- info@careermakers.edu.np
- +977 1 4423870
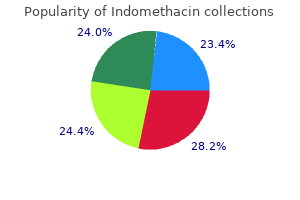
Indomethacin
John Larry, MD
- Section Chief, OSU East Cardiovascular Medicine
- Associate Professor of Medicine
- Ohio State University Medical Center
To select for cells that have undergone homologous recombination arthritis differential diagnosis order online indomethacin, a drug-based selection strategy is used arthritis treatment lower back 50 mg indomethacin buy with amex. The neo gene replaces or disrupts one of the exons of gene X on homologous recombination rheumatoid arthritis zapper 25 mg indomethacin free shipping. The thymidine kinase (tk) gene in the vector will be inserted into the genome only if random arthritis pain arm shoulder generic 50 mg indomethacin with amex, nonhomologous recombination occurs arthritis for dogs symptoms buy indomethacin with mastercard. These cells are then injected into a blastocyst, which is then implanted into the uterus of a pseudopregnant mouse. If the mutation is present in germ cells, it can be propagated by further breeding. Cells in which the gene is integrated randomly will be resistant to neomycin but will be killed by ganciclovir, whereas cells in which homologous recombination has occurred will be resistant to both drugs because the tk gene will not be incorporated. This positive-negative selection ensures that the inserted gene in surviving cells has undergone homologous recombination with endogenous sequences. In addition, targeting vectors can be designed such that homologous recombination will lead to the deletion of one or more exons of the endogenous gene. The germ cells are also usually chimeric, but because these cells are haploid, only some will contain the chromosome copy with the disrupted (mutated) gene. If chimeric mice are mated with normal (wild-type) animals and either sperm or eggs containing the chromosome with the mutation fuse with the wild-type partner, all cells in the offspring derived from such a zygote will be heterozygous for the mutation (so-called germline transmission). Such heterozygous mice can be mated to yield animals that will be homozygous for the mutation with a frequency that is predictable by simple mendelian segregation. Homologous recombination can also be used to replace a normal gene sequence with a modified version of the same gene (or of another gene), thereby creating a knockin mouse strain. Knockin mice can be used to assess the biologic consequences of a change in a single base, for instance, as opposed to the deletion of a gene. A knockin approach could, in principle, also be used to replace a defective gene with a normal one. In certain circumstances, a different gene may be placed at a defined site in the genome by use of a knockin strategy rather than in a random site as in conventional transgenic mice. In this case, the targeting vector contains an exogenous gene encoding a desired product as well as sequences homologous to an endogenous gene that are needed to target the site of recombination. Although the conventional gene-targeting strategy has proved to be of great usefulness in immunology research, the approach has some limitations. First, the mutation of one gene during development may be compensated for by altered expression of other gene products, and therefore the function of the targeted gene may be obscured. Second, in a conventional gene knockout mouse, the importance of a gene in only one tissue or at only one time during development cannot be easily assessed. Third, a functional selection marker gene, such as the neo gene, is permanently introduced into the animal genome, and this alteration may have unpredictable results on the phenotype of the animal. An important refinement of gene knockout technology that can overcome many of these drawbacks is a "conditional" targeting approach. A commonly used conditional strategy takes advantage of the bacteriophage-derived Cre/loxP recombination system. To generate mice with loxP-tagged genes, targeting vectors are constructed with one loxP site flanking the neo gene at one end and a second loxP site flanking the sequences homologous to the target at the other end. A second strain of mice carrying a cre transgene is then bred with the strain carrying the loxP-flanked ("floxed") target gene. In the offspring, expression of Cre recombinase will mediate deletion of the target gene. Importantly, expression of the cre gene, and therefore deletion of the targeted gene, can be restricted to certain tissues or specified times by the use of cre transgene constructs with different promoters. For example, selective deletion of a gene only in macrophages and granulocytes can be accomplished by using a cre transgenic mouse in which cre is driven by a lysozyme promoter, or the selective loss of a gene only in regulatory T cells can be accomplished using a foxp3 promoter driving a cre transgene. Alternatively, a steroid-inducible promoter can be used so that Cre expression and subsequent gene deletion occur only after mice are given a dose of dexamethasone. Many other variations on this technology have been devised to create conditional mutants. In this case, loxP sites are placed in the targeting vector to flank the neo gene and the homologous sequences, but they do not flank the replacement (knockin) gene sequences. Therefore, after cre-mediated deletion, the exogenous gene remains in the genome at the targeted site. Gene knock in technology has been applied to create "reporter" mice in which cells that would normally express a particular protein will express a fluorescent molecule at the same time as the native protein. This is accomplished by replacing the native gene with a transgene that encodes the fluorescent reporter protein and the native protein, both under the control of the native promoter and enhancer. The cells expressing the reporter genes can also be isolated alive and subjected to functional studies ex vivo, even if the native gene reported is a nuclear transcription factor whose expression would otherwise only be detectable by methods that kill the cells. Although such a break can disrupt a gene, co-transfecting a plasmid with a mutated version of the target sequence allows efficient homologous recombination and the creation of a targeted knockin mutation. This is the most rapid approach available for the generation of knockout or knockin mutations in cell lines or in the germlines of experimental animals. Often, these antibodies need to be immobilized on solid surfaces or beads or cross-linked with secondary anti-antibodies to induce optimal activation responses. Antigen-Induced Activation of Polyclonal T Cell Populations Polyclonal populations of normal T cells that are enriched for T cells specific for a particular antigen can be derived from the blood and peripheral lymphoid organs of individuals after immunization with the antigen. More recently, several techniques have been developed to study T cell proliferation, cytokine expression, and