- info@careermakers.edu.np
- +977 1 4423870
Mebendazole
Peter Faulhaber, MD, MA
- Associate Professor of Radiology
- Case Medical Center
- Case Western Reserve University
- Director
- Clinical PET
- University Hospitals Case Medical Center
- Cleveland, Ohio
Then the cancer pain movement began capside viral anti vca-igg order mebendazole with visa, and it was learned that patients with pain due to cancer often required very large doses of opiates to get relief hiv gut infection cheap mebendazole 100 mg free shipping, inexorable dose escalation due to tolerance was not a major problem antiviral zovirax purchase mebendazole 100 mg visa, and that xylitol antiviral order mebendazole with american express, with stable disease status hiv infection rate in singapore purchase discount mebendazole on-line, doses of opiates were typically stable. Furthermore, when treatment other than opiates was implemented that alleviated the cause of the pain, such patients rapidly reduced or discontinued their use of opiates without manifesting an abstinence syndrome. With little evidence to support generalization of the experience with cancer pain to noncancer pain, it was loudly advocated by a small number of physicians that every patient should be given whatever dose of opiate was required to obtain pain relief. Poor prescribing habits eventually led to inappropriate usage, a rapid increase in emergency room visits and deaths related to prescription opiates, and little reduction in pain and disability in the overall population of patients with chronic pain (6). Public outcry about excessive opiate prescribing and efforts by state and federal officials to discourage opiate usage for medicinal purposes now have made it difficult for appropriately selected patients to obtain chronic opiate prescriptions. We have seen two revolutions of the opiate-prescribing cycle in the United States. What has been lacking is reliable evidence to support the position of either side in this dispute. Care for patients with chronic pain has fluctuated widely, but certainly not on the basis of scientific evidence. Fortunately, most opiates are inexpensive, and agencies designed to control costs (often labeled as "managed care") have not focused upon their use. Another example of socioeconomic changes in the provision of care for pain patients is the rapid expansion of pain specialists among anesthesiologists that occurred in the past 20 years both in the United States and in other countries. In the United States, federal agencies determine the charges for services by an arcane process that is not immune to lobbying. Procedures such as epidural steroids, facet blocks, and nerve blocks are reimbursed far more handsomely than consultation time with the patient. It is no accident, therefore, that proceduralists rapidly increased in number (even in the absence of outcomes-based evidence for efficacy) whereas multidisciplinary pain clinics have rapidly decreased in number, since they do not generate sufficient revenue to satisfy practitioners or hospital administrators. The number of providers is directly related to economic factors such as remuneration for services. The advent of managed care in the United States was an attempt to contain costs and in some cases to establish profitable business franchises, disguised as an effort to improve patient management. Although some large managed care organizations persist, this method has not been very successful at either improving management or containing costs. Furthermore, managed care organizations often limit access to specialists, tests, drugs, procedures, and surgery; these constraints, too, can be damaging to patients with pain. Chronic pain is often not considered a "real" disease, and sufferers are considered less than deserving of care (7). As is true for almost every aspect of medical practice, there are wide variations in rates of surgery for low back pain (1,8 11). Small area analysis of surgery for low back pain has shown wide variations in the rates of surgery in different states in the United States. These variations are clearly not due to a higher prevalence of patients with defective backs who reside in each high-rate area. Although no satisfactory explanation for all of the variance has been forthcoming, clearly, physician practice style, which is influenced by both peer group pressures and economics, plays a role. Both factors do so in a largely unexamined fashion and lead to increased patient management costs. When surgeons make a much more handsome living than medical practitioners, it should not surprise anyone that more young doctors choose to go into surgery. The rate of surgery for low back pain is directly proportional to the number of orthopedic and neurologic surgeons in a country, not to the population at risk (10). Within the neurosurgical and orthopedic specialties, it is widely recognized that the most lucrative practice involves spinal fusions using hardware. Hence, the type of care offered to patients with low back pain is largely determined by the availability of providers, which is partially determined by economic factors. In his fascinating book, Occupation and Disease, Dembe documents the socioeconomic factors that have changed the way the Western world looks at low back pain (12). What started out in the 18th and early 19th centuries as a form of rheumatism, whose pathogenesis lay completely within the sufferer, evolved over a 100-year period to be an occupational disorder secondary to trauma. The development of orthopedics as a specialty facilitated this transition and led to increasing surgery to contend with low back pain. The idea that the workplace was the cause of low back pain and that illnesses originating in the workplace should be paid for by the employer completed the change in thinking about how to manage low back pain. Despite the remarkable preclinical advances described by Baron, Basbaum, Cousins, Dickenson, Yaksh, and others in this volume, health care is, and always has been determined much more by socioeconomic factors than medical science. Contemporary pain management has not been shaped by evidence of treatment efficacy. If it were, multidisciplinary pain clinics would be flourishing, instead of waning (13). Whether these external factors alter the perception of a noxious stimulus or alter the response to that stimulus, or both, is not clear. Pain behaviors are influenced by a wide range of socioeconomic factors including culture, gender, family systems, social class, education, employment, and social support systems such as compensation, litigation, and welfare programs (15). As is true for psychological factors in general (see Chapter 35 by Melzack and Katz), the