- info@careermakers.edu.np
- +977 1 4423870
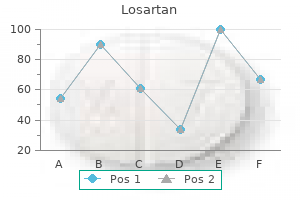
Losartan
Nina Holland PhD
- Adjunct Professor, Emerita, Environmental Health Sciences
https://publichealth.berkeley.edu/people/ernest-hook/
Note: I n the appropriate clinical and radiologic se ing diabetes mellitus versi indonesia losartan 50 mg purchase on line, the findings are compatible with sarcoidosis diabetes symptoms and symptoms purchase 50 mg losartan visa. Fungal Infection Fungal infections should always be on the differential when there is granulomatous inflammation (Table 3 diabetes type 1 life expectancy order losartan 25 mg on line. S ome of the most important fungal diseases to be aware of are those caused by dimorphic fungi managing diabetes 55 buy losartan cheap online, which exist as yeasts at 37°C (human body temperature) and molds at colder temperatures; these include histoplasmosis diabetes type 1 genetic losartan 25 mg with mastercard, blastomycosis, coccidioidomycosis, and paracoccidioidomycosis. I nvasive aspergillosis, zygomycosis, and candidiasis tend to invade pulmonary tissue and blood vessels, especially in immunocompromised patients. Worldwide Thick, uniform, septate hyphae with 45-degree angle branching Fruiting bodies associated with calcium oxalate crystals Background typically shows abundant neutrophils and necrosis Zygomycosis Rhizopus sp. Worldwide Yeast, can elongate into true or broad-b ased pseudohyphae ("sausage links") 4-4 0 3-6 Other filamentous fungi 3-2 5 Aspergillus, Candida 3-4 May be mistaken for Aspergillus or Cryptococcus spp. A double-layered cell wall, which is characteristic of Blastomyces, can be appreciated (Pap stain). In contrast to Aspergillus hyphae, these are nonseptate with variable widths (Pap stain). Matrix-Containing Lesions Matrix-containing lesions include those that produce extracellular matrix material, most notably pulmonary hamartoma (benign) and adenoid cystic carcinoma (malignant). This section will focus on matrix-containing tumors found in the lungs, where identification of the matrix component facilitates the diagnosis. Checklist: Etiologic Considerations for Matrix-Containing Lesions Pulmonary Hamartoma Adenoid Cystic Carcinoma Pulmonary Hamartoma Hamartomas are the most common benign lung neoplasm and are often found incidentally in the peripheral lung as a well-circumscribed solitary single nodule (uncommonly in a central location or as multiple nodules). Histologically, hamartomas show abnormal growth of normal mesenchymal elements, most commonly cartilage, adipose tissue, and smooth muscle with entrapped ciliated, respiratory-type epithelium. Fibromyxoid stroma (upper right) is present in a background of benign epithelial cells (Diff-Quik stain). There are abundant benign epithelial cells associated with fibromyxoid stroma (Diff-Quik stain). Adenoid Cystic Carcinoma A denoid cystic carcinoma is one of the most common salivary glandtype tumor found in the lung, most commonly occurring in the trachea, but also in the major bronchi. The cells are basaloid and uniform and form three-dimensional clusters around globules of hyaline material (Diff-Quik stain). A mixture of matrix material and neoplastic cells should suggest the possibility of a salivary gland neoplasm, though the morphology seen here is not specific for adenoid cystic carcinoma (Pap stain). The small hyperchromatic cells form three-dimensional clusters around a large, homogenous translucent globule (Pap stain). Extras Curschmann Spirals Curschmann spirals are strands of mucus that are characteristically coiled due to their formation as inspissated mucous plugs in the subepithelial mucous gland ducts. A lthough they are more frequently seen in association with asthma and smoking, they can be seen in other types of specimens and are generally a nonspecific finding. Ferruginous Bodies Ferruginous bodies are fiber particles encrusted with proteins containing iron salts. The presence of ferruginous bodies should be specifically mentioned in the pathology report to ensure that the patient is screened for mesothelial risk factors, if not already performed. They can be seen in conditions associated with pulmonary edema, although they are nonspecific and have no clinical significance. Psammoma Bodies Psammoma bodies are concentrically laminated calcifications that are associated with malignant neoplasms (especially those with papillary architecture) as well as benign diseases. A morphous proteins can also be seen in viral infections and Pneumocystis pneumonia. There are scattered, dense, amorphous globules in a dirty, frothy background (Pap stain). Pneumocystis jirovecii Pneumonia caused by Pneumocystis jirovecii typically presents in immunocompromised individuals and manifests as bilateral pulmonary infiltrates on chest X-ray. Giemsa stains show the cyst outlines and stains the intracystic trophozoites as discrete blue dots. These lesions are characterized by hemorrhagic infarcts, which makes sampling less likely to yield Aspergillus hyphae. I n these high-risk cases, fungal stains and microbiologic cultures should be performed. A lthough cytology cannot determine if the aspergillosis is invasive or not, the presence of hyphae in the appropriate clinical and radiologic setting is sufficient to prompt therapy initiation. The cytomorphologic features and immunohistochemical profile of these two tumors can overlap. Clinicoradiologic correlation to look for multiple lung nodules or other sites of metastatic tumor and/or comparison with the primary tumor (if available) may assist in making the distinction. The carcinoma is poorly differentiated, and the cells seen here could also possibly represent a primary lung adenocarcinoma or squamous cell carcinoma (Diff-Quik stain). Some cells have dense cytoplasm, and there are spaces between some neighboring cells, suggesting the possibility of squamous differentiation (Pap stain). The carcinoma cells are focally positive for uroplakin, a