication overdose secondary to the rare malfunction of the device, in addition to emergency medical management, the emergency physician can empty the pump reservoir by using the steps outlined in Box 70. One may also access the manufacturer-specific online manuals to review the steps necessary to remove the contents of the pump reservoir and thus prevent further infusion of intrathecal medication. In 1985, Zabara demonstrated the anticonvulsant effect of vagal nerve stimulation through animal studies. The generator turns off and then immediately on again, thereby delivering a burst of vagal nerve stimulation based on the preprogrammed settings. If the device is properly turned off, the patient should notice loss of episodic adverse effects, such as stimulation-induced voice alteration or pain. Cerebrospinal fluid may be withdrawn directly from a side port on the pump if a lumbar puncture is required. Device Complications the device is typically turned on 10 to 14 days after implantation to allow adequate wound healing. Be aware that patients seen postoperatively during the first 2 weeks after implantation may not have had their device activated yet. In addition to surgery-related risks and complications, if the patient complains of severe neck pain, worsening hoarseness, choking, or difficulty breathing, consider device-specific complications. Voice alteration or hoarseness is the most common device-specific adverse effect, with more than 50% of patients being affected. Interrogation and programming of the device are conducted with an external programming wand connected to a handheld computer. The variable settings that can be adjusted include current output, signal frequency, pulse width, and on/ off stimulation times. Holding a magnet over the pulse generator for at least 65 seconds (5 seconds in the Model 106) will turn off any ongoing stimulation while the magnet is held in place. This on-demand stimulation, if initiated at the onset of an aura or seizure, may abort the attack or, if initiated during a seizure, may halt its progression. Phrenic nerve stimulator or diaphragmatic pacemaker Electrodes implanted into each phrenic nerve with a receiver implanted into subcutaneous tissue. Used to treat respiratory insufficiency secondary to upper motor neuron paralysis or respiratory drive dysfunction. Peterson When evaluating the pregnant patient who has been or may be exposed to ionizing radiation and attempting to estimate risk, consideration must be given to a number of factors. These include not only factors related to gestational age, dose and type of radiation, and the studies performed or to be performed, but also to the mother herself, as studies raise concern about exposure of maternal breast tissue to ionizing radiation and the future risk of breast cancer. As radiation propagates through space, it can impart or give-up some or all of its energy to surrounding material or tissues, and detection of this energy or its absence forms the basis of diagnostic medical imaging. Clinicians, nurses, and even radiologists may be ignorant of the effects of ionizing and nonionizing radiation. For example, 23% of pregnancies in Greece were terminated after the Chernobyl incident because of unsubstantiated fears. According to the American College of Obstetricians and Gynecologists, "With few exceptions, radiation exposure through radiography, computed tomography scan, or nuclear medicine imaging techniques is at a dose much lower than the exposure associated with fetal harm. If these techniques are necessary in addition to ultrasonography or magnetic resonance imaging or are more readily available for the diagnosis in question, they should not be withheld from a pregnant patient. Their probability of occurrence rises with dose, and their severity is independent of the dose. The quantity of energy that is imparted by radiation to the material or tissue is a physical quantity, can objectively be measured, and is called the absorbed dose (D). This unit is deprecated but remains in use in some countries (notably the United States). The many forms of radiation differ in their abilities to impart energy to the absorbing material and cause ionizing events. The radiation weighting factor, previously called the quality factor, is dependent only on the type of radiation (and for neutrons, its energy) and is dimensionless. Per the International Committee on Radiological Protection, wR = 1 for all photons and electrons; wR = 2 for protons and charged pions; wR = 20 for alpha particles, heavy ions, and fission fragments; and wR is a continuous function of energy for neutrons. As diagnostic radiology examinations involve essentially only photons, the equivalent and effective doses have essentially the same magnitude as the absorbed dose. As an example, a mean absorbed dose of 100 mGy results in an effective dose of 100 mSv if the source is electromagnetic radiation or 2 Sv if the source is alpha radiation. Radioactive decay or radioactivity is the process by which the nucleus of an unstable atom emits energy in the form of radiation. At the quantum level, the process is stochastic, but at the macroscopic level, the decay of a sufficiently large collection of unstable atoms can be calculated and is represented by the half-life, or the time it takes for the collection of unstable atoms to reduce by half. Its units are therefore inverse seconds (1 Bq = 1 s-1), as a nuclear decay event is dimensionless. Its definition is based on the amount of radioactivity in one gram of radium and also has units of events per second; 1 Ci = 3. These units encode neither the type nor energy of the radiation emitted by the nuclear decay process. The risks of radiation are most significant during organogenesis and the early fetal period, somewhat less in the second trimester, and least in the third trimester. It is in this stage of development that the embryo is least likely to be malformed,5 and the predominant effect of radiation exposure is failure to implant,12 resulting in abortion. Embryos that survive exposure in this period of development demonstrate no increased risk for malformations or growth retardation. Although any organ system can be affected, the predominantly observed effects are microcephaly and growth retardation,5,1214 and have a dose threshold of 50 to 200 mGy,12,13 which is significantly higher than doses obtained from diagnostic radiology examinations.