impact of each of these factors varies among individuals, and it is unlikely that any single one determines the experience of or response to pain. The best model would appear to be that, whereas socioeconomic factors do not initiate chronic pain, they do influence pain behaviors and the ensuing disability. It appears heuristically useful to separate effects on pain from those on disability ascribed to pain, even though the things one does or does not do that create disability can also be considered to be pain behaviors. Thirty years later, Elton and Stanley showed that cultural and ethnic factors strongly influence both the experience of pain and the behaviors associated with it (17). Many papers have alleged that social and cultural factors, typically the family, have strong influences upon the presence of chronic pain, usually based upon the concept of modeling by children of their parents and older relatives. However Turk and colleagues have identified significant methodological flaws in most of these papers, chiefly the lack of control populations, reliance on self-report, and potentially biased recall (2). Chronic widespread pain and fibromyalgia have been found to be associated with weaker social support, a family history positive for chronic pain, and immigrant status (11). Cross-cultural studies have often reported differences in prevalence rates of chronic pain, but it is possible that factors biasing responses to questionnaires are the cause of such apparent differences. A cross-cultural epidemiologic study by Volinn revealed that low back pain was less common in poorer developing countries than in Western Europe, but the author cautioned that study methodologies or other artifacts could account for these conclusions (19). It appeared that both early-life and adult-life factors contributed to this finding. A study on the risk factors for temporomandibular pain in Norway found that adverse socioeconomic factors were much more common in those with the condition than in those without it (21). A Finnish study revealed that chronic pain and disability were more frequent with older age, lower education, and lower occupational class (22). Another study of chronic pain in women in Sweden showed that those in a "deprived socioeconomic situation not only run a higher pain risk, but also experience their pain as more severe/disabling than their more privileged counterparts" (23). An extensive literature describes the effects of the family upon the development and persistence of chronic pain (2,24,25). Children in Norway were found to be at increased risk of chronic pain if they lived in poorly educated, low-income worker families (26). Cultural affiliation has repeatedly been shown to influence the perception of and response to acute and experimental pain. Bates and co-workers, in a series of publications, investigated the relationships between ethnic group, pain perception, and variation in responses to treatment in patients with chronic pain during multidisciplinary pain therapy (28). Cultural differences in attitudes, beliefs, and emotional states predicted pain intensity variation; medications and surgical treatments did not. In conclusion, socioeconomic status is a significant predictor of prevalence, duration, and severity of almost every type of chronic pain in every country in which studies have been undertaken. Furthermore, this is true even in countries that have a universal health care system, so it is not the deficiency of health care that makes low socioeconomic status an adverse factor in chronic pain patients. The magnitude of the effect varies, and controlled, prospective, random allocation studies are few. Socioeconomic status affects all aspects of health and well-being; there is nothing unique about its effects on pain and disability. Education Most, but by no means all, of the reported studies indicate that educational level affects the prevalence and persistence of chronic pain, but it is difficult to separate educational status from social class and type of work performed. Deyo and TsuiWu did show that lower levels of education were associated independently of other factors with increased chronic low back pain and duration of disability (29). Chapter 29: Socioeconomic Factors in Chronic Pain and Its Management 647 Socioeconomic Class Lower social class is probably a factor in chronic pain in general and low back pain specifically (15), an effect that, in published studies, is larger in males than females. This effect seems to be related primarily to the large number of manual laborers in the lower classes. Whether the recent increase in outside-thehome employment for women will alter this phenomenon is unknown. However, migraine headaches in women are more common in lower-income households in the United States, and women from lower-income households are more likely to use emergency rooms for their health care (30). At the time of the Institute of Medicine review of Pain and Disability in 1987, the available literature strongly suggested that socioeconomic factors were associated with low back pain, lower educational status, low occupational status, and heavy physical demands of the job (31). Another aspect of the influence of social class on pain was revealed by Richards and colleagues, who studied differences in responses to chest pain between those men who resided in an affluent neighborhood and those who lived in a deprived region in Glasgow (32). Residents of the deprived regions reported greater exposure to ill health, perceived themselves to be more vulnerable to heart disease, yet were less likely to seek cardiology care. The authors concluded that social and cultural factors influenced perceptions of symptoms and illness behavior. This same study showed that socioeconomic factors were not related to radiologic findings of disc degeneration. Chronic pain and the disability associated with it were found to be strongly associated with socioeconomic disadvantage, high levels of unemployment, and significant costs to the disabled worker and society in Australia (34). Most pain management physicians agree that a patient who is enmeshed in a compensation system has a potent comorbidity that often intrudes into the rehabilitative process. There is evidence from the review by Rohling (35) that the experience of pain is more intense in those receiving compensation. However, the literature on the effects of compensation upon symptom relief, treatment response, and return to work is not uniformly indicative of the ill effects of compensation. How much of the variance is methodologic and how much is related to different countries and compensation plans is not clear (31,35). In a separate study, Mendelson found