specific marker for a urothelial origin. Immunohistochemical results should be interpreted with caution if they conflict with the clinical impression (uroplakin immunostain). The clinical impact of solid and micropapillary patterns in resected lung adenocarcinoma. Updated molecular testing guideline for the selection of lung cancer patients for treatment with targeted tyrosine kinase inhibitors: guideline from the College of American Pathologists, the International Association for the Study of Lung Cancer, and the Association for Molecular Pathology. Cytologic-histologic correlation of programmed death-ligand 1 immunohistochemistry in lung carcinomas. Optimal immunohistochemical markers for distinguishing lung adenocarcinomas from squamous cell carcinomas in small tumor samples. Immunohistochemical algorithm for differentiation of lung adenocarcinoma and squamous cell carcinoma based on large series of whole-tissue sections with validation in small specimens. Nonspecific reactivity of polyclonal napsin a antibody in mucinous adenocarcinomas of various sites: a word of caution. Diagnosis of lung cancer in small biopsies and cytology: implications of the 2011 International Association for the Study of Lung Cancer/American Thoracic Society/European Respiratory Society classification. Molecular genetic alterations in thyroid transcription factor 1-negative lung adenocarcinoma in cytology specimens: a subset with aggressive behavior and a poor prognosis. Pulmonary non-small cell carcinoma with morphologic features of adenocarcinoma or "non-small cell carcinoma favor adenocarcinoma" in cytologic specimens share similar clinical and molecular genetic characteristics. Usefulness of immunohistochemical and histochemical studies in the classification of lung adenocarcinoma and squamous cell carcinoma in cytologic specimens. Immunohistochemical subtyping of nonsmall cell lung cancer not otherwise specified in fine-needle aspiration cytology: a retrospective study of 103 cases with surgical correlation. The role of cytologic evaluation of pleural fluid in the diagnosis of malignant mesothelioma. Cytogenetics and fluorescence in situ hybridization as adjuncts to cytology in the diagnosis of malignant mesothelioma. Unsuspected metastatic renal cell carcinoma diagnosed by fine needle aspiration biopsy. Cytologic diagnosis of bronchial mucoepidermoid carcinoma by fine needle aspiration biopsy. Survival analysis of 200 pulmonary neuroendocrine tumors with clarification of criteria for atypical carcinoid and its separation from typical carcinoid. The pathologic classification of neuroendocrine tumors: a review of nomenclature, grading, and staging systems. Diagnostic issues with cytopathologic interpretation of lung neoplasms displaying high-grade basaloid or neuroendocrine morphology. Insulinoma-associated protein 1 immunostain: a diagnostic tool for pulmonary small cell carcinoma in cytology. The use of immunohistochemistry improves the diagnosis of small cell lung cancer and its differential diagnosis. Ki-6 7 antigen in lung neuroendocrine tumors: unraveling a role in clinical practice. Prognostic implications of neuroendocrine differentiation and hormone production in patients with Stage I nonsmall cell lung carcinoma. Endobronchial ultrasound-transbronchial needle aspiration for lymphoma in patients with low suspicion for lung cancer and mediastinal lymphadenopathy. Inflammatory fibrosarcoma: update, reappraisal, and perspective on its place in the spectrum of inflammatory myofibroblastic tumors. Solitary fibrous tumor clinicopathologic, immunohistochemical and molecular analysis of 28 cases. Malignant fat-forming solitary fibrous tumor (so-called "lipomatous hemangiopericytoma"): clinicopathologic analysis of 14 cases. Sarcomatoid carcinoma of the lung: histologic criteria and common lesions in the differential diagnosis. Fine-needle aspiration cytology of an unusual primary lung tumor, chondrosarcoma: case report. Epithelioid hemangioendothelioma of the lung diagnosed by transesophageal endoscopic ultrasound-guided fine needle aspiration: a case report. Transthoracic fine-needle aspiration biopsy of pulmonary spindle cell and mesenchymal lesions: a study of 61 cases. Clinicopathological and immunohistochemical analysis of spindle-cell carcinoid tumour of the lung. Identification of infectious organisms in cytopathology: a review of ancillary diagnostic techniques. Diagnosis of histoplasmosis in bronchoalveolar lavage fluid by intracytoplasmic localization of silver-positive yeast. Unusual forms of immature sporulating Coccidioides immitis diagnosed by fine-needle aspiration biopsy. The cytomorphologic spectrum of salivary gland type tumors in the lung and mediastinum: a report of 16 patients. Monoclonal immunofluorescence compared with silver stain for investigating Pneumocystis carinii pneumonia. Metastatic metaplastic breast carcinoma mimicking pulmonary squamous cell carcinoma on fine-needle aspiration. The apical surfaces of the hepatocyte cords face the sinusoids, which carries blood from the portal vein and hepatic artery to the central vein. The basal surfaces of the hepatocyte cords form bile canaliculi, which provide a conduit for bile drainage from the hepatocytes to bile ducts that eventually leave the liver. The hepatocytes are polygonal cells with round nuclei and abundant pink cytoplasm (H&E). Vacuolization of the cytoplasm due to fat or glycogen accumulation is also common and may or may not be pathologic. Benign hepatocytes are present in cytological specimens as single cells or in fragments/trabeculae, typically no more than two cells wide. Some nuclear size variation and occasional binucleation is normal (Diff-Quik stain). When sampled by aspiration, the bile duct epithelial cells are usually present in small groups and fragments, in contrast to sheets. Hepatocytes have abundant cytoplasm and lower nuclear to cytoplasmic ratios, as compared with the ductal epithelium (Diff-Quik