anatomic redistribution in response to antigen activation in vivo. The new experimental approaches have been particularly useful for the study of naive T cell activation and the localization of antigen-specific memory T cells after an immune response has waned. The limitation of these monoclonal populations is that they are maintained as longterm tissue culture lines and therefore may have phenotypically diverged from normal T cells in vivo. One type of monoclonal T cell population that is frequently used in experimental immunology is an antigen-specific T cell clone. Both helper and cytotoxic T lymphocyte clones have been established from mice and humans. Polyclonal activators are mostly used in vitro to activate T cells isolated from human blood or the lymphoid tissues of experimental animals. Polyclonal activators can also be used to activate T cells with unknown antigen specificities, and they can evoke a detectable response from mixed populations of naive T cells, even though the frequency of cells specific for any one antigen would be too low to elicit a detectable response. The Jurkat line, derived from a human T cell leukemia cell, is an example of a tumor line that is widely used as a model to study T cell signal transduction. T cells are first labeled with chemically reactive lipophilic fluorescent esters and then adoptively transferred into experimental animals. The dyes enter cells, form covalent bonds with cytoplasmic proteins, and then cannot leave the cells. Biotin binds with high affinity to a protein called avidin, and each avidin molecule binds four biotin molecules. This method is the only feasible approach for identification of antigen-specific T cells in humans. The same technique is being used to enumerate and isolate T cells specific for self antigens in normal individuals and in patients with autoimmune diseases. Cytokine secretion assays can be used to quantify cytokine-secreting effector T cells within lymphoid tissues. In these types of studies, antigen-induced activation and differentiation of T cells take place in vivo, and then T cells are isolated, restimulated with antigen or polyclonal activators, and tested for cytokine expression in vitro. Cytoplasmic staining of cytokines requires permeabilizing of the cells so that fluorochrome-labeled antibodies specific for a particular cytokine can gain entry into the cell, and the stained cells are analyzed by flow cytometry. As cytokines are secreted from individual T cells, they bind to the antibodies in discrete spots corresponding to the location of individual T cells. An approach to circumventing this problem is to use anti-Ig antibodies as analogues of antigens, with the assumption that anti-Ig will bind to constant (C) regions of membrane Ig molecules on all B cells and will have the same biologic effects as an antigen that binds to the hypervariable regions of membrane Ig molecules on only the antigen-specific B cells. To the extent that precise comparisons are feasible, this assumption appears generally correct, indicating that anti-Ig antibody is a valid model for antigens. Antigen-Induced Activation of B Cell Populations With a Single Antigen Specificity To examine the effects of antigen binding to B cells, investigators have attempted to isolate antigen-specific B cells from complex populations of normal lymphocytes or to produce cloned B cell lines with defined antigenic specificities. However, transgenic mice have been developed in which virtually all B cells express a transgenic Ig of known specificity, so that most of the B cells in these mice respond to the same antigen. A somewhat more sophisticated approach has been to generate antigen receptor knockin mice, in which rearranged Ig H and L chain genes have been homologously recombined into their endogenous loci. Such knockin animals have proved particularly useful in the examination of receptor editing. Antibody production is measured in two different ways: with assays for cumulative Ig secretion, which measure the amount of Ig that accumulates in the supernatant of cultured lymphocytes or in the serum of an immunized individual; and with single-cell assays, which determine the number of cells in an immune population that secrete Ig of a particular specificity or isotype. In addition, the availability of anti-Ig antibodies that detect Igs of different heavy or light chain classes allows measurement of the quantities of different isotypes in a sample. Other techniques to measure antibody levels include hemagglutination for anti-erythrocyte antibodies and complement-dependent lysis for antibodies specific for known cell types. Results from these assays are usually expressed as antibody titers, which are the dilution of the sample giving half-maximal effects or the dilution at which the endpoint of the assay is reached. Single-cell assays provide a measure of the numbers of Ig-secreting cells, but they cannot accurately quantify the amount of Ig secreted by each cell or by the total population. In this way, affinity maturation can be assessed by testing serum or B cells sampled at different times during an immune response. Assays to Measure B Cell Proliferation and Antibody Production Much of our knowledge of B cell activation is based on in vitro experiments, in which different stimuli are used to activate B cells and their proliferation and differentiation can be measured accurately. The same assays may be done with B cells recovered from mice exposed to different antigens or with homogeneous B cells expressing transgene-encoded antigen receptors. Here we will summarize some of the most common laboratory approaches commonly used for initial diagnosis of immunologic abnormalities. In many cases, abnormalities found by these approaches are followed up with highly specialized tests, including molecular genetic analyses. Assays for Humoral Immunity Serum protein electrophoresis can reveal decreased gamma globulins in immunodeficiency as well as monoclonal Ig peaks associated with malignant and premalignant clonal expansions of plasma cells. Evaluation of the levels of IgG subclasses in serum is most helpful in patients who have normal to borderline low total IgG (400 mg/dL in the adult population). Complement levels and function are quantified in several clinical contexts including recurrent infections, recurrent angioedema, and/or autoimmune disease. In the context of recurrent angioedema, a C4 level is often recommended as the initial screening test, followed by a C1 inhibitor level and function in the setting of a low C4 and/or a high level of clinical suspicion of an underlying C1 inhibitor deficiency. In the context of autoimmune disease, a low C3 and/or C4 level can be useful measures of ongoing immune complex formation. Autoantibody screening for a range of specificities may be performed depending on the clinical context, using various techniques in which a patents serum is tested for the presence of Ig that binds to purified antigens or to cells. Responses