Purchase cheap finasteride on-line. Nutrine Garlic Shampoo 4 Hair loss & Nutrine Garlic Conditioner 4 Hair loss.
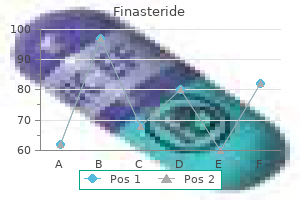
The arcuate arteries lie between the outer and the middle third of the uterine wall hair loss and itchy scalp finasteride 1 mg buy lowest price, either anterior or posterior hair loss women vitamin deficiency discount 5 mg finasteride with amex. Free anastomoses between the arcuate arteries on either side of the uterus can be seen hair loss 12 months postpartum purchase finasteride with amex. The blood supply of the tube and the ovary is derived from both the uterine and the ovarian arteries hair loss cure october 2014 best finasteride 5 mg. In general hair loss treatment 2015 generic 5 mg finasteride mastercard, the uterine supplies the medial half of the ovary and the medial two thirds of the tube, whereas the remainder of the blood supply arises from the ovarian artery. It anastomoses with the vaginal arteries, forming the azygos artery of the vagina. The cervicovaginal branch arises directly from the uterine artery in 91% of cases, whereas in 9% its origin is directly from the internal iliac artery. The origin of the uterine artery is extremely variable, but four different patterns have been identified. Type I is defined as the uterine artery arising as the first branch of the inferior gluteal artery (45%). However, in a recent publication, the classification of the uterine artery was inconclusive in 23% of the cases, and not possible to be studied in 39% of the angiograms. Uterine Artery Supplies Ureter Vagina Uterus Broad ligament of uterus Round ligament of uterus Uterine tube and part of the ovary the tortuous terminal branches in the uterus are called helicine arteries Vaginal Artery the vaginal artery may be two or three arteries and corresponds to the inferior vesical artery in males. Supplies Vagina Vesical fundus Rectum Obturator Artery this artery leaves the pelvis through the obturator canal and has an anterior and a posterior branch. Branches Inside the Pelvis Iliac branches Vesical branch Pubic branch Outside the Pelvis Anterior and posterior branches encircle the foramen Anterior branches supply various muscles and anastomoses with the medial circumflex femoral artery Posterior branches supply various muscles and anastomoses with the inferior gluteal artery; give an acetabular branch that supplies the acetabular fossa and the femoral head through the ligament of the femoral head A pubic branch of the inferior epigastric artery may replace the obturator artery. It may be a branch either of the anterior or posterior trunks of the internal iliac artery and may be a branch of the superior or inferior gluteal artery. Branches Inferior rectal artery (anastomoses with the contralateral inferior rectal artery and with the superior and middle rectal arteries) Perineal artery. Enters the crus penis and transverses the corpus cavernosum longitudinally, supplying the erectile tissue on each side; runs the entire length. Erection results from parasympathetic stimulation via the pudendal nerves, with contraction of the smooth muscles enlarging the sinusoids and the intersinusoidal connections, with simultaneous closure of the venous outflow and increase of the arterial inflow. The inferior gluteal and internal pudendal arteries are often a common stem from the internal iliac, sometimes including the superior gluteal artery. There arteries continue down the thigh with the sciatic and posterior femoral cutaneous nerves, supplying these nerves as well, and anastomoses distally with branches of the perforating arteries in the thigh. Internal iliac and inferior gluteal artery embolization may cause nerve ischemia and paralysis of segments of the lower extremity. The artery profunda femoris is also an important blood supplier to the sciatic nerve, and embolization of this artery may cause nerve damage by ischemia. Branches Inside the pelvis Muscular (piriformis, coccygeus, and elevator ani) Perirectal fat Vesical fundus, seminal vesicles, and prostate Outside the pelvis Muscular branches Anastomoses with superior gluteal, internal pudendal, obturator, and medial circumflex femoral arteries