that personal injury litigants did not describe their pain as more severe than nonlitigants, nor were they more psychologically disturbed (39). A very interesting literature addresses the effects of rear-end auto collisions ("whiplash injury"). First, subjects in a study by Castro and co-workers used bumper cars (as found in an amusement park) to experience collisions at 6 to 9 mph. This seems odd, as many people involved in rear-end collisions in automobile accidents at similar speeds do ascribe neck pain to their accidents. A report by Schrader suggested that whiplash symptoms were rare in a society that did not offer compensation and litigation for such an injury (41). At the North American Spine Society meeting in 1997, Patheni reported that only 9% of Greeks involved in such an accident had any symptoms, and that none persisted for 6 months (42). Finally, Borchgrevink reported on a sample of 201 whiplash patients who were randomly assigned either to a cervical collar or resumption of normal activities. The group receiving a cervical collar had significantly more symptoms that persisted longer (43). Other studies of whiplash injury report similar findings of a link between litigation and symptom severity. This sample of the literature shows that socioeconomic factors such as a tort system, expectation of litigation and compensation, and the culture in which an accident occurs, in addition to the physical forces involved, can strongly influence the incidence and persistence of pain. These conclusions are consistent with a recent Australian telephone survey of 484 adults with chronic pain by Blyth, Cousins, and colleagues, in which "litigation. Influences on Disability Ascribed to Pain Disability ascribed to pain is a major burden in any developed country. The complaint of pain must be discriminated from the disability that is blamed on the existence of pain; it is much easier to measure the disability than the pain itself. In most studies, disability really means failure to be gainfully employed for wages but, particularly in the elderly, disability does not necessarily involve work status. It is wisest to consider disability as the result of an impairment that interferes with activities of daily living, including, but not limited to work. A study by Thumboo, Chew, and Lewin-Koh in Singapore found that ethnicity, youth, education and employment status, and psychological factors influenced both pain and functioning (45). A Canadian study of whiplash injury victims indicated that longer recovery periods were associated with older age, female sex, having dependents, and not being employed full time. Neurologic findings and the dynamics of the accident also contributed to lengthening recovery time (46). A systematic review, also by Canadian investigators, indicated that workplace factors such as the lack of workplace accommodation and lack of work autonomy predicted chronic pain disability. On the other hand, factors such as lower job satisfaction, perception of difficult work demands, heavy physical demands of the job, private rather than public employment, and lower socioeconomic status were not predictive in that review (21). An interesting Litigation Litigation, such as being involved in a compensation system, may alter the disability ascribed to pain, but no evidence supports the idea that pain is caused or perpetuated by litigation. The myth of "cured by a verdict," as promulgated by the English neurologist Henry Miller, in 1961, has never been supported by any research and should be discarded (36,37). Socioeconomic factors are important in the relationships between injury, impairment, and disability (48). An extensive body of literature on wage replacement programs for injured workers and the availability of disability programs for those who do not work has led to the recognition of the moral hazard of these insurance programs: Some people take advantage of such programs to avoid productive employment. Twenty years ago, Beals summarized the effects of a compensation system on the recovery from injury and advocated that these systems be changed so as to provide incentives for, rather than impediments to , return to work (50).
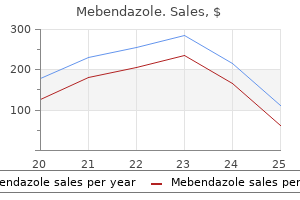
The residual analgesia allows for more rapid early recovery antiretroviral used for hiv mebendazole 100 mg on-line, with a high degree of alertness and freedom from nausea (66) antiviral medication for chickenpox mebendazole 100 mg discount. This syndrome usually presents as back pain radiating into the groin or legs antiviral yify mebendazole 100 mg generic, beginning 6 to 24 hours following the resolution of spinal anesthesia and persisting for 3 to 5 days (68) how long after hiv infection do symptoms show discount mebendazole 100 mg buy on-line. The degree of discomfort is variable how the hiv infection cycle works order mebendazole 100 mg otc, but may be sufficient to preclude return to normal daily activities or to work. The phenomenon Herniorrhaphy Hernia repair includes inguinal, femoral, umbilical, or incisional herniorrhaphies. Inguinal hernia repair is another excellent opportunity for the use of several regional techniques. Lidocaine spinal anesthesia provides good muscle relaxation and exposure, but with a discharge time slightly longer than general anesthesia (54). The use of longer-acting drugs, such as bupivacaine, is associated with greater variability of block and duration (55), longer discharge, and a higher frequency of urinary retention (56), and may not be competitive in the outpatient setting with local infiltration or general anesthesia (57,58). The evident dilemma is that the use of the higher doses of drug needed for the higher level of anesthesia may also be associated with delayed voiding (17). Thus, the choice of spinal anesthetic for outpatient hernia repair is a challenging one. Epidural anesthesia may offer an acceptable alternative, in which short-acting drugs may be used with a continuous technique, but the longer performance and onset time of epidural blocks limits their use. Paravertebral blockade has been utilized because it is not associated with urinary retention and does not require resolution before discharge. Despite the longer time, the potential for failed block, and the potential for epidural spread (60), this technique may have a role in outpatient hernia repair. Many studies of hernia repair illustrate the advantages of local infiltration for postoperative analgesia in what is otherwise an uncomfortable operation (61). Preincisional blockade of the ilioinguinal and iliohypogastric nerve provides significant pain reduction in the immediate postoperative period (62) and can allow for performance of this procedure