are determined by measuring serum levels of IgG specific to both T cell-dependent antigens (proteins or glycoproteins. Titers are most commonly measured approximately 6 weeks post-vaccination, and low titers may warrant further evaluation for an underlying B cell immunodeficiency. Akt activation, in T cell activation, 156, 158f Alarmins, 60 Alemtuzumab, 413t Alkaline phosphatase, 537538 Allelic exclusion, 195 Allergen(s), 437 nature of, 439 Allergic disease(s) genetic susceptibility to , 450452, 451t in humans, pathogenesis and therapy of, 452455 immunotherapy for, 455 Th2 cells and innate lymphoid cells in, 440 Allergic reactions basophils in IgE binding to , 442443 mediators produced by, 442t morphology of, 441f properties of, 440448, 441t eosinophils in, 448 mediators produced by, 442t morphology of, 441f properties of, 441t, 448 IgE-dependent, 448450. Erythroblastosis fetalis, 393 Escherichia coli, 353t354t E-selectin, in leukocyte recruitment, 4142, 41t Exhaustion, 365 Exotoxins, 354 Extracellular bacteria, immunity to , 353t354t, 354357. Immuno-affinity chromatography, 533, 534f Immunoassays, quantitation of antigen by, 531533, 532f Immunodeficiency(ies) acquired, 474475, 474t affecting T or B lymphocytes, features of, 460t after hematopoietic stem cell transplantation, 395 common variable, 465t congenital, 460474 multisystem disorders with, 473474 Immunodeficiency diseases acquired, 475486. This concise, well-illustrated text provides an overview of the principles of human pathology while emphasizing pathogenesis and the clinical features of disease. The key concepts and principles of pathology are presented in a condensed, at-a-glance format, making it the perfect pocket-sized reference for quick review anytime! Sinusitis can be caused by an upper respiratory infection, dental infection, atmospheric pressure changes. As the swelling and mucous production intensifies, the passageways leading to the nasal cavity become partially or completely obstructed, resulting in sinus secretion accumulation. The mucous accumulation within the paranasal sinuses further promotes the development of bacterial infections. The mucous accumulation causes pressure, pain, headaches, fever, and local tenderness. Treatment consists of antibiotics to treat bacterial infections and various therapeutic modalities designed to enhance sinus drainage, such as decongestants, hydration, and steam inhalation. Anterior-posterior X-ray film showing infection and inflammation at frontal sinus, ethmoid sinus, maxillary sinus. The precise cause is not known but may be related to chronic inflammation of the lining of nose and sinuses. Symptoms include nasal congestion, sinusitis, trouble breathing through the nose, runny nose, postnasal drip, nasal speech, mouth breathing, and loss of smell and decreased taste sensation. The tongue is located on the floor of the oral cavity and fills most of the oral cavity when the mouth is closed. When chewing food, the tongue holds the food and continuously repositions it between the teeth. In addition, the tongue mixes the food with saliva and forms a compact mass called a bolus, and then initiates swallowing by moving the bolus posteriorly into the pharynx. The intrinsic muscles are only located in the tongue and are not attached to bone. The intrinsic muscle fibers allow the tongue to change its shape-for example, to become thinner, thicker, longer, or shorter. The extrinsic muscles of the tongue extend from their points of origin on bones of the skull or of the soft palate.
Antigens may be sequestered from the immune system by anatomic barriers arthritis and rheumatology order indomethacin 25 mg free shipping, such as in the testes and eyes arthritis diet advice generic indomethacin 75 mg on-line, and thus cannot engage antigen receptors (see Chapter 14) arthritis diet book 50 mg indomethacin with mastercard. In experimental models arthritis foot mri buy discount indomethacin 50 mg on line, some self antigens are available for recognition by lymphocytes but arthritis treatment guidelines cheap 25 mg indomethacin overnight delivery, for unknown reasons, fail to elicit any response and are functionally ignored. The importance of this phenomenon of ignorance for the maintenance of self-tolerance is not established. The induction of immunologic tolerance is a possible therapeutic strategy for preventing harmful immune responses. There is great interest in inducing tolerance to treat autoimmune and allergic diseases and to prevent the rejection of organ transplants, and clinical trials are under way. Tolerance induction may also be useful for preventing immune reactions to the products of newly expressed genes in gene therapy protocols, for preventing reactions to injected proteins in patients with deficiencies of these proteins. Experimental approaches, especially the creation of genetically modified mice, have provided valuable models for analysis of self-tolerance, and many of our current concepts are based on studies with such models. Furthermore, by identifying mutations and genetic polymorphisms that may be associated with autoimmunity in mice and humans, it has been possible to deduce some of the mechanisms of self-tolerance. However, we do not know which self antigens induce central or peripheral tolerance (or are ignored). More importantly, it is also not known which tolerance mechanisms fail in common human autoimmune diseases, and this remains a major challenge in understanding autoimmunity. In the sections that follow, we will discuss central and peripheral tolerance first in T cells and then in B lymphocytes, but many aspects of the processes are common to both lineages. This is, in part, because immunologists have developed elegant experimental models for studying T cell tolerance that are informative. Also, many of the therapeutic strategies that are being developed to induce tolerance to transplants and autoantigens are aimed at inactivating or eliminating T cells. Death of immature T cells as a result of recognition of antigens in the thymus is known as deletion, or negative selection; it was described in Chapter 8 in the discussion of T cell maturation. Negative selection of thymocytes is responsible for the fact that the repertoire of mature T cells that leave the thymus and populate peripheral lymphoid tissues is unresponsive to many self antigens that are present in the thymus. Negative selection occurs in double-positive T cells in the thymic cortex and newly generated singlepositive T cells in the medulla. In both locations, immature thymocytes with high-affinity receptors for self antigens that encounter these antigens die by apoptosis. Recognition of self antigens by immature T cells in the thymus leads to the death of the cells (negative selection, or deletion) or to the development of regulatory T cells (Tregs) that enter peripheral tissues. Thus, the important questions that are relevant to negative selection are: which self antigens are present in the