stain). Kupffer Cells Kupffer cells are specialized macrophages lining the liver sinusoids. I n aspirate smears, Kupffer cells have ovoid or elongated nuclei and scant cytoplasm and are often a ached to hepatocytes. Hepatocellular Pattern the hepatocellular pa ern includes benign/reactive and neoplastic lesions composed primarily of hepatocytes, which can range from bland-appearing to cytologically atypical. Benign hepatocytes are intermixed with fibroblasts, which traverse across the hepatocytes (Pap stain). Note that the benign hepatocytes have no nuclear atypia or pleomorphism, and there is no necrosis or mitoses, which can be seen in cirrhosis (Diff-Quik stain). Regenerative Nodules Regenerative nodules in the liver are generally seen in association with cirrhosis, where the normal liver architecture is transformed by bands of bridging fibrosis, resulting in nodules of regenerating hepatocytes. Small thin fragments and scattered benign-appearing hepatocytes are seen in a background of fibrotic strands and lymphocytes (Pap stain). The regenerating hepatocytes in this fragment have prominent nucleoli and increased nuclear to cytoplasmic ratio but no architectural features to suggest malignancy. The hepatocytes are benign-appearing with binucleation, moderate anisonucleosis, and abundant granular/vacuolated cytoplasm (Diff-Quik stain). Bile accumulation within hepatocytes may be seen, but bile ducts are not present within the lesion (Diff-Quik stain). The hepatocytes are benign-appearing with abundant vacuolated cytoplasm (Pap stain). The smear is highly cellular and contains sharply outlined trabecular groups (Pap stain). There are clusters of tumor cells with clear hepatocellular differentiation, although the nuclear to cytoplasmic ratio is higher. Background solitary tumor cells are naked nuclei stripped of cytoplasm (Diff-Quik stain). The neoplastic cells are monotonous with minimal nuclear atypia, although there is reduced cytoplasm. The neoplastic cells resemble benign hepatocytes and have regular, uniform nuclei with fine, granular chromatin (Pap stain). In this instance, there is increased pleomorphism and nuclear atypia, with eccentric nuclei and very prominent central nucleoli, but the cells maintain some features of hepatocellular differentiation (such as abundant granular cytoplasm) (H&E, cell block). The neoplastic cells are irregular and pleomorphic with enlarged nuclei and prominent nucleoli (Diff-Quik stain).
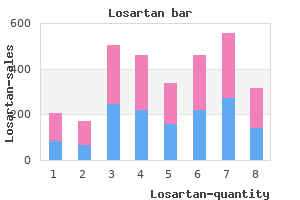
Pulmonary valve replacement prior to pregnancy is advised in women with severe pulmonary regurgitation who are symptomatic or in absence of symptoms when there is significant right ventricular systolic dilation or dysfunction [7] diabetic diet food chart buy cheap losartan on line. During pregnancy diabetes prevention flyer order line losartan, serial clinical and echocardiographic assessment should be performed during and early postpartum to evaluate the size and function of the right ventricle and the severity of pulmonary and tricuspid regurgitation blood glucose meter accuracy buy losartan 25 mg with mastercard. The septal and posterior leaflets of the tricuspid valve are displaced apically and malformed leading to atrialization of part of the right ventricle diabetic lunch ideas losartan 50 mg buy with amex. The valve abnormalities are associated with tricuspid regurgitation diabetes prevention study 50 mg losartan for sale, or much less commonly, tricuspid stenosis. The functional right ventricle may be hypoplastic, or dilated, if there has been chronic volume overload from tricuspid regurgitation. Right atrial dilation and accessory pathways increase the risk of atrial arrhythmias. The volume load of pregnancy can contribute to cardiac complications in women with Ebstein anomaly. Women with interatrial shunt may demonstrate worsening cyanosis during pregnancy because of the inability of the right ventricle to handle the volume load of pregnancy leading to higher right atrial pressure promoting right to left shunting. Women with Ebstein anomaly who have symptoms or cyanosis at rest or with exercise should have repair prior to pregnancy. Complete transposition of the great arteries Complete transposition of the great arteries is a rare cyanotic congenital cardiac condition in which there is ventriculoarterial discordance. Patients would have undergone repair in childhood, having had either an atrial switch operation (Mustard or Senning operation) or an arterial switch operation (Jatene operation). The difference in childhood surgery drives substantial differences in clinical course as adults. Atrial switch operations (Mustard/Senning operation) the older surgical approach was the atrial switch operation (Mustard or Senning operation). This operation diverted blood at the atrial level by constructing intraatrial baffles. While this approach corrected cyanosis and improved longevity, the operation left patients with a subaortic right ventricle supporting the systemic circulation and a tricuspid valve in the subaortic position prone to regurgitation, as well as a propensity to arrhythmias. The most common complications late after an atrial switch operation are atrial and ventricular arrhythmias, tricuspid regurgitation, and subaortic right ventricular systolic dysfunction and failure. Arrhythmias and heart failure are the most common cardiac complications during pregnancy, although the rates of cardiac complications vary among studies [11,13,4446]. During pregnancy, the hemodynamic load on the subaortic right ventricle contributes to worsening ventricular function, tricuspid valve regurgitation, and clinical heart failure. These hemodynamic changes can also precipitate arrhythmias; atrial arrhythmias, ventricular tachycardia, and cardiac arrest are reported. Some women who develop deterioration in subaortic right ventricular function or worsening of tricuspid regurgitation do not recover after pregnancy [11,13]. There is no way