under local anesthesia with sedation. The incidence of the syndrome is generally around 15% with lidocaine, but increases to as high as 30% when knee arthroscopy and lithotomy-position operations are performed using this drug. Many anesthesiologists have abandoned the use of lidocaine for arthroscopy for this reason. Ben-David and his colleagues found that a 5-mg dose of plain bupivacaine was inadequate (69), but the addition of fentanyl provided adequate anesthesia for their patients (70). Although the discharge times were acceptable (3 hours from time of injection), the variability of bupivacaine is wide and may result in delayed discharge in some patients. Ben-David and his group have also looked at verylow-dose lidocaine as an alternative to the standard 50-mg lidocaine spinal anesthetic. There remain questions about the history of neurotoxicity with chloroprocaine that also need to be resolved before it can be recommended as a subarachnoid agent (76,77). Nevertheless, spinal anesthesia remains the most reliable and time-effective alternative for regional techniques for outpatient knee arthroscopy, and preservative-free 2-chloroprocaine may be identified as the ideal drug. Unilateral spinal blockade has been advocated as a technique to reduce the total dosage and duration of spinal anesthesia for arthroscopy. This is usually achieved by placing the patient in a lateral position and injecting a small dose of hyperbaric local anesthetic. If the lateral position is maintained for 10 to 15 minutes, the majority of anesthesia is produced in the dependent extremity (7881). Some spillover inevitably T6 Lidocaine T8 2-Chloroprocaine T10 Dermatome T12 L2 L4 S1 S3 0 10 20 30 40 50 60 70 80 90 100 110 120 130 140 150 160 170 Time (min) p = 0. Extent and duration of subarachnoid anesthesia with 40 mg lidocaine or 2-chloroprocaine in volunteers. This technique is useful in trying to provide targeted anesthesia of only the involved extremity, but it cannot be relied upon to exclusively anesthetize one side. A second alternative is the use of lumbar epidural anesthesia, which provides an appropriate band of analgesia and anesthesia at the dermatomes needed for the surgical procedure. Again, 2-chloroprocaine is an ideal choice for this procedure because of its rapid onset and predictable 1-hour duration. The resolution of a 2chloroprocaine epidural is equivalent to spinal anesthesia with chloroprocaine and is somewhat faster than spinal anesthesia with procaine, lidocaine, or bupivacaine. The disadvantage of epidural injection is the slower onset compared to spinal block, but this can be overcome by the use of an induction area, or by the use of the combined spinal-epidural technique (83). Urmey and colleagues have used this procedure to provide rapid onset, but with the added benefit of the potential for prolonged duration if the procedure becomes prolonged. With both of these neuraxial techniques, patients can generally tolerate the procedure with minimal sedation and thus observe the arthroscopy on the monitor screen and see the anatomy of their own surgical procedure. One issue is the potential for urinary retention, but, as discussed, this is infrequent with short-acting blocks. In these situations, local infiltration of the wound portals is helpful in reducing postoperative pain. There is also some evidence that installation of bupivacaine and morphine into the knee joint may produce analgesia for several hours or as long as 24 hours following knee arthroscopy. Psoas compartment block has been described as an effective single-shot injection for knee surgery (84). The single injection in the back at the lower lumbar level provides blockade of the femoral, lateral femoral cutaneous, and usually the obturator nerves, thus allowing analgesia of the entire anterior medial and lateral portions of the knee joint where the trocar insertion sites are placed. The disadvantage of the psoas block is the somewhat slower onset than spinal anesthesia, but it can certainly be competitive with epidural anesthesia in terms of its onset. As with other nerve block techniques, patients need to be cautioned about the potential for residual blockade of the femoral nerve and the associated quadriceps weakness. If crutches are used to provide discharge ambulation, a prolonged blockade (such as with mepivacaine or even bupivacaine) can provide prolonged analgesia for patients while still providing ambulation. This is simpler to perform than a psoas compartment block and can be instituted rapidly. Injection of the femoral nerve sheath generally provides reliable blockade of the lateral femoral cutaneous nerve, thus creating sensory analgesia of the anterior portions of the leg where the trocar insertions are usually performed. Pain scores after anterior cruciate ligament repair with placebo, single-shot femoral nerve block, or continuous infusion with levobupivacaine. In experienced hands, the time to surgical readiness is equivalent to spinal anesthesia (87). This technique provides faster recovery than general anesthesia, and can provide faster discharge if a short-acting local anesthetic such as 2-chloroprociane is used for the blocks (88). With all of the regional techniques possible for the knee, postoperative analgesia and ambulation must be considered. With the unilateral peripheral nerve blocks, prolonged analgesia for the more painful procedures of the lower leg, such as anterior cruciate ligament repair with a patellar tendon autograft, can be provided by a longer-acting local anesthetic. This technique reduces postoperative pain sufficiently to significantly reduce the chance of overnight admission, potentially by a factor of 10 (90), and to reduce hospital costs dramatically (91). For more complex surgeries, the use of a combined femoral and sciatic block provides additional analgesia (92,93) and also reduces the chance of overnight admission. Discharge with a numb thigh limits ambulation, but can be overcome by the use of crutches and careful patient instruction. Pain relief can be extended even further by the insertion of a continuous femoral nerve catheter (9496). Surgery to the Foot and Ankle Most surgical procedures to the foot and ankle are also performed on an outpatient basis. They vary in intensity and duration from simple bunionectomies to much more complex repairs of the ligaments and bones of the anterior and posterior foot. Many of the less painful procedures can be performed with a simple local anesthetic injection by the surgeon. The more complex operations are amenable to an ankle or popliteal fossa block, particularly if a tourniquet is not to be used (or if a low calf tourniquet can be employed). For a full ankle block, five