Coccygeal branches Artery of the sciatic nerve Anastomotic branch Join the cruciate anastomosis (perforating arteries) Articular branch Cutaneous branch Branches of the Posterior Trunk Iliolumbar Artery. Branches Lumbar branch (psoas and quadratus lumborum) Anastomoses with the fourth lumbar artery and sends a small spinal branch to the cauda equina between the fifth lumbar and first sacral vertebrae. The ventral rami of L5, S1, and S2 from the sacral and coccygeal plexus have supply from the iliolumbar artery. Embolization of this artery can cause paresthesia and paralysis of the lower extremity. Iliac branch (iliac bone through a nutrient branch) Anastomoses with the superior gluteal, circumflex iliac, and lateral circumflex femoral arteries Lateral Sacral Arteries. It passes the lower part of the greater sciatic foramen to reach 658 Atlas of Vascular Anatomy Inferior lateral sacral branch Anastomoses with the median sacral artery, anterior to the coccyx, and enters the sacral canal through the anterior sacral foramina Branches Inferior Epigastric Artery. It anastomoses with the superior epigastric and lower posterior intercostal arteries. Leaves the pelvis through the greater sciatic foramen above the piriformis and dividing in superficial and deep branches. Branches Cremasteric artery Pubic branch Muscular branches Cutaneous branches Branches Superficial branch Supplies the gluteus maximus; anastomoses with the inferior gluteal artery and posterior branches of the lateral sacral arteries Deep branch Divides into superior and inferior rami. The superior ramus anastomoses with the deep circumflex iliac artery and the ascending branch of the lateral circumflex femoral artery. The inferior ramus anastomoses with the lateral circumflex femoral, inferior gluteal, and ascending branch of the medial circumflex femoral artery Deep Circumflex Iliac Artery. It anastomoses with the ascending branch of the lateral circumflex femoral artery and the iliolumbar and superior gluteal arteries and has a large ascending branch. It is important to be aware of the terminology employed in discussing collateral circulation. An affluent vessel is a collateral branch that arises from a patent main vessel above the obstruction or from a patent contralateral mate. An effluent vessel is a branch below the obstruction that receives blood from the affluent vessel and allows it to flow in a retrograde manner to reconstitute the occluded artery. The affluent vessel may pass blood into the effluent vessel as a continuous line, a phenomenon called inosculation, or may be connected to the effluent vessel by a network of fine vessels, forming what is called retiform anastomosis. Inosculation keeps a good flow through the anastomosis, with a heavy head of pressure, leading to refilling of the main vessels distal to the occlusion. An example of retiform anastomosis is the communication between the lumbar and iliolumbar arteries or the Winslow pathway (that is, from the intercostal and internal mammary arteries to the external iliac arteries via the epigastric arteries). An example of inosculation is between the lateral ascending branch of the arteria profunda femoris and lateral branches of the superior gluteal artery. The sciatic artery is the axial artery of the lower extremity, providing blood supply during the early stages of embryonic development. It normally regresses to form the proximal part of the inferior gluteal artery after the third month of embryologic life, after the development of the femoral artery from the external iliac artery. If the femoral system fails to develop, the sciatic artery becomes the dominant supply to the leg and the superficial femoral artery remains hypoplastic. Conversely, failure of complete involution of the sciatic artery may result in a hypoplastic sciatic artery with a normal femoral system. Aneurysm formation in the persistent sciatic artery occurs in as many as 46% of cases, and may be the first evidence of the presence of the anomaly, causing buttock pain and sometimes sciatic nerve compression with sciatic pain in the affected leg. The sciatic vein usually follows the same path as that of the artery but is less perceptible