thymus and how are immature T cells that recognize these antigens deleted The antigens that are present in the thymus include many circulating and cell-associated proteins that are widely distributed in tissues. The thymus also has a special mechanism for expressing many protein antigens that are expressed in different peripheral tissues, so that immature T cells specific for these antigens can be deleted from the developing T cell repertoire. This group of diseases is characterized by antibody- and lymphocyte-mediated injury to multiple endocrine organs, including the parathyroids, adrenals, and pancreatic islets. The mechanisms of apoptosis are described later in this chapter, when we discuss deletion as a mechanism of peripheral T cell tolerance. Clearly, immature and mature lymphocytes interpret antigen receptor signals differently-the former die and the latter are activated. The regulatory cells leave the thymus and inhibit responses against self antigens in the periphery. What determines the choice between deletion and development of Tregs is not known. We will describe the characteristics and functions of Tregs later in the context of peripheral tolerance because these cells suppress immune responses in the periphery. These mechanisms may be responsible for T cell tolerance to tissue-specific self antigens, especially those that are not abundant in the thymus. We do not know if tolerance to different self antigens is maintained by one or another mechanism or if all of these mechanisms function cooperatively to prevent autoimmunity. The same mechanisms may also induce unresponsiveness to foreign antigens that are presented to the immune system under tolerogenic conditions. In this process, which is called anergy, the self-reactive cells do not die, but they become unresponsive to the antigen. It is likely that self antigens are continuously displayed to specific T cells in the absence of innate immunity and strong costimulation. Antigen-induced anergy has been demonstrated in a variety of experimental models, including studies with T cell clones exposed to antigens in vitro (which were the basis for the original definition of anergy), experiments in which antigens are administered to mice without adjuvants, and studies with transgenic mice in which particular protein antigens are expressed throughout life and are recognized by T cells in the absence of the inflammation and innate immune responses that normally accompany exposure to microbes. There is evidence that anergy is a mechanism of tolerance to some self antigens in humans as well. The signals involved in a normal immune response (A) and the three major mechanisms of peripheral T cell tolerance (B) are illustrated. Mice in which the gene encoding Cbl-b is knocked out show spontaneous T cell proliferation and manifestations of autoimmunity, suggesting that this enzyme is involved in maintaining T cell unresponsiveness to self antigens. It is not known why self antigen recognition, which occurs typically without strong costimulation, activates these ubiquitin ligases, whereas foreign antigens that are recognized with costimulation do so much less or not at all. The functions of the best-known inhibitory receptors of T cells are described in the following section. Regulation of T Cell Responses by Inhibitory Receptors In Chapter 9, we introduced the general concept that the outcome of antigen recognition by T cells is determined by a balance between engagement of activating and inhibitory receptors. Studies of these inhibitory receptors have increased our understanding of tolerance mechanisms and led to new therapeutic approaches for manipulating immune responses. Predictably, many of the treated patients develop manifestations of autoimmunity with inflammation in various organs. There is great interest in defining the roles of these receptors in selftolerance and the regulation of immune responses and the potential of targeting these molecules therapeutically. Suppression by Regulatory T Cells the concept that some lymphocytes could control the responses of other lymphocytes was proposed many years ago and was soon followed by experimental demonstrations of populations of T lymphocytes that suppressed immune responses. These initial findings led to enormous interest in suppressor T cells, which became one of the dominant topics of immunology research in the 1970s. However, this field has had a somewhat checkered history, mainly because initial attempts to define populations of suppressor cells and their mechanisms of action were largely unsuccessful. More than 20 years later, the idea had an impressive rebirth, with the application of better approaches to define, purify, and analyze populations of T lymphocytes that inhibit immune responses. FoxP3 is a member of the forkhead family of transcription factors and is critical for the development and function of most Tregs. These observations have established the importance of Tregs for maintaining selftolerance. Regulatory T cells (Tregs) are generated by self antigen recognition in the thymus (sometimes called natural regulatory cells) and (probably to a lesser extent) by antigen recognition in peripheral lymphoid organs (called inducible or adaptive regulatory cells). In peripheral tissues, Tregs suppress the activation and effector functions of other self-reactive and potentially pathogenic lymphocytes. Generation and Maintenance of Regulatory T Cells Tregs are generated mainly by self antigen recognition in the thymus and by recognition of self and foreign antigens in peripheral lymphoid organs. Predictably, thymic regulatory cells are specific for self antigens because these are the antigens mainly encountered in the thymus. Although many markers have been proposed to distinguish thymic from peripheral Tregs, it is not established if these markers are always unique to one subset or are similar in mice and humans. Particular populations or subsets of dendritic cells may be especially important for stimulating the development of Tregs in peripheral tissues. There is evidence that dendritic cells exposed to retinoic acid, the vitamin A analogue, are inducers of Tregs, especially in mucosal lymphoid tissues (see Chapter 14). T Lymphocyte Tolerance 335 Mechanisms of Action of Regulatory T Cells Tregs appear to suppress immune responses at multiple steps-at the induction of T cell activation in lymphoid organs as well as the effector phase of these responses in tissues. Although numerous mechanisms of suppression have been proposed, the following are the best supported by available data. It is not established if all regulatory cells work by all of these mechanisms or if there are subpopulations that use different mechanisms to control immune responses. These cytokines are produced by and act on many other cell types in addition to regulatory cells. It is synthesized as an inactive precursor that is proteolytically cleaved in the Golgi complex and forms a homodimer. This cytokine may play a