to predict which women will develop permanent deterioration in subaortic ventricular function, and all women should understand this risk before embarking on a pregnancy. Careful clinical and echocardiographic surveillance during pregnancy is important for early detection of heart failure. Women with atrial switch operations who have severe subaortic right ventricular dysfunction and/or severe tricuspid regurgitation should be advised against pregnancy. There are significant perinatal risks as well from preterm deliveries and low birth weight babies [11]. Young women following arterial switch operation have recently reached childbearing age. In an early reported cohort of 13 term pregnancies in women with arterial switch operations, one woman with ventricular dysfunction had ventricular tachycardia during pregnancy, and one woman with a mechanical valve had valve thrombosis [47]. In women with preserved ventricular function and no significant great vessel dilation or valve disease, pregnancy will likely be well tolerated. Congenitally corrected transposition of the great arteries Congenitally corrected transposition of the great arteries, or atrioventricular and ventriculoarterial discordance, is rare. With this anatomical arrangement, the morphologic right ventricle serves as the subaortic ventricle supporting the systemic circulation. Late complications may be secondary to subaortic right ventricular dysfunction, tricuspid valve regurgitation, conduction disease including complete heart block or other associated congenital cardiac lesions. Although many women do well during pregnancy, deterioration in subaortic right ventricular function and tricuspid valve regurgitation, heart failure, and atrial arrhythmias are reported [48,49]. Women with good functional class and normal subaortic ventricular function are unlikely to develop cardiac complications. Women with severe subaortic right ventricular dysfunction, with or without tricuspid valve regurgitation, are at risk for further deterioration in ventricular function and clinical heart failure during pregnancy. Close surveillance with serial transthoracic echocardiograms is advised, and arrhythmias should be sought and rapidly controlled. Truncus arteriosus Truncus arteriosus is a rare congenital lesion in which a single arterial vessel exits the heart giving rise to the pulmonary and systemic circulation. Truncus repair involves isolating the pulmonary arteries from the truncus and reattaching them to the right ventricle with a conduit. Conduit failure, truncal ("aortic") root dilation, truncal ("aortic") valve regurgitation, branch pulmonary artery stenosis, ventricular dysfunction, ischemia, and pulmonary vascular disease have all been described late after repair. Few cases of pregnancy have been reported in women born with truncus arteriosus; however, women without significant ventricular dysfunction or residual valve lesions will likely do well [50]. Fontan operation the Fontan operation, used to palliate patients with a single ventricle, has had several modifications since it was first introduced. Originally conceived for tricuspid atresia, its use has expanded to palliation of other single ventricle lesions. Caval flow enters directly into the pulmonary arteries without interposition of a subpulmonary ventricle: the superior vena cava is connected directly to the pulmonary arteries (Glenn operation, bidirectional cavopulmonary anastomosis), and the inferior vena cava is connected to the pulmonary arteries using one of right atrial to pulmonary artery connection, intraatrial conduit (lateral tunnel Fontan), or extracardiac conduit (extracardiac Fontan). Some women may have cyanosis due to arteriovenous malformations or Fontan fenestration. Failure of the Fontan circulation occurs in patients who, over time, develop diastolic or systolic dysfunction, atrioventricular valve regurgitation, and/or increase in pulmonary vascular resistance (overt pulmonary hypertension does not occur). The low-flow circuit also predisposes to thromboembolic complications, which, in the setting of Fontan physiology, can be fatal. Women following Fontan operations who have ventricular dysfunction, moderate to severe atrioventricular valvular regurgitation, cyanosis or protein-losing enteropathy should be advised against pregnancy. The hemodynamic changes that occur during pregnancy can destabilize the Fontan circulation. In a systematic review of studies published between 1986 and 2015, supraventricular arrhythmia occurred in 8. The prothrombotic state of pregnancy also increases the risk of thromboembolic complications [52,53]. Women with a history of arrhythmias or thromboembolic complications should receive anticoagulation during pregnancy. While some experts advocate anticoagulation therapy in all women with Fontan circulation during pregnancy, the benefit of anticoagulation needs to be weighed against the risk of bleeding, which is also increased in this population, reported in up to 25% of pregnancies [53]. Our group only uses anticoagulation therapy in pregnant women with the Fontan operation, who are at high risk for thromboembolic complications. Although maternal deaths are rare, careful patient selection for pregnancy is crucial. Shortened life span is expected following the Fontan operation and is a critical issue to sensitively explore and clarify during preconception counseling, since it may influence decisions regarding proceeding with pregnancy [17]. In addition to maternal cardiac risks, there are significant fetal and neonatal risks. The y axis represents the percent of pregnancies complicated by perinatal complications. Serial clinical and echocardiographic assessment should be performed during pregnancy and early postpartum to identify changes in ventricular function and atrioventricular valve regurgitation. The Fontan circulation is preload dependent and Valsalva maneuvers, blood loss or arterial or venous vasodilatation from medications