in the imaging modalities. Larger than the internal iliac arteries, they descend laterally along the medial border of the psoas major, entering the thigh posteriorly to the inguinal ligament, thereby becoming the femoral artery. Selective arteriography of the right internal iliac artery in an elderly patient showing the gluteal arteries and branches. Pelvic angiography in a patient with occlusive disease, showing the development of the collateralization in the pelvis. A, Pelvic angiography in a patient with a uterine lesion showing the enlargement of the uterine arteries. D, Selective angiography of the right internal iliac artery shows the pelvic circulation, mainly the uterine artery. E, Selective injection at the left uterine artery shows the typical vascular pattern of the enlarged uterus. A, Type I uterine artery arising as the first branch of the inferior gluteal artery, or anterior trunk. Other branches such as the internal pudendal artery may be the first branch of the inferior gluteal artery. The uterine artery, the inferior gluteal artery, and the superior gluteal artery arise at the same level as a trifurcation. The right uterine artery is the first branch of the anterior trunk, inferior gluteal artery (Type I). The left uterine artery is the first branch of the inferior gluteal artery, but not as evident (type I). The uterine artery origin is the first branch of the inferior gluteal artery (type I). The spongiosal artery is not always visible and the interruption at the bulb of the corpus spongiosum is an angiographic artifact. Selective right internal pudendal angiogram showing the classic arterial anatomy of the penis. The penile artery is the continuation of the internal pudendal artery after it gives origin to the perineal artery, and scrotal branches. The cavernosal artery is larger than usual and freely anastomoses with segments of the dorsal penile artery. B, Late phase of the angiogram showing the corpus cavernosum and corpus spongiosum. Selective angiography of the right internal iliac artery showing only the dorsal penile artery. A, Selective angiography of the right internal iliac artery shows the right dorsal penile artery and right and left cavernosal arteries filling from the right side injection. B, Right internal iliac angiography shows the dorsal penile artery and the cavernosal artery. C, Right internal iliac artery shows a small dorsal penile artery, an even smaller cavernosal artery, and a long and relatively large spongiosal artery. When flaccid, the sinusoids are smaller in capacity and the muscle has a high tonus, limiting arterial inflow. After stimulation, the sinusoidal smooth muscle relaxes and the sinusoids distend, reducing resistance to arterial flow, and obstructing the venous outflow by compressing the peripheral venules against the tunica albuginea, thereby raising the cavernosal pressure close to systolic pressure. Right internal iliac angiography showing the transverse root communication between the right and left arterial systems. Pelvic angiography showing the communications between the right and left arterial systems through the transverse root communication (A) and between medial femoral circumflex arteries or external pudendal arteries (B) in a patient with vascular disease. Pelvic angiography showing the development of anastomosis between the lumbar arteries and the internal iliac branches, due to an occlusion at the aortic bifurcation. Pelvic angiography in a patient with arterial occlusion showing the development of the lateral sacral arteries and the gluteal arteries. Right internal iliac arteriogram showing the persistent sciatic artery instead of the inferior gluteal artery. Schematic diagram of the major potential parietal pathways of collateral circulation encountered in chronic obstructive vascular disease at the abdominal and pelvic levels. Computerized tomographic angiogram of the thorax and abdomen showing the thoracoabdominal arterial anastomoses through the superior epigastric arteries and the inferior epigastric arteries, connecting with the common femoral arteries through the retiform anastomosis between the two systems. A, Anteroposterior view of a right internal