pathologic role in diseases in which fibrosis is an important component, such as pulmonary fibrosis and systemic sclerosis. Because it is both produced by and inhibits macrophages and dendritic cells, it functions as a negative feedback regulator. Tregs are also critical for maintaining fetal tolerance and preventing the rejection of fetuses (see Chapter 14), and play a role in preventing elimination of commensal microbes. It is possible that the role of these cells in different tissues is related to their recognition of antigens expressed in those tissues. Deletion of T Cells by Apoptotic Cell Death T lymphocytes that recognize self antigens with high affinity or are repeatedly stimulated by antigens may die by apoptosis. Because of these findings, it is believed that this cytokine is especially important for controlling inflammatory reactions in mucosal tissues, particularly in the gastrointestinal tract (see Chapter 14). Numerous attempts are being made to identify defects in the development or function of Tregs in more common autoimmune and inflammatory diseases in humans such as inflammatory bowel disease, type 1 diabetes, and multiple sclerosis, as well as in allergic disorders. Defects in Tregs or resistance of effector cells to suppression by Tregs may contribute to the pathogenesis of these diseases. There is also potential for expanding Tregs in culture and injecting them back into patients to control pathologic immune responses. Clinical trials of Treg transfer are ongoing in attempts to treat transplant rejection, graft-versus-host disease, and autoimmune and other inflammatory disorders. In addition to their role in controlling autoimmunity, Tregs have been shown to serve many other roles. Subpopulations of Tregs with unique transcriptional signatures are present in many tissues and appear to perform functions that are especially beneficial for those tissues. Tregs in skin, muscle, and organs such as the lung promote tissue repair and the proliferation and differentiation of stem cells, thus helping to restore tissue integrity after inflammatory reactions resolve. Activated Bim binds to two pro-apoptotic effector proteins of the Bcl-2 family called Bax and Bak, which oligomerize and insert into the outer mitochondrial membrane, leading to increased mitochondrial permeability. The result is that many mitochondrial components, including cytochrome c, leak out into the cytosol and activate cytosolic enzymes called caspases. The receptors oligomerize and activate cytoplasmic adaptor proteins, which assemble procaspase-8, which cleaves itself when oligomerized to yield active caspase-8. Apoptosis is induced by the mitochondrial and death receptor pathways, described in the text, which culminate in fragmentation of the dead cell and phagocytosis of apoptotic bodies. Cells undergoing apoptosis develop membrane blebs, and fragments of the nucleus and cytoplasm break off in membrane-bound structures called apoptotic bodies. There are also biochemical changes in the plasma membrane, including the exposure of lipids such as phosphatidylserine, which is normally on the inner face of the plasma membrane. These alterations are recognized by receptors on phagocytes, and apoptotic bodies and cells are rapidly engulfed and eliminated, without ever having elicited a host inflammatory response. Furthermore, phagocytosis of apoptotic cells may induce the production of antiinflammatory mediators by macrophages. The best evidence for the involvement of the two apoptotic pathways in the elimination of mature 338 Chapter 15 Immunologic Tolerance and Autoimmunity self-reactive lymphocytes is that genetic ablation of both in mice results in systemic autoimmunity. These two death pathways may function in different ways to maintain self-tolerance. When T cells avidly recognize self antigens, they may directly activate Bim, which triggers death by the mitochondrial pathway, as described earlier. The Bim-dependent mitochondrial pathway of apoptosis is also involved in negative selection of selfreactive T cells in the thymus (described earlier) and in the contraction phase (decline) of immune responses after the initiating antigen has been eliminated (see Chapter 9). Repeated stimulation of T cells results in the coexpression of the death receptor Fas and its ligand Fas-L, and engagement of Fas triggers apoptotic death. When T cells are repeatedly activated, FasL is expressed on the cell surface, and it binds to surface Fas on the same or adjacent T cells. This activates a cascade of caspases, which ultimately cause the apoptotic death of the cells. The same pathway of apoptosis may be involved in the elimination of self-reactive B lymphocytes also in the periphery (discussed later). Factors That Determine the Tolerogenicity of Self Antigens Studies with a variety of experimental models have shown that many features of protein antigens determine whether these antigens will induce T cell activation or tolerance (Table 15. These antigens are expressed in generative lymphoid organs, where they are recognized by immature lymphocytes. In peripheral tissues, self antigens engage antigen receptors of specific lymphocytes for prolonged periods and without inflammation or innate immunity. The nature of the dendritic cell that displays antigens to T lymphocytes is an important determinant of the subsequent response. Dendritic cells that are resident in lymphoid organs and nonlymphoid tissues may present self antigens to T lymphocytes and maintain tolerance. Tissue dendritic cells are normally in a resting (immature) state and express low levels of costimulators; some of them may traffic at a low level from epithelia even at steady state (in the absence of infection or inflammation). As we will discuss later, local infections and inflammation may activate resident dendritic cells, leading to increased expression of costimulators, breakdown of tolerance, and autoimmune reactions against tissue antigens. There is great interest in manipulating the properties of dendritic cells as a way of enhancing or inhibiting immune responses for therapeutic purposes. These concepts are based largely on experimental models in which antigens are administered to mice or are produced by transgenes expressed in mice. One of the continuing challenges in this field is to define the mechanisms by which various normally expressed self antigens induce tolerance, especially in humans. Short-lived (eliminated by immune response) Subcutaneous, intradermal; absence from generative organs Antigens with adjuvants: stimulate helper T cells Mature dendritic cells: High levels of costimulators Features That Favor Tolerance Prolonged, leading to persistent antigen receptor engagement Intravenous, mucosal; presence in generative organs Antigens without adjuvants: absence of costimulation Immature (resting) dendritic cells: Low levels of costimulators and cytokines B Lymphocyte Tolerance 339 plays a role in preventing antibody responses to protein antigens.