separate injections of five nerves are required, and the onset time is somewhat slow. This technique would be ideally performed in a holding area or before the positioning, preparation, and draping in the operating room, to allow adequate time for onset. Anesthesia with bupivacaine will provide up to 12 hours of postoperative pain relief and is useful in allowing patients to go home pain free. If longer analgesia is required, or for the more extensive and painful operations, more proximal blockade of the nerves can be used. This can most easily be accomplished by a popliteal fossa blockade of the two branches of the sciatic nerve, which must be supplemented by a block of the saphenous branch of the femoral nerve at the level of the tibial head. Popliteal fossa block can be performed either in the traditional posterior approach or in the supine position via a lateral approach between the heads of the biceps femoris and the vastus lateralis. This block is useful for operations performed with the use of a calf tourniquet and when longer analgesia is required, and can be sufficient as the sole anesthetic for the surgery (97). Again, as with the ankle block, the onset is relatively slow, and the block should be placed in a separate area as early as possible before the intended incision. This approach is also amenable to the use of continuous catheters, which can provide superb pain relief for several days after surgery (97,98). White has shown better immediate pain control after extensive foot surgery, facilitating earlier discharge home and lower overnight admission rates (99). Ilfeld and Borgeat have confirmed better analgesia, lower opioid consumption, and better sleep patterns at home with 72 hour continuous popliteal infusions (100,101), Capdevilla further evaluated whether this improved analgesia could enhance recovery. For much longer and more complex operations in which a thigh tourniquet is to be used by the surgeon, more central blockade is appropriate, usually through a subarachnoid injection. Although combined blockade of the sciatic and lumbar plexus at the level of the hip could provide adequate analgesia, it would also interfere significantly with ambulation and discharge. The use of a spinal anesthetic combined with more distal block (either popliteal fossa or ankle block) is ideal in this situation for providing adequate surgical anesthesia and excellent residual analgesia to facilitate discharge home. If a spinal anesthetic is used, a unilateral technique can be employed, as described earlier. Pediatric Regional Techniques Regional techniques can also be applied to pediatric patients in the outpatient setting to provide the advantages of postoperative analgesia and rapid discharge, as in the adult (see also Chapter 27). The primary applications in this age group for outpatient surgery are aimed at providing pain relief in the healthy child being discharged home the same day. An alternative for a child is simply to irrigate the wound with local anesthetic; this appears to have efficacy equal to injection techniques for hernia surgery (103). Ilioinguinal nerve block is simple and useful after hernia repair or scrotal procedures. A 25-gauge needle is introduced into the abdominal wall 1 cm above and medial to the anterior superior iliac spine and a volume of local anesthetic is injected in a fan-wise direction to block the ilioinguinal nerve fibers traveling between the transverse and internal oblique abdominal muscles and the iliohypogastric fibers running superficially to the muscles. The sacral hiatus is much more easily appreciated in children than in adults, and the cornua on either side can be seen and easily palpated. This block is usually performed with the infant asleep, and it requires very little time in experienced hands (see Chapters 11 and 27). The simplest is the subcuta- neous ring block, injecting local anesthetic superficial to the fascia of the penile shaft at its base. Alternatively, 1 to 2 mL of local anesthetic can be injected deep to the fascia (Buck fascia) on either side of the dorsal midline. This will provide analgesia for procedures on the distal shaft, although the proximal shaft and the base of the penis are innervated by the genitofemoral and ilioinguinal nerves, which must be blocked by superficial infiltration. The principles of anesthetic management for outpatients are the same as those for inpatients, but the added advantages of prolonged analgesia and reduced side effects make neural blockade an excellent anesthetic choice. If these considerations are followed, the use of neural blockade in outpatients will be a most satisfying experience. Postoperative pain experience: Results from a national survey suggest postoperative pain continues to be undermanaged. Postoperative nausea and vomiting after discharge from outpatient surgery centers. Practice guidelines for the perioperative management of patients with obstructive sleep apnea: A report by the American Society of Anesthesiologists Task Force on perioperative management of patients with obstructive sleep apnea. Influence of obesity on surgical regional anesthesia in the ambulatory setting: An analysis of 9,038 blocks. Brachial plexus anesthesia compared to general anesthesia when a block room is available. A retrospective comparison of interscalene block and general anesthesia for ambulatory surgery shoulder arthroscopy. The learning curve associated with a simulated ultrasound-guided interventional task by inexperienced anesthesia residents. Ambulatory discharge after long-acting peripheral nerve blockade: 2382 blocks with ropivacaine. Ambulatory surgery patients may be discharged before voiding after short-acting spinal and epidural anesthesia. The preemptive analgesic effect of rofecoxib after ambulatory arthroscopic knee surgery. The preemptive analgesic effect of intraarticular bupivacaine and morphine after ambulatory arthroscopic knee surgery. Portable infusion pumps used for continuous regional analgesia: Delivery rate accuracy and consistency. Outpatient management of continuous peripheral nerve catheters placed using ultrasound guidance: An experience in 620 patients. Pharmacoeconomics of intravenous regional anaesthesia vs general anaesthesia for outpatient hand surgery. Brachial plexus anesthesia for outpatient surgical procedures on an upper extremity. A comparison of infraclavicular nerve block versus general anesthesia for hand and wrist day-case surgeries. Continuous infraclavicular brachial plexus block for postoperative pain control at home: A randomized, doubleblinded, placebo-controlled study. Suprascapular nerve block prolongs analgesia after nonarthroscopic shoulder surgery but does not improve outcome.