iliac arteriogram in an individual with occluded right external iliac artery, with reconstitution of the arteria profunda femoris and superficial femoral artery through collateral anastomosis from lateral branches of the superior gluteal artery and lateral ascending branch of the arteria profunda femoris. B, Lateral view of the same arteriogram showing the continuation between the two systems. A, Anteroposterior view of a left internal iliac arteriogram in an individual with occluded left external iliac artery, with reconstitution of the arteria profunda femoris and the superficial femoral artery through collateral anastomosis from lateral branches of the superior gluteal artery and lateral ascending branch of the arteria profunda femoris. B, Lateral view of the same arteriogram showing the continuation of the two systems. Continued The external iliac vein is the continuation of the femoral vein; it begins at the inguinal ligament, and joins the internal iliac vein, thereby forming the common iliac vein. Tributaries Origin outside the pelvis Superior gluteal veins Inferior gluteal veins Internal pudendal veins Obturator vein Anterior to the sacrum Lateral sacral veins Origin in visceral venous plexus Middle rectal veins Rectal venous plexus Prostatic venous plexus Vesical plexus Dorsal veins of the penis and penile venous plexus Uterine plexuses Vaginal plexuses with the medial circumflex femoral and first perforating veins. They enter low in the greater sciatic foramen, joining the internal iliac vein, and connect with the superficial gluteal veins through the gluteal perforating veins. These receive veins from the penile bulb and the scrotal (or labial) and inferior rectal veins. The deep dorsal vein of the penis ends in the prostatic plexus, but is connected through that plexus to the internal pudendal veins. Obturator Vein this vein commences in the proximal adductor region and enters the pelvis through the obturator foramen, coursing a retroperitoneal path, passing between the ureter and the internal iliac artery to join the internal iliac vein. Middle Rectal Vein this vein arises from the rectal venous plexus, receiving tributaries from the bladder, prostate, and seminal vesicle. These veins enter the pelvis through the greater sciatic foramen, above the muscle piriformis, and join the internal iliac vein as a single trunk. It has an internal rectal plexus, under the rectal and anal epithelium, and an external rectal plexus outside the muscular layer. In the anal canal, the internal plexus has longitudinal dilations, most prominent in the left lateral, right anterolateral, and right posterolateral sectors. These veins are apt to become varicose and will be known as 699 Inferior Gluteal Veins Venae comitantes of the inferior gluteal artery. These veins arise proximal and posteriorly in the thigh and anastomose 700 Atlas of Vascular Anatomy internal hemorrhoids. The internal plexus drains mostly to the superior rectal vein but connects extensively with the external rectal plexus. The external rectal plexus drains inferiorly by the inferior rectal veins, a tributary of the internal pudendal vein. The external rectal plexus drains in the middle to a middle rectal vein, a tributary of the internal iliac vein. The superior rectal vein is the beginning of the inferior mesenteric vein and drains the superior part of the external rectal plexus. The veins in the subcutaneous part of the external rectal plexus may thrombose and form the so-called external hemorrhoids. The wide anastomoses between the rectal venous plexus and the internal iliac vein, as well as with the inferior mesenteric vein, establish communication between the portal and systemic venous systems. Vesical Plexus the vesical plexus covers the lower bladder and the prostatic base in males and is connected to the prostatic venous plexus in males and to the vaginal venous plexus in females. The superficial dorsal vein of the penis drains the prepuce and skin, and is positioned longitudinally along the penis, draining to the external pudendal veins. The superficial dorsal vein of the penis receives, along its course, flow from the corpora cavernosa penis through circumflex veins.