A Airway Piaw B Airway Piaw Poaw Poaw 755 mm Hg 760 mm Hg 760 mm Hg Ptm = 5 Poaw 760 mm Hg 765 mm Hg Poaw 760 mm Hg Ptm = + 5 Positive Transmural Pressure +5 torr Negative Transmural Pressure 5 torr Negative transmural pressure is said to exist when the pressure is greater outside the airway than the pressure inside the airway arthritis in dogs glucosamine dosage 75 mg indomethacin with mastercard. Transpulmonary pressure (Ptp) is the difference between the alveolar pressure (Palv) and the pleural pressure (Ppl) rheumatoid arthritis factor normal range buy 50 mg indomethacin mastercard. Ptp 5 Palv 2 Ppl For example arthritis in back causing hip pain buy discount indomethacin 75 mg, if the Ppl is 755 mm Hg and the Palv is 760 mm Hg arthritis zehengrundgelenk discount indomethacin 25 mg without prescription. Ptp 5 Palv 2 Ppl 5 760 mm Hg 2 755 mm Hg 5 5 mm Hg Or reverse arthritis with diet 25 mg indomethacin buy, if the Palv is 763 mm Hg and the Ppl is 758 mm Hg. In the normal lung, the Palv is always greater than the Ppl, which, in turn, maintains the lungs in an inflated state. A Gas Flow Palv = 757 mm Hg 3 mm Hg +3 mm Hg Pbs = 760 mm Hg Pbs = 760 mm Hg Transthoracic Pressure Gas Flow Palv = 763 mm Hg B Inspiration Expiration Transthoracic pressure (Ptt) is the difference between the alveolar pressure (Palv) and the body surface pressure (Pbs). Ptt 5 Palv 2 Pbs For example, if the Palv is 757 mm Hg and the Pbs is 760 mm Hg. Ptt 5 Palv 2 Pbs 5 757 mm Hg 2 760 mm Hg 5 23 mm Hg Or, if the Palv is 763 mm Hg and the Pbs is 760 mm Hg. The Ptt is the pressure responsible for expanding the lungs and chest wall in tandem. Technically, there is no real difference between the transrespiratory pressure (Prs) and the transthoracic pressure (Ptt). Clinical Connection 2-2 Abdominal Paradox (diaphragm fatigue) During normal resting inspiration, the diaphragm descends, and the external intercostal muscles lift the ribs up and outward to increase thoracic volume. During passive exhalation, the diaphragm moves back to its upward resting position and the abdomen moves inward to fill the void as the diaphragm and lungs move upward. This action decreases the thoracic volume, which, in turn, increases the alveolar pressure and causes gas to move out of the lungs. As the diaphragm becomes ineffective, the accessory muscles of inspiration-that is, the external intercostal, scalene, sternocleidomastoid, pectorals major, and trapezius muscles-attempt to maintain ventilation by becoming more active. Unfortunately, this condition can alter the normal mechanics of breathing as follows: As the accessory muscles of inspiration work to lift the ribs up and outward, the increase in thoracic volume will cause a resultant decrease in intrathoracic pressure. When the diaphragm is fatigued or paralyzed, it will be sucked upward by the negative intrathoracic pressure. During expiration, as the chest wall returns to its resting position, the thoracic volume decreases, and the intrathoracic pressure rises. The increased intrathoracic pressure, in turn, pushes the passive diaphragm downward and causes the abdomen to move outward. During exhalation, the chest wall decreases (which is normal), while the abdomen moves outward (which is not normal). In response to the low lung compliance, the infant-via their diaphragm-must generate a greater than normal negative pressure during inspiration. This action, in turn, causes their abdominal area to protrude outward (which is normal), and the substernal area and soft tissue between their ribs to move inward (which is not normal). During exhalation, the abdominal area moves inward and the substernal area and soft tissue between the ribs move back to their resting positions. When the diaphragm is fatigued or paralyzed, the chest wall expands with inspiration (which is normal), while the abdomen moves inwards (which is not normal). Normal Diaphragm Abdominal Paradox 92 Section one the Cardiopulmonary System-The Essentials Clinical Connection 2-3 the Harmful Effects of Pressure Gradients When the Thorax Is Unstable In the Clinical Application Case 1 (page 144), the respiratory therapist is called to assist in the care of a 22-year-old male motorcycle crash victim who presents in the emergency room with numerous abrasions, lacerations, and a very serious chest injury-multiple broken ribs over the right anterior chest. For example, each time the patient inhales, the transpulmonary and transthoracic pressure gradients cause his broken ribs to sink inward. To correct this problem, the therapist must place the patient on a positive-pressure ventilator. The positive-pressure ventilator eliminates the negative intrapleural pressure changes during each inspiration-which, in turn, stops the adverse effects of the transpulmonary and transthoracic pressure gradients during inspiration. The respiratory therapist uses positive-pressure ventilation to prevent the flailed portion of the chest from affecting breathing and to provide time for the broken ribs to heal. Pathology includes (1) double fracture of at least three or more adjacent ribs, (2) affected ribs cave in (flail) during inspiration, (3) atelectasis and lung collapse, (4) lung contusion or trauma, and (5) secondary pneumonia. Note the subcutaneous emphysema-which is the presence of air in the subcutaneous tissues (green arrow). That is, the chest wall has a natural tendency to move outward or to expand as a result of the bones of the thorax and surrounding muscles. The lungs have a natural tendency to move inward or collapse because of the natural elastic properties of the lung tissue. This lung chest wall relationship is often compared to that of two springs working against each other-that is, the chest wall works to spring outward; the lungs work to recoil inward. Clinically, the elastic forces of the lungs are routinely evaluated by measuring the lung compliance. For example, if an individual generates a negative pleural pressure change of 5 cm H2O during inspiration, and the lungs accept a new volume of 0. In other words, a negative 5-cm H2O pressure generated in the pleural space, around the lungs, will produce the same volume change as a positive 5-cm H2O pressure delivered to the tracheobronchial tree. A hysteresis is seen in the P-V curve because more energy is required to inflate the lungs than to deflate them. This is because the primary mechanism of lung inflation and deflation involves the sequential opening (called recruitment) and closing (called de-recruitment) of