during labor and delivery can result in circulatory collapse. The Norwood procedure is used as initial palliation of children with hypoplastic left heart syndrome. The operation is the first part of a staged procedure and involves the construction of a neoaorta and creation of an aortopulmonary shunt. This is followed by the creation of a bidirectional cavopulmonary shunt (Glenn operation) and eventually a Fontan operation. Women born with hypoplastic left heart syndrome and managed as described are only now reaching childbearing age, but pregnancy outcomes are not yet well described [54]. Cyanosis due to pulmonary hypertension and shunt reversal is discussed in the section on Eisenmenger syndrome that follows. While some women with cyanotic heart disease may experience an uncomplicated pregnancy, maternal death, heart failure, arrhythmias, hemoptysis, thromboembolic complications, cerebrovascular events, and endocarditis are reported [55,56]. In a study of 71 pregnancies in women with cyanotic heart disease, 27% were complicated by cardiac events. Women with resting oxygen saturation less than 85% should be advised against pregnancy because of maternal risk and expectation of very poor neonatal outcome [7]. Oxygen saturation should be monitored throughout labor and delivery and well into the postpartum period as well. Blood loss or hypotension from medications at the time of delivery or postpartum can lead to worsening right to left shunting. Eisenmenger syndrome Eisenmenger syndrome occurs as a complication of larger left to right shunts. Pulmonary arterial hypertension leads to reversal of the shunt, becoming bi-directional or rightto-left across the septal defect or aortopulmonary communication. Eisenmenger syndrome is a multisystem disease with cyanosis, secondary erythrocytosis, hyper viscosity syndrome, thromboembolic events, hemoptysis, cerebrovascular complications, renal dysfunction, gout, cholelithiasis, and hypertrophic osteoarthropathy. The y axis represents the percent of live births in women with cyanotic heart disease. The increased volume load of pregnancy and pregnancyassociated reduction in systemic vascular resistance predispose to further right-to-left shunting and worsening hypoxia as well as volume overload of the right heart. Hypoxemia can lead to further pulmonary vasoconstriction and pulmonary hypertensive crisis. Thromboembolic complications increase during pregnancy because of the hypercoagulable state. In a literature review of publications between 1997 and 2007, mortality in women with idiopathic pulmonary arterial hypertension, pulmonary arterial hypertension in association with congenital heart, and pulmonary arterial hypertension from other causes was 17%, 28%, and 33% respectively [25]. Reported causes of death include right heart failure, cardiogenic shock, arrhythmias and sudden death, thromboembolic complications, and pulmonary artery rupture. In addition to maternal mortality, morbidity is high due to right heart failure, arrhythmias, and nonfatal thromboembolic disease. Although a few studies from specialized centers have reported lower maternal mortality than previously reported [57,58], in view of the high maternal morbidity and mortality, women with significant pulmonary hypertension from any cause should be discouraged from pregnancy, and if pregnant offered termination as the safest option [7]. There have been significant advances in the treatment of pulmonary hypertension, and while it is likely that these advanced therapies can improve pregnancy outcomes, this has not been clearly demonstrated (see also Chapter 16). Women taking pulmonary arterial hypertension medications prior to pregnancy should continue the medications during pregnancy when possible. However, bosentan, and probably other endothelin receptor antagonists as well, is teratogenic, so alternative medications should be considered when possible. Cardiac decompensation can occur at the time of delivery, so careful planning is essential. Blood loss or hypotension from anesthetic agents or other drugs can lead to worsening right to left shunting, hypoxemia, pulmonary vasoconstriction, and a vicious spiral potentially to death. Vaginal deliveries are often possible with close monitoring, good pain management, and careful postpartum surveillance. Aggressive postpartum diuresis is helpful to prevent right heart failure, but caution is advised because over diuresis can be dangerous in women with Eisenmenger syndrome. Reported maternal mortality extends through the first week postpartum, so extended postpartum in-hospital monitoring for seven days or so is justified. Pregnancy outcomes and relative risk factors among Chinese women with congenital heart disease. Heart rate response during exercise and pregnancy outcome in women with congenital heart disease. Long-term outcome following pregnancy in women with a systemic right ventricle: is the deterioration due to pregnancy or a consequence of time Pregnancy-related obstetric and cardiologic problems in women after atrial switch operation for transposition of the great arteries. The effects of pregnancy on right ventricular remodeling in women with repaired tetralogy of Fallot. Effect of pregnancy on ventricular and aortic dimensions in repaired tetralogy of Fallot. Survival prospects and circumstances of death in contemporary adult congenital heart disease patients under follow-up at a large tertiary centre. Pregnancy complications in women with heart disease conceiving with fertility therapy. Adverse neonatal and cardiac outcomes are more common in pregnant women with cardiac disease. Anesthetic management of a consecutive cohort of women with heart disease for labor and delivery. Management of pregnancy in patients with complex congenital heart disease: a scientific statement for healthcare professionals from the American Heart Association. Comparison of pregnancy outcomes in women with repaired versus unrepaired atrial septal defect.