In the trials listed in the aforementioned treatment sections hair loss cure jak order finasteride with mastercard, patients older than 60 years had a higher risk for treatment failure and experienced more treatment-related toxicity than did younger patients hair loss and itchy scalp finasteride 5 mg otc. Age is not a contraindication to aggressive treatment hair loss 2year old buy cheap finasteride 5 mg on line, but hair loss 1 year after pregnancy finasteride 5 mg purchase on line, compared with younger patients hair loss in men zip off pants purchase finasteride paypal, fewer older adult patients receive intended chemotherapy doses, which influences the poorer outcomes seen in the elderly. As such, the use of consolidative radiation therapy is more widely accepted in this population, which can limit the number of cycles of chemotherapy. Aberrant expression of Notch1 interferes with the B-lymphoid phenotype of neoplastic B cells in classical Hodgkin lymphoma. Recommendations for initial evaluation, staging, and response assessment of Hodgkin and non-Hodgkin lymphoma: the Lugano classification. Prognostic factors and treatment outcome in primary progressive Hodgkin lymphoma: a report from the German Hodgkin Lymphoma Study Group. It was updated in 2016 and incorporates more molecular and genetic features relevant to biologically targeted therapeutics. Comparing newer trial data to older "historic control" trial data is generally not valid in part for this reason. Current clinical trial design, inclusion criteria, and interpretation of findings must take these advances in classification into account so that the trial informs the treatment effects of the specific disease of interest. Recent advances have led to resolution of clinically relevant molecular-based distinctions among lymphomas. Advances that incorporate gene expression and tumor genetic mutational analysis are likely to become relevant for everyday clinical practice in the near future. Newer therapeutic agents that show activity according to the specific tumor biology require diagnostic tests so that physicians can select appropriate therapy. In addition to infectious agents, environmental and occupational exposures, especially organic compounds such as organophosphate insecticides have been linked to lymphoma risk. Recent refinements in some of these technologies have made them invaluable tools for clinical trials, and some may become relevant to routine clinical application. Expression (or its lack thereof) of cell surface antigens and immunoglobulin proteins is dependent on the type of lymphocyte and its stage of differentiation. Analysis of these proteins in tumor cells is diagnostically useful as well as for determining tumor histogenesis. Importantly, no single immunophenotypic marker is specific for any tumor, and a constellation of features is required for specific diagnosis. There is an increasing appreciation of the relationship between tumor tissue origin and clinical behavior. The latter are considered distinct diagnostic entities and are grouped together based on functional properties of their normal counterpart. A cell of origin is postulated for each neoplasm, although this may not necessarily be the cell in which the initial transforming event occurs. Thus, the designated cell of origin represents the state of differentiation of the tumor cells that are seen in the tissues. It can also be helpful to consider lymphoid neoplasms broadly in terms of the arm of the immune system from which the tumor arises: the innate or adaptive immune response. The innate immune responses are a first-line of mucocutaneous defense not requiring antigen-presenting cells to initiate the immune response. The innate immune system cells are mainly extranodal, and lymphomas arising from these cells thus tend to be extranodal. The adaptive immune response is more complex and specific for particular pathogens and capacity to develop memory. The complexity of the adaptive immune response not only gives rise to the molecular heterogeneity of many B-cell lymphomas but also helps to determine the type of lymphoma as it relates to a particular B-cell stage of development. Most B-cell neoplasms tend to reflect the stages of normal B-cell differentiation, and the lymph node architecture is highly relevant to this process: Nodal neoplasms are more likely to be seen. T lymphoblastic leukemia/ lymphoma is termed lymphoma when the disease is confined to nodal masses and does not involve the peripheral blood and marrow. The very indolent tumors have low curative potential but median survivals measured in years to decades. The aggressive tumors have varying curative potential but without treatment can have a rapidly fatal clinical course. New B-cell receptor