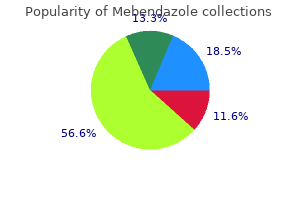
A large volume of injectate and use of a "blind" technique was likely the cause of the complications hiv infection period cheap mebendazole 100 mg on-line. Small-volume phenol injection under fluoroscopic guidance has been reported to be successful hiv infection through food 100 mg mebendazole buy amex, with only minor side effects (153) hiv infection nhs generic mebendazole 100 mg. Others have found that approximately Pelvis and Perineum the most caudal domain of the sympathetic chain includes the superior hypogastric plexus and the impar (Walter) ganglion hiv infection transmission generic 100 mg mebendazole visa. The superior hypogastric plexus is the extension of the aortic plexus below the level of aortic bifurcation antiviral brandon cronenberg order mebendazole 100 mg line. It is situated at the anterior aspect of the promontorium, with somewhat of a left side shift. The impar ganglion is the most caudal part of the sympathetic chain, located just ventrally to the sacrococcygeal junction. Moreover, phenol injection in the vicinity of the spinal cord and vertebral artery may result in direct neural damage, vascular injury, and neural infarcts (147). A: Anteroposterior view: an 18-gauge curved active tip radiofrequency cannula is inserted beneath the head of T2 rib. B: Lateral view: an 18-gauge curved active tip radiofrequency cannula is positioned in the middle of the T2 vertebra. To ensure ablation of the T2 ganglion, sequential lesions have to be made with the cannula withdrawal dorsally. A modified technique using a curved-tip cannula probably simplifies cannula positioning and lessens the risk of pneumothorax. An 18-gauge electrode with a 10-mm curved active tip is inserted between the third and fourth ribs medial to the scapular margin and aimed at a point 2 to 5 mm lateral and rostral to the midpoint of the T3 vertebra. The electrode tip is positioned at the ventral edge of T3 in the lateral x-ray image under the head of the third rib. The next lesion is made by passing the electrode between the second and third ribs just lateral to the T2T3 interspace. When each electrode is properly positioned, stimulation is carried out and positioning effected so as to avoid a somatic motor or sensory response below 0. A test lesion at 60 C for 60 seconds is made to guard against Horner syndrome, while plethysmography and hand temperature monitoring indicate whether sympathetic interruption is occurring. When all criteria have been satisfied, a 90 C 180-second lesion is made and enlarged by withdrawing the tip 8 to 10 mm. Two patients suffered from pneumothorax, three from brachial neuralgia, and one from unwanted Horner syndrome. In a recent series of 1,742 cases of hyperhidrosis, the authors concluded that the modified technique was associated with very good long-term results and a low complication rate. Similar outcomes were obtained when the sympathectomy was performed at the T2 and T3 levels, or at the T2 level only (159). Splanchnic Neurolysis Splanchnic and celiac plexus neurolysis pertains almost completely to the pain management of abdominal malignancies (see Chapter 45). Nevertheless, several observational studies suggest that the procedure can be effective in the treatment of chronic pancreatic pain (160,161). To achieve this position, a 10- to 20-degree fluoroscopic view of the T11 or T12 vertebra is obtained. The image intensifier is rotated to the lateral view, and the cannula is advanced with the tip rotated medially until reaching the anterior third of the vertebral body (see Chapter 45). Once the cannula is in place, sensory stimulation at 50 Hz is conducted up to 1 V. A: Anteroposterior view: an 18-gauge radiofrequency cannula with curved active tip rotated medially is positioned adjacent to the T12 vertebra. B: Lateral view: an 18-gauge curved active tip radiofrequency cannula is seen at the lateral surface of the T12 vertebral body reaching the anterior third of the vertebral shadow. B Chapter 42: Percutaneous Neural Destructive Techniques 1023 spaces, the cannula must be advanced anteriorly. The cannula is rotated 180 degrees, and the second lesion is performed at the same setting. If the procedure is for bilateral neurolysis, then the same procedure of testing and lesioning should be completed on the opposite site. Dondelinger and Kurdziel (163) suppressed pain in 60% of patients, but vascular improvement occurred in only 33%. Cross and Cotton (164) recorded a 67% reduction in rest pain persisting for 6 months. Gybels and Sweet note the confusion as to whether the procedure achieved its results in patients with peripheral vascular disease by virtue of vasodilation or of pain fiber interruption. Cousins and colleagues (165) reported that 80% of 386 patients with rest pain had complete or partial pain relief, with a mean duration of 6 months, regardless of changes in blood flow (see Chapter 39). The procedure was temporarily complicated by an excessively hot, swollen foot, and by postsympathectomy (genitofemoral) neuralgia in a few cases (167). Open versus Percutaneous Cordotomy Although there are still advocates of open cordotomy, a careful review of the situation reveals few indications for the open procedure. Pathologic and anatomic abnormalities virtually never interfere with the percutaneous approach, so the lesser impact and increased precision of this approach should give it priority, except when a surgeon capable of performing the procedure is not readily available to a sick patient who cannot travel. Percutaneous cordotomy is the operative cordotomy procedure of choice in cancer pain, whenever it is not contraindicated (176,177). Thereis minimal evidence of efficacy and safety of the percutaneous cordotomy in the management of nonmalignant pain (178) (see also Chapter 31). Percutaneous Cordotomy Percutaneous cordotomy, modeled after the open operation of Spiller and Martin (179), was first employed by Mullan and colleagues (180) using the lateral approach between C1 and