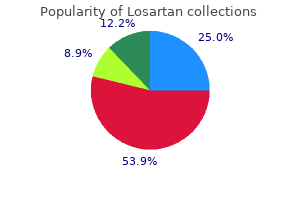
The intact placenta diabetes insipidus name origin cheap 25 mg losartan visa, as barrier for prevention or vehicle for administration route of therapeutic agents diabetes symptoms checklist cost of losartan, provides protection from drug effects and yet opportunity for fetal treatment [7] diabetes symptoms dry mouth purchase cheapest losartan. Maternal disease states and conditions that compromise optimal placental function may change the drug exposure level and risk diabetes labs losartan 25 mg purchase on line. Pharmacogenetic expression in maternal organs of drug elimination diabetes in dogs and itching cheap 25 mg losartan mastercard, as well as in the placenta, may vary among pregnant patients, with genetic polymorphisms in metabolizing enzymes and transporter proteins contributing to further variability in pharmacokinetics parameters. This, together with the pharmacogenomics of the disease state and receptor binding and sensitivity, creates less predictable disposition and response, and varying exposure risk to the fetus. Even the genotype of the unborn may play a role in placental and fetal drug metabolism and transplacental passage [8]. These issues extend to the early postpartum period, where reverting back to prepregnancy pharmacokinetics evolves with time, as does drug exposure to the infant via breast milk, and the specific drug physicochemical and partitioning properties that effect drug delivery via that route [9]. Utilization of therapeutic drug monitoring principles and techniques, with population pharmacokinetic parameter estimates and feedback plasma concentrations, assists in initiating and modifying maternal drug doses with more tailored accuracy, and help predict potential fetal exposure [10]. Clearly, more studies of the pharmacokinetics of drugs in pregnancy, modeling and simulation efforts using ex vivo systems and in vivo data collection are needed to enrich the database and guide the clinician toward proper drug choice and dosimetry [11,12]. There is still a dearth of published studies with direct comparisons of the pharmacokinetics of drugs in the pregnant/ postpartum and nonpregnant female, including cardiovascular agents [3]. Encouraging is the more than 150 studies featuring pharmacokinetics in pregnant patients posted on clinicaltrials. More studies and data on the pharmacokinetics of existing and new drugs in the mother and the fetus add valuable information to this narrative approach to provide the best available guidance to clinicians and patients. Physiologic changes and drug disposition in pregnancy Absorption Though changes in absorption due to pregnancy have overall less impact on systemic drug levels in pregnant patients than other pharmacokinetic changes, altered extent and rate of absorption require consideration. The absorption of orally administered drugs undergoes subtle changes during pregnancy [24]. With the increase in emesis seen in early pregnancy, the bioavailability and compliance with oral medication may be reduced if less drug is presented to the absorptive surface. Delayed gastric emptying, due to the continued rise in progesterone, may lengthen the time to peak concentrations. As the intestinal wall is capable of drug metabolism and subject to transporter effects, and drug metabolism interactions with grapefruit juice products, bioavailability and presystemic clearance may be altered. Similar reductions have been seen with nadolol when co-administered with green tea, with a potential muting of expected blood pressure response [17]. Moreover, single-nucleotide polymorphisms alter gene expression of these intestinal transport (pump) proteins and intestinal drug absorption. Food, aluminumcontaining, macrolides, and sedative-hypnotics decrease or increase the absorption rate of coadministered drugs [21]. Additionally, saturability of carrier-mediated absorption is seen with drugs such as amoxicillin and gabapentin, such that the higher the incremental dose, the lower will be the bioavailability [22,23]. With increases in regional blood flow and body fat composition during pregnancy, the uptake from tissue sites of injection of lipid soluble agents is generally expected to be faster, with an earlier time to peak concentration from nonintravenous parenteral administration, as observed for 17hydroxyprogesterone caproate in castor oil intramuscular injection given to prevent preterm labor when compared to nonpregnant females for other indications [24]. Less evidence is available for more rapid or complete absorption for more hydrophilic drugs [4]. The intrinsic physicochemical nature of certain drugs limits their intramuscular use. Superimposed heart failure limits the absorption rate of orally administered diuretics caused by gastrointestinal edema, delaying their peak effects, and in concert with pharmacodynamic factors, may produce an additional pharmacokinetic consideration for diuretic therapeutic resistance [25,26]. Other routes of drug administration generally retain their rates of absorption as for nonpregnant patients, although some changes may be seen with augmented regional blood flow. Biliary secretion with enterohepatic recirculation occurs with amiodarone, contributing in part to a biphasic elimination pattern of concentration decay after oral administration [29]. Pregnancy-associated intrahepatic cholestasis could further impose changes in absorption rate for lipid soluble drugs. Volume of distribution the space into which the drug disperses within the body is referred to as the volume of distribution (Vd in liters). It is important to standardize or normalize volume of distribution values to body weight (l/kg) or body surface area (l/m2), in order to compare patients of different disease states or conditions, body habitus and ages, or gestational period. More accurate is to describe this space as the "apparent" volume of distribution, as some drugs may conform to an actual physiologic volume. More restricted distribution volumes occur with drugs demonstrating high serum protein binding and relatively low tissue binding. In the case of Vd larger than total body water, both receptor-based and other tissues are involved, and these drugs will generally exhibit longer elimination halflives, as drug unbinds slowly from the deeper tissue stores back into the systemic circulation where they are cleared by the organs of elimination. As an example, amiodarone distributes extensively into adipose tissue, lengthening its latephase half-life to several weeks [29]. If one assumes complete bioavailability of a drug and instantaneous distribution. With drugs that are intermittently infused, the amount of drug cleared during the infusion must be accounted for if the infusion time is less than three to four elimination halflives to accurately calculate volume of distribution [31]. A two-compartment model, with exchange between the central and peripheral compartment, will first show rapid and then slow decay of the concentration, with eventual