inhibitors, such as ibrutinib and idelalisib, may have a role in the management. Allogeneic stem cell transplant may offer curative potential in selected patients. It appears to be associated with hepatitis C infection and virus eradication may be effective lymphoma management. Lymphoplasmacytic Lymphoma this tumor is the most frequent cause of Waldenström macroglobulinemia and is associated with marrow and nodal involvement with paraproteinemia (usually immunoglobulin M [IgM]) that can cause hyperviscosity syndrome, which when present should be treated immediately with plasmapheresis. Treatment with rituximab alone or combined with other agents such as cyclophosphamide, or bendamustine is very active. Other options include bortezomib-based therapy, carfilzomib, lenalidomide, and ibrutinib have important therapeutic roles. Solitary Plasmacytoma of the Bone Localized bone tumor consisting of monoclonal plasma cells. Extraosseous Plasmacytoma Localized plasma cell neoplasms that arise in tissues other than the bone. Monoclonal Immunoglobulin Deposition Diseases Nonorganized immunoglobulin fragments are deposited along renal basement membranes with subsequent organ deterioration. It comprises up to 50% of primary gastric lymphoma and is associated with Helicobacter pylori. This grading system has been criticized for lack of clinical relevance and poor interobserver reproducibility. Symptomatic disease or disease-causing psychological distress can be managed in various ways (as discussed further). These have a low rate of progression, but because of their frequent association with prior or synchronous lymphomas, they require additional evaluation to determine the risk of progression. If the assessment is not straightforward, expert hematopathological evaluation may be required. Duodenal-Type Follicular Lymphoma this is distinct from other gastrointestinal tract lymphomas. Most patients have localized disease, and survival appears to be excellent even without treatment. It is nodal with large highly proliferative follicles with blastoid follicular center cells rather than the classic centroblasts or centrocytes. It is typically low stage and found in Waldeyer ring and/ or cervical lymph nodes. Rituximab and other immunotherapeutics are commonly used; disease control is variable. When other mutations and cytogenetic abnormalities are present the course is generally more aggressive. In Situ Mantle Cell Neoplasia this entity has a low rate of progression and is important to recognize to avoid overtreatment. These differences are associated with molecular and immunophenotypic findings that help to segregate the various entities into various subgroups. Morphologic variants include centroblastic, immunoblastic, and anaplastic subtypes. Two cell of origin subtypes are now included in the classification because the improved molecular pathogenesis of these has led to more targeted and specific therapies based on the differences in tumor biology. Radiotherapy induced late-term neurotoxicity can lead to severe cognitive deficit. Presentation is generally an ulcerative red or bluish tumor on the leg, although other sites can be involved. Radiotherapy, immunotherapy, and stem cell transplant are reported as being used in these patients. Presenting features include localized disease, and signs and symptoms related to a large anterior mediastinal mass. Advanced-stage presentation is typical; so few cases have been reported and as such there is limited information on outcomes, although short median survival of less than 12 months is reported. Originally thought to involve predominantly the oral cavity, it is now appreciated to also involve other extranodal sites. The "starry sky" pattern on histopathology examination results from macrophages that have injected the apoptotic tumor cells. Short course intensive chemotherapy with rituximab is generally recommended (for adults), and cure rates are quite high for standard-risk disease. Most cases are in those aged more than 40 years, but the disease is rare (<2% of mature lymphocytic leukemia). After a period of recurrent skin lesions over a period of 15 years, a more aggressive systemic progression may occur. There are several clinical variants: Acute, lymphomatous, chronic, and smoldering. The most common is the acute form with elevated white blood count, skin rash, lymphadenopathy, and hypercalcemia. Upper aerodigestive involvement is characteristic, although it can involve other areas of the body. Nodular skin lesions, perforating intestinal lesions, or other sites are also seen. Prognosis is variable, but may be improved with upfront combination chemo-radiotherapy. Enteropathy-Associated T-Cell Lymphoma this is an intestinal lymphoma (mainly of the jejunum or