C2, and using a radiostrontium source to make the lesion. Meanwhile, Hitchcock (187,188) and others (189) developed a dorsal approach in the occiputC1 space requiring the use of a stereotactic frame, whereas Lin and colleagues (190) introduced a low anterior cervical approach to avoid potential damage to the pathways responsible for respiratory control. Apart from an application for the treatment of cancer pain (168) (see Chapter 45), neurolytic superior hypogastric block has been proposed in the management of chronic pelvic pain associated with endometriosis and pelvic inflammatory disease (169,170). Radiofrequency lesioning of the impar ganglion has been described in the treatment of chronic perineal nonmalignant pain in a small study, demonstrating that it can decrease pain severity by at least 35% (171). The low anterior approach (190) has two disadvantages: it achieves a low level of analgesia, and it requires first traversing the cervical disk and part of the cord with the electrode before the spinothalamic tract is reached. Thus, small changes of electrode position require withdrawal of the electrode through the disk first and then reinsertion. Oil-based contrast medium, which is superior to the evanescent water-soluble types, although associated with aseptic arachnoiditis (201), is now difficult to obtain. These dimensions ensure the optimum 2-mm penetration of the cord for lesioning the spinothalamic tract and provide standard impedance measurements. If the electrode is correctly positioned, 2-Hz stimulation should produce muscle contractions in the ipsilateral neck and sometimes in the upper limb, whereas 50-Hz stimulation should produce contralateral warm/cold or "wind" sensations. If these contractions are felt in the lower limb, the electrode tip lies in the distal dermatomes of the spinothalamic tract; if felt in the hand, it lies in the proximal dermatomes. When all parameters are satisfactory, the first low-temperature (50 C) lesion is performed for 60 seconds. If cordotomy is to be performed on the second side, an interval of at least a week should be taken. Extreme caution must be observed to avoid respiratory complications; persisting unconscious respiration on the first side should be radiologically confirmed preoperatively, and the patient should be observed in an intensive care unit postoperatively, with monitoring of blood gases to detect a rising arterial carbon dioxide level forewarning of respiratory arrest. A significant risk of bladder dysfunction must be anticipated after bilateral cordotomy. The lancinating element of central spinal cord pain, that is common with thoracolumbar injuries, and allodynia or hyperpathia associated with neuropathic pain in the lower extremities are also indications (191,192) (Table 42-10). In general, severe pain in a single lower extremity is the best indication; bilateral lower limb pain requiring bilateral cordotomy exposes the patient to the risk of bladder dysfunction and respiratory complications. Bilateral lower truncal-pelvicperineal pain is a poor indication (193), partly because it responds poorly, possibly due to elements of neuropathic pain caused by previous surgery and/or radiation-and partly because it requires bilateral operation. Voluntary respiration, in response to the command "take a deep breath," is controlled by the corticospinal tract, rarely damaged during percutaneous cordotomy. On the other hand, unconscious respiration, as in sleep, is mediated by the strictly ipsilaterally distributed reticulospinal tracts. Since these lie adjacent to the cervical dermatomes of the spinothalamic tract, they are easily damaged by a cordotomy lesion that achieves high levels of cervical analgesia. This is of no concern if both lungs and their innervation are functioning normally. However, if, for example, an apical carcinoma has destroyed the phrenic nerve on one side and a cordotomy is being contemplated on the other to produce analgesia into the upper cervical dermatomes, the remaining reticulospinal tract will be interrupted and unconscious respiration abolished, with fatal results. In such situations, cordotomy is either contraindicated or fraught with much risk. The same issues apply if a previous cordotomy has interrupted the tract and a new cordotomy is now being considered on the second side. Lema and Hitchcock (200) found that respiratory function (measured as the forced expiratory volume in 1 second) was interfered with to a greater degree by high dorsal percutaneous cordotomy than by percutaneous myelotomy or trigeminal tractotomy. Other contraindications, such as anomalies or disease in the C1C2 area, virtually never interfere, and in children or confused patients who cannot cooperate, general anesthesia may be used. The dorsal (13,183,189) Results the results of percutaneous cordotomy are perhaps best displayed in tabular form. The electrode tip is impaling the cord at the level of the dentate ligament, where a lesion produced analgesia up to T6 without complications. Other Spinal Cord Procedures Hitchcock (208) has evolved a high cervical dorsal percutaneous technique in the occipitalC1 space for central myelotomy, a substitute for longitudinal myelotomy done by open laminectomy. This latter curious procedure, introduced by Armour (209), was originally intended to interrupt decussating spinothalamic fibers in the anterior commissure and thus to raise the analgesic level achieved by a cordotomy at the same level. The open operation also achieved the same effect as cordotomy if performed over many levels; when performed in the cervical area, it avoided the risk of respiratory complications. In a series of 244 cases (173), the procedure was completed in 99% of patients, achieving spinothalamic interruption in 92. Incidence of pain relief after bilateral cordotomy obeys the P-squared rule and is therefore lower than for unilateral cordotomy (82. Recurrence of the nociceptive pain for which the procedure was performed virtually never occurs in an area of persisting