equilibrium between the compartments being met, the timing of which depending on the rates of movement from central to peripheral compartment and vice versa [31]. After intravenous bolus administration, digoxin distributes to the central compartment speedily and the peripheral compartment slowly, accounting for a relatively slower time to peak activity, as time is needed to occupy receptor sites in cardiac tissue (and other non-receptor muscle tissue) within the peripheral compartment [32]. Additionally, drawing serum concentrations prior to four to six hours, when intercompartmental equilibrium is achieved could be misinterpreted as supratherapeutic from a pharmacokinetic perspective, and tolerable from a pharmacodynamic perspective. The number of compartments necessary to best fit the serum concentrationtime data can be settled statistically, after visual inspection. Body composition plays a large role in the differences in volume of distribution among patients [33]. During pregnancy, the plasma volume increases 20% by mid-gestation and 50% at term. The extracellular and total body volume increases 5080% in concert with the development of the conceptus and the enlargement of the uterus and breasts [2]. This will result in increased volume of distribution relative to body weight of more water soluble drugs. Additionally, blood volume increases to a lesser degree in pregnancy-induced hypertension and preeclampsia and may provide values for volume of distribution and peak plasma concentrations of antihypertensive agents that are closer to nongravid patient values [35]. With increases in fat mass, the potential for longer activity of drugs with greater fat solubility in the pregnant patients exists for sedative agents such as diazepam and thiopental. Plasma protein binding Alterations in drug disposition may result from changes in plasma protein binding during the course of pregnancy, labor, delivery, and the puerperium [2]. Protein binding variability may occur secondary to changes in the concentration of specific proteins and the available number of binding sites that bind drugs (binding capacity), as well as changes in the ability of these proteins to bind drugs (binding affinity) [36,37]. Variations in the protein binding of drugs are significant for the impact that it makes on both the pharmacokinetics and pharmacodynamics, the latter reflecting that the unbound drug is the active moiety that binds to receptors. Generally, the unbound fraction of an albumin-bound drug negatively correlates with the albumin concentration. Progressive decreases in maternal serum albumin occur through each trimester of gestation, with levels falling to as low as 3. This is due primarily to dilution given the expanded blood and extracellular fluid volume. Hypoalbuminemia will lower the plasma binding of mainly acidic drugs, with the most clinically important changes occurring for drugs that are typically highly bound (90%). This is observed with the antiepileptic drug phenytoin, where the unbound fraction increases by 40% from baseline to thirdtrimester [42]. High urea nitrogen concentration and diabetes can, respectively, carbamylate and glycate the albumin molecule, altering the conformation of the binding sites and resulting in reduced binding affinity [43,44]. Therefore, uremic renal failure, where increases in blood urea nitrogen are coupled with hypoalbuminemia, can diminish albumin binding of drugs such as warfarin and salicylates. Similar results may occur with uncontrolled diabetes and proteinuria, where glycation combines with hypoalbuminemia to increase the free fraction of acidic drugs [45]. Such binding displacement during pregnancy may not only make more drugs available for pharmacodynamic effect in the mother but also for delivery to the fetal compartment, subjecting the unborn to more potential risk. This may be magnified by the increased albumin concentration in the fetus with gestation (opposite to the maternal pattern) [36,47], thus allowing for greater binding in the fetal compartment and increasing the fetal:maternal concentration ratio of highly bound drugs with gestation [48]. Therefore, under these various drug-albumin protein binding altering circumstances, the free fraction of the drug is expected to increase, and the free concentration level will increase for any given total concentration. This 44 000 molecular weight protein is synthesized by the liver, is an acute-phase reactant (rising with acute myocardial infarction, trauma, cancer, sickle cell crisis, renal disease, etc. Others include tricyclic antidepressants, carbamazepine, meperidine, methadone, and fentanyl. This reduces the free plasma level of the drug available for antiarrhythmic effect in acute medical situations, and may require transient dose adjustments to provide therapeutic benefit. Unlike most drugs where the free fraction is independent of the total level in the plasma, lidocaine and disopyramide exhibit concentration-dependent protein binding, with the free fraction ranging several-fold within the respective therapeutic total concentration range. This has been demonstrated in a well-designed study of maternal disopyramide binding in each trimester and postpartum [54] as well as the need for higher doses of remifentanil to immobilize the fetus for surgical intervention [55]. Competitive binding interactions can occur between basic drugs for sites on this protein. Moreover, basic drugs that are transmitted to the fetus will have progressively higher binding and a lower free fraction, and this may cause accumulation of drug within the fetal compartment, and sustain pharmacodynamic effects in the newborn after delivery for drugs given during labor. The volume of distribution is also greatly influenced by the degree of plasma protein binding of the drug, as under conditions of normal vascular integrity, it is only the unbound drug that can leave the intravascular space to interact with receptor and nonreceptor binding sites. Drugs for which fuP fuT will not be restricted to the plasma space and the volume of distribution may be greater than total body water (>0. However, in situations where the protein binding in the serum is higher than that in the tissue, or fuP fuT, the volume of distribution will be restricted and approach 0. This equation is also useful in demonstrating the reduced volume of distribution of digoxin observed in patients with renal failure, heart failure, or hypothyroidism, and its interaction with quinidine, where diminished tissue binding is suggested [32]. Finally, maternal lipoproteins, which increase during gestation, bind a limited number of drugs, including cyclosporine, which could impact cellular uptake [59], and its anti-rejection performance and toxicity in transplant patients and require careful therapeutic drug monitoring. Red blood cell binding occurs for a number of lipid soluble drugs, including chlorthalidone and acetazolamide, potentially altering the diuretic intensity of these agents [60]. Clearance concepts the clearance