peripheral alveoli. In other words, at the beginning of a normal inspiration, many peripheral alveoli are closed. As inspiration continues, some of the peripheral alveoli are forced open-that is, recruited-by the increased transpulmonary pressure. In fact, during normal inspirations, the lung volume actually increases-to a large extent-because of the newly recruited alveoli, not because previously open alveolar diameters increase. In short, more energy is needed during inspiration for the recruitment process-mostly to overcome the molecular adhesive forces of surface tension. These molecular adhesive forces are essentially absent in alveoli that are already open during exhalation. When lung compliance is increased, the lungs accept a greater volume of gas per unit of pressure change. Note that during inspiration, the lung compliance is initially very low, and then progressively increases in the middle of the curve, and then again progressively decreases as the lungs expand to their full capacity. For example, with a consistent pressure change of 5 cm H20, the P-V curve shows a low lung volume changes between 10 and 15 cm H2O (a), a high-volume change between 30-35 cm H2O (B), and a low lung compliance with little to no volume change between 60-65 cm H2O little to no volume change between 60-65 cm H2O (c). As a result, the chest wall works to offset the normal elastic properties of the lungs. If unopposed, the normal compliance of both the lungs and chest wall are about equal at 0. However, because the lungs are enclosed within the thorax-and attached to the internal surface of the chest wall-the two elastic systems function as springs that naturally recoil away from each other. In this case, the patient is forced to generate high intrapleural pressure changes-with little, or no, volume change. How long do you think you could breathe at this level of your pressure-volume curve As a respiratory therapist, you will be treating many patients who have had this experience with every acute asthmatic episode. Asthma is characterized by periodic episodes of (1) reversible bronchial smooth muscle constriction, called bronchospasm; (2) airways inflammation, which results in mucosal edema and airways swelling; (3) excessive production of thick, whitish bronchial secretions; (4) mucous plugging; and (5) air trapping and hyperinflation of the alveoli. This condition forces the patient to generate high intrapleural pressure changes-with little or no volume change-and the work of breathing increases. Other restrictive lung disorders that can cause the pressure-volume curve to shift to the right include pneumonia, pneumothorax, pleural effusion, acute respiratory distress syndrome, pulmonary edema, and interstitial lung disease. Pathology includes the partial or total collapse of previously expanded alveoli, which result in (1) the prevention of respiratory exchange of carbon dioxide and oxygen in that part of the lung and (2) reduced lung compliance. Collapsed alveoli Lack of oxygen exchange Normal alveoli and capillaries chapter 2 Ventilation 99 turn, decreases the compliance of each elastic system to about one-half of the individual components- or 0. On the other hand, a pulmonary disorder that causes the lungs to break away from the chest wall. Elastance is the natural ability of matter to respond directly to force and to return to its original resting position or shape after the external force no longer exists. Thus, lungs with high compliance (greater ease of filling) have low elastance; lungs with low compliance (lower ease of filling) have high elastance. Note that elastance is the reciprocal of compliance for only a truly elastic body. Because the normal lungchest wall is not a total, or absolute, elastic mechanism, it functions in a more sigmoidal than linear manner. When the force exceeds the elastic limits of the substance, the ability of length to increase in response to force rapidly decreases. Thus, over the normal physiologic range of the lungs, volume varies directly with pressure. The lungs behave in a manner similar to the spring, and once the elastic limits of the lung unit are reached, little or no volume change occurs in response to pressure changes. Clinically, this phenomenon explains a hazard associated with mechanical ventilation. That is, if the pressure during mechanical ventilation (positive-pressure breath) causes the lung unit to expand beyond its elastic capability, the lung unit could rupture, allowing alveolar gas to move into the pleural space, and thus causing the lungs to collapse. When a truly elastic body-such as the spring in this illustration-is acted on by 1 unit of force, the elastic body will stretch 1 unit of length; when acted on by 2 units of force, it will stretch 2 units of length; and so forth. When the force goes beyond the elastic limit of the substance, however, the ability of length to increase in response to force quickly ceases. Once the elastic limits are reached, however, little or no volume change occurs in response to pressure change. Increasing Alveolar Pressure Increasing Alveolar Volume Volume level Volume level doubles Volume level triples 5 cm H2O 10 cm H2O 15 cm H 2O 20 cm H 2O 25 cm H 2O 30 cm H 2O Rupture Volume level increases very little Volume level beyond the elastic limit of the lung unit Increasing Volume Increasing Force Clinical Connection 2-6 Positive-Pressure Ventilation Clinically, when the patient is placed on a positivepressure ventilator, the intrapleural pressures, intra-alveolar pressures, and the movement of the diaphragm will all be quite different than the normal mechanisms of pulmonary ventilation. As the pressure progressively increases in the alveoli during inspiration, the intrapleural pressure also increases. Expiratory Phase of Positive-Pressure Ventilation During exhalation, the intra-alveolar pressure decreases toward atmospheric pressure and allows the elastic properties of the lungs to return to their normal resting level-similar to the decreased positive pressure that occurs in an elastic balloon that How a positive pressure breath from a mechanical ventilator affects the intra-alveolar pressure, intrapleural pressure, the excursion of the diaphragm, and gas flow during inspiration and expiration. Mechanical Ventilation Positive Pressure Breath (30 cm H2O Pressure Above Atmospheric Pressure) Inspiration Intra-alveolar pressure progressively increases above atmospheric pressure Intrapleural pressure progressively increases above atmospheric pressure