ileum) composed of large lymphoid cells with an inflammatory background. It appears to be associated with celiac disease; early prevention with gluten-free diet appears to protect against lymphoma. There is a monomorphic variant occurring in regions where celiac disease is rare, and this is probably a different disease entity. Once lymphoma has developed, there is poor response to therapy and prognosis is unfavorable. Indolent T-Cell Lymphoproliferative Disorder of the Gastrointestinal Tract this is a new provisional entity with superficial monoclonal intestinal T-cell infiltrate. Hepatosplenic T-Cell Lymphoma the T cells of this extranodal and systemic lymphoma are generally derived from the T-cell receptor type. The peak incidence is in adolescents and young adults and accounts for <1% of all lymphomas. Initial response to chemotherapy is followed by relapse and median survival is generally less than 2 years. Patients often present with multiple subcutaneous nodules, particularly in the extremities and trunk. If hemophagocytic syndrome develops, prognosis is poor; otherwise, 80% survive 5 years or longer. Combination chemotherapy is used, but reports of immune suppressive therapy alone suggest activity and may help in treatment choices. Earlystage disease does not benefit from multiagent chemotherapy, and dermatologic skindirected therapy is generally most appropriate. Although prognosis is favorable, systemic lymphoma may develop, thus warranting an ongoing surveillance. Peripheral T-Cell Lymphoma, Not Otherwise Specified these account for about 30% of peripheral T-cell tumors in the Western world and are seen mainly in adults, with a male:female ratio of 2:1. Lymph node involvement is typical, but any site can be affected, including peripheral blood. The follicular variant can appear similar to nodular lymphocyte-predominant Hodgkin lymphoma while the T-zone variant can be mistaken for benign hyperplasia. The associated immune dysfunction renders aggressive chemotherapy administration infeasible in many cases. In particular, empiric antibiotic therapy to assess treatment failure as a means of establishing a malignant diagnosis should be relegated to the history books. If both tests are positive, the positive predictive value for lymphoma is 100%, and specific therapy can be commenced. Posttransplant Lymphoproliferative Disorders these occur after solid organ or hematopoietic cell transplant. Sufficient material is critical to conduct the studies needed to ensure accurate diagnosis B. Needle biopsies generally yield inadequate tissue for these studies and should be avoided for primary diagnosis C. Serum -fetoprotein or -human chorionic gonadotropin in young males with an isolated mediastinal mass where the differential diagnosis includes mediastinal germ cell tumor. Generally restaging after four cycles is indicated in aggressive lymphomas (repeat all abnormal tests). In indolent lymphomas, response to therapy may be slower; restaging can be performed less frequently. The rate of response may reflect tumor sensitivity to treatment and may have prognostic value. Biopsy of residual masses after therapy may be required to determine whether viable tumor is present. Response evaluation following novel biologic and immunologic therapeutics is an evolving science and consensus has not yet been reached. Disease-related features include tumor bulk, stage, number of extranodal disease sites, and histologic type and tumor histogenesis (or tumor biology). Patient-related factors include age and performance status, and whether there are comorbid conditions present that may affect the ability to administer therapy. Prognostic assessment and modeling strategies have been developed to predict the outcome based on clinical presentation. Clinical behavior is generally described as indolent, aggressive, or highly aggressive.
References
- Lee JY, Spratt DE, Liss AL, et al. Vessel-sparing radiation and functional anatomy-based preservation for erectile function after prostate radiotherapy. Lancet Oncol 2016;17(5):e198-e208.
- Duran M, Wanders RJA, de Jaguar JP, et al. 3-Hydroxydicarboxylic aciduria due to long-chain 3-hydroxyacyl coenzyme A dehydrogenase deficiency associated with sudden neonatal death: protective effect of medium-chain triglyceride treatment. Eur J Pediatr 1991;150:190.
- Oberman HA. Metaplastic carcinoma of the breast. A clinicopathologic study of 29 patients. Am J Surg Pathol. 1987;11(12):918-929.
- Erenoglu C, Miller A, Schirmer B: Laparoscopic Toupet versus Nissen fundoplication for the treatment of gastroesophageal reflux disease. Int Surg 88:219, 2003.
- Nukada H, Pollock M, Haas LF. The clinical spectrum and morphology of type II hereditary sensory neuropathy. Brain. 1982;105:647-665.