analgesia. Nevertheless, persistent or recurrent pain after cordotomy can result from various causes: (a) technical failure of the procedure; (b) spread of cancer beyond the site involved at the time of the cordotomy (6% of 244 cases developed pain above their cordotomy level); (c) presence or development of neuropathic pain from plexus destruction (203); and (d) development of, or intensification of, ipsilateral or "mirror" pain (41% of 244 cases) (173). Once thought to be the result of unmasking of lesser pain on the other side of the body, it now seems more likely to be the result of opening up of previously inactive ipsilateral spinothalamic cord synapses after successful cordotomy, allowing painful stimuli applied to the now analgesic site to be appreciated in the mirror position on the other side of the body (204207). In those patients in whom cordotomy was performed for other than malignant disease (191), levels of analgesia tended to fade with time and pain recurred. It is unfortunate that percutaneous cordotomy has been so nearly supplanted in many centers by subcutaneous infusion of opioids using an external pump or by intrathecal/epidural administration of opioids and local anesthetics (see Chapter 40). Because of tolerance, the former therapy may result in enormous daily dosages of morphine, with their inevitable secondary effects; and the latter, neuroaxial delivery, requires continual attendance at a medical facility. In selected patients, particularly those with lower limb pain, cordotomy-a once-only procedure-may achieve sufficient lasting pain relief so that the patient may require only small doses of oral analgesics postoperatively until the terminal stages of the illness. Diagram illustrating technique of percutaneous cordotomy by the lateral high cervical approach, including impedance changes on cord impilation and anatomic organization of the region. Possibly it is similar to that in the so-called dorsal root entry zone introduced by Hyndman (219) and elaborated by Sindou and co-workers (130) in the treatment of cancer pain, by Nashold and Ostdahl (220) for deafferentation pain at the cord level, and by Bernard and colleagues (221) for deafferentation pain affecting the trigeminal nerve. Crue and colleagues (213,222) first performed trigeminal medullary tractotomy primarily for the treatment of nociceptive pain; Fox (214,215) introduced radiographic localization. Four centimeters lateral to the midline, a second 18-gauge thin-wall lumbar puncture needle is passed over C1 lamina and aimed toward cisterna magna, terminating 12 mm from the midline as measured uncorrected on the posteroanterior film and 8 mm caudal to obex at the level of the dorsum of the brainstem on the lateral film (also uncorrected). These x-rays are achieved with a 30-inch tube-to-target and a 40-inch tube-to-film distance so as to afford reproducible measurements. Hitchcock and Schvarcz (218) performed the procedure with the patient in the sitting position under local anesthesia using a stereotactic frame. A needle is passed through the occipitalC1 interspace in the midsagittal plane, and a contrast dye is injected to outline the anterior/posterior aspects of the cord and the cisterna magna. The caudal dermatomes of the spinal tract of the fifth nerve at this location are said to lie 3 to 4 mm anterior to the posterior aspect of the cord and 6 mm lateral. Rostral dermatomes lie more laterally and anteriorly, and intermedius, ninth, and tenth dermatomes more posteriorly and medially. Stimulation of the dorsal columns or their nuclei may induce ipsilateral sensory effects; stimulation of the spinothalamic tract, contralateral sensory effects; the trigeminal effects are ipsilateral. At the level of C1, all of the trigeminal fibers, including those for the circumoral dermatomes, are present, the latter not being represented more distally. Fox (214) operated on eight patients with cancer, two with postherpetic neuralgia, one with tic, and one with questionable iatrogenic deafferentation facial pain. Analgesia of the nature is unclear and which is distinct from the spinothalamic tract (210). The procedure is an option in patients with pain caused by cancer, whereas its role in those with deafferentation pain needs further observation. It is a useful alternative to intrathecal or epidural opiate instillation in patients with midline or bilateral trunk pain in the lower body. High cervical commissurotomy is performed percutaneously under local anesthesia through the occipitalC1 interspace with the patient sitting, using a suitable frame. A cisternal myelogram outlines the dorsal and ventral aspects of the medulla and cord. It is passed toward a point 5 mm anterior to the dorsal cord margin in the midsagittal plane. As the electrode enters the cord, stimulation of dorsal columns produces paresthesias in both feet. More deeply near the central canal, stimulation effects are referred to more dorsal aspects of the lower limbs. At the central canal region, paresthesiae occur in the soles, spreading to the dorsal aspects of the legs as the current is increased. Sometimes paresthesiae affect the whole face, crossed limbs, or bilateral upper limbs, or else burning in the trunk occurs. Lesions are made as in cordotomy, just anterior to or at the sites of distal lower limb responses.
Order mebendazole online pills. 10 Signs You May Have HIV || Telugu Timepass TV.
References
- Harding AH, Darnton A, Wegerdt J, McElvenny D. Mortality among British asbestos workers undergoing regular medical examinations (1971- 2005). Occup Environ Med 2009;66(7):487-95.
- Graham Jr TP, Bricker, JT, James FW, et al. Task Force 2: Congenital heart disease: 26th Betheda Conference. J Am Coll Cardiol, 24.
- Preusser M, Capper D, Ilhan-Mutlu A, et al. Brain metastases: pathobiology and emerging targeted therapies. Acta Neuropathol 2012; 123(2):205-222.
- Czer L, Hamer A, Murthey F, et al: Transient hemodynamic dysfunction after myocardial revascularization, J Thorac Cardiovasc Surg 86:226, 1983.