Diaphragm is progressively pushed downward Expiration Intra-alveolar pressure progressively decreases toward atmospheric pressure Intrapleural pressure progressively decreases to its resting level (below the atmospheric pressure) Diaphragm progressively moves upward to its resting level A Gas Flow B End-Inspiration Intra-alveolar pressure is 30 cm H2O above atmospheric pressure Intrapleural pressure is about 30 cm H2O above atmospheric pressure Downward movement of diaphragm stops End-Expiration Intra-alveolar pressure in equilibrium with atmospheric pressure Intrapleural pressure holds at resting level (below the atmospheric pressure) Upward movement of diaphragm stops No Gas Flow + + + + + + C Gas Flow + D No Gas Flow 0 + + chapter 2 Ventilation 103 Clinical Connection 2-6, Continued is being allowed to return to the atmospheric pressure during deflation. This means that the high intraalveolar pressure moves in the direction of the low atmospheric pressure until the intra-alveolar pressure is in equilibrium with the atmospheric pressure. At end-expiration, the intra-alveolar pressure is in equilibrium with atmospheric pressure. The intrapleural pressure is held at its resting level that, under normal circumstances, is below atmospheric pressure. The administration of positive-pressure ventilation may also cause a number of adverse side effects, including lung rupture and gas accumulation between the lungs and chest wall (tension pneumothorax) and decreased cardiac output and blood pressure (see Clinical Connection 27). Clinical Connection 2-7 Hazards of Positive-Pressure Ventilation the respiratory therapist must carefully monitor the patient on mechanical ventilation for a number of adverse effects associated with positivepressure ventilation-including a sudden tension pneumothorax and decreased cardiac output and blood pressure. Tension Pneumothorax A patient receiving high positive pressures during mechanical ventilation is always at some degree of risk of a sudden lung rupture and resulting pneumothorax. A pneumothorax in which the intrapleural pressure is greater than the intraalveolar (or atmospheric) pressure is called a tension pneumothorax. At the bedside, a number of clinical signs and symptoms can develop that indicate a sudden tension pneumothorax: (1) increased heart rate, (2) diminished or absent breath sounds on the affected side, (3) hyperresonant percussion note over the pneumothorax, (4) tracheal shift to the unaffected side, (5) displaced heart sounds, (6) an enlarged and immobile chest on the affected side, and (7) decreased cardiac output and blood pressure. A chest X-ray is used to confirm the extent of a pneumothorax and typically reveals (1) gas accumulation in the pleural cavity, (2) depressed diaphragm, and (3) shift of the mediastinum to the unaffected side of the chest. Note the collapsed right lung, the depressed right diaphragm, and the heart and mediastinum pushed to the unaffected side. Decreased Cardiac Output and Blood Pressure the decreased cardiac output and blood pressure associated with a tension pneumothorax are caused by the positive intrapleural pressure-which is caused by the gas accumulation in the pleural cavity. As a result of the positive pleural pressure, the major intrathoracic veins-the inferior and superior vena cava-are compressed. In general, the more severe the tension pneumothorax, (1) the greater the positive pressure in the pleural cavity, (2) the more the major intrathoracic veins will be compressed, and (3) the more cardiac output will be reduced. Because of the high resistance encountered by blood returning to the right atrium of the heart, blood pooling develops in the peripheral vascular system-mainly the legs, arms, and abdominal viscera. Chest X-ray of a right-sided tension pneumothorax caused by positive pressure ventilation. Note, in both A and B, the collapsed right lung (horizontal arrow in B), the depressed right diaphragm (vertical arrow in B), and the heart and mediastinum pushed to the unaffected side. Clinical Connection 2-8 Negative-Pressure Ventilation In 1928, Drinker and Shaw invented the first modern and practical negative-pressure ventilator-most commonly known as the "iron lung. The iron lung was made famous for its important contributions during the poliomyelitis epidemics of the 1930s and 1950s. This gas flow continues until the intra-alveolar pressure and the atmospheric pressures are in equilibrium. Once the equilibrium point is reached, 4 Also called the Drinker tank or Shaw tank. To initiate expiration, the piston mechanism releases the negative pressure, which, in turn, allows the elastic recoil forces of the thorax and lungs to return to their normal-and smaller-size (decreased volume). This action causes the intra-alveolar pressure to increase, creating a pressure gradient between the intra-alveolar pressure and atmospheric pressure. This gas flow will continue until the intra-alveolar pressure and the atmospheric pressure are in equilibrium. There are several disadvantages associated with the full-body iron lung, including (1) patient access, (2) abdominal venous blood pooling, (3) decreased venous return, and (4) decreased cardiac output and blood pressure. Although the iron lung is still being utilized for long-term ventilation today, the prominent negative-pressure devices used are (1) the Porta-lung (offers the same level of efficiency as the iron lung, but in a lightweight portable unit), (2) the chest cuirass (an upper body only shell- named after the body armor worn by medieval soldiers), or (3) the body suit.
Order indomethacin mastercard. Psoriatic arthritis - causes symptoms diagnosis treatment pathology.
References
- Haas M, Spargo BH, Wit EJ, et al: Etiologies and outcome of acute renal insufficiency in older adults: a renal biopsy study of 259 cases, Am J Kidney Dis 35:433-447, 2000.
- Saussele S, Lauseker M, Gratwohl A, et al. Allogeneic hematopoietic stem cell transplantation (allo SCT) for chronic myeloid leukemia in the imatinib era: evaluation of its impact within a subgroup of the randomized German CML Study IV. Blood 2010;115(10):1880-1885.
- Shine TS, Harrison BA, De Ruyter ML, et al. Motor and somatosensory evoked potentials: their role in predicting spinal cord ischemia in patients undergoing thoracoabdominal aortic aneurysm repair with regional lumbar epidural cooling. Anesthesiology 2008;108:580-7.
- Robertson MM, Trimble MR, Townsend HR. Phenomenology of depression in epilepsy. Epilepsia 28: 364-372, 1987.