of a drug is defined as the volume of blood completely purged of drug per unit time. The total body clearance of a drug combines all the available routes of elimination including hepatic, renal, lung, skin, intestinal, etc. The calculated clearance can then be normalized to rates per unit time in minutes, hours, or per day. Compartmental analysis allows fitting of the serum concentration time data to a specified model, and clearance is derived. This may require increasing the dose, and potentially lengthening the dosage interval, if peak and trough levels are critical to control. Cardiac output increases 4050% and renal plasma flow increases 2550% by the second trimester [2,61] and by 75% near term [62]. Overall, these changes speed the clearance of renally eliminated drugs during gestation and in the puerperium and is correlated with the measured increases in inulin and creatinine clearance. This applies to water-soluble drugs and metabolites that are mainly excreted unchanged. Digoxin, atenolol, clonidine, and enoxaparin are cardiovascular drugs that demonstrate increased renal clearance during pregnancy [2]. These levels would be considered in the therapeutic for preventing eclamptic seizures, where a variety of pharmacokinetically assessed dosage regimens are suggested [65]. Therefore, the changing elements during pregnancy of decreased protein binding, and increased glomerular filtration and renal blood flow contribute to the increase in renal drug clearance. Along with flow dependence and ionization, tubular secretion of substrate drugs is modulated by the expression of the major efflux transporter, P-gp, which is upregulated in the kidney during pregnancy [2]. Located on the luminal side or apical membrane of the renal tubular cell, P-gp enhances secretion over reabsorption for its drug and chemical substrates during pregnancy. As an example, digoxin renal clearance was demonstrated to correlate with creatinine clearance in a cohort of pregnant women studied at 2832 weeks gestation and again to 10 weeks postpartum [66]. Similarly, the mean tubular clearance of digoxin during gestation was nearly double that of the postpartum values (mean = 0. Greater impact on renal secretory clearance is seen with classic potent P-gp inhibitors such as verapamil, resulting in raised digoxin levels and potential concentrationrelated toxicities [20]. Carvedilol shows a similar extent of effect on digoxin renal clearance as verapamil. Combining the more rapid clearance and the larger distribution volume of numerous renally cleared agents in pregnancy may require larger dosage regimen adjustments. However, as in all other patients, care must be taken in adjusting the dosage regimen in the pregnant patient who has any degree of renal insufficiency that limits clearance and create adverse accumulation of the drug. Therapeutic drug monitoring and clinical pharmacologic endpoint evaluation may assure that if larger maternal doses are needed during pregnancy, safety to the mother and the fetus can be maintained while efficacy is promoted [10]. Hepatic clearance and drug metabolism As an organ responsible for detoxification and synthesis, both of these features are utilized in Phase 1 and Phase 2 drug metabolism reactions and conjugation involving xenobiotics. Routes to hepatic elimination of drugs include biliary elimination of changed or unchanged drug, and hepatic microsomal metabolic conversion to active or inactive metabolites, which are either further metabolized, or cleared renally. It has been debated as to whether hepatic blood flow increases with gestation, and affecting hepatic clearance of some drugs. Increases in liver blood flow result in higher hepatic clearance for systemically administered drugs that have a high extraction ratio (see below), and the increased first-pass metabolism and decreased bioavailability when these drugs are given orally (hence the 10-fold difference in oral and intravenous doses of propranolol). Comparative decreases in hepatic flow occur during labor when a number of cardiac and anesthetic agents may be initiated, and the clearance of those may be substantially different that seen earlier in the third trimester or in the nonpregnant counterpart. This, along with the changes in hemodynamics during labor and delivery may alter the pharmacologic effect of drugs during this more precarious time.
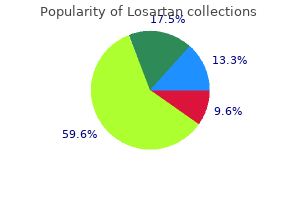
The authors concluded that while the rate of reactions appeared to decrease over time for most subjects diabetic diet sheet order generic losartan from india, reactions were common and largely unpredictable diabetic ketoacidosis in type 2 diabetes mellitus--pathophysiology and clinical presentation order discount losartan online, with several systemic reactions occurring at previously tolerated doses diabetes mellitus eye complications cheap 50 mg losartan otc, often with exercise or a viral illness diabetes signs and symptoms nhs 25 mg losartan buy with amex. This was highlighted in a study by Keet illustrating that some subjects begin to lose protection within 1 week of discontinuing treatment [11] diabetic vasculopathy losartan 50 mg on line. In this study, 35 years after completing treatment, only 19% of subjects were consuming milk in an unrestricted fashion, 31% were consuming at least one serving/ day but still were restricted, 28% consumed some uncooked milk but less than a serving/day, 6% had minimal milk or milk in a baked food only, and 16% were strictly avoiding milk. Twentytwo percent limited their consumption because of symptoms, and an additional 25% limited milk while exercising and 6% limited milk with an illness. Notably, some subjects who initially did well subsequently had increased symptoms that led to resumption of a strict milk avoidance diet. Several experienced repeated episodes of anaphylaxis after periods of apparent tolerance. This study found that 95% of children experienced at least one dose-related reaction; 91% of reactions affected a single organ; 14 children (17. Twelve percent of reactions occurred in the setting of cofactors, such as exercise, infection, emotional stress, asthma exacerbation, fasting, lying down, and tiredness. However, the omalizumab group had significantly fewer 526 Recognition, prevention, and treatment of adverse effects associated with oral allergen immunotherapy doses with symptoms (2. While these reactions can occur in an unpredictable fashion and are not all preventable, some may be preventable by taking care to always exercise extreme caution in dose administration, especially during dose escalation. Three studies used avoidance diet as a control, and one study used a placebo group. An open label long-term follow-up period of this cohort showed a benefit of longer therapy with 20/40 (50%) achieving sustaining unresponsiveness by year 4 [43]. Reports of adverse events in this important study reveal that no severe reactions were reported but that mild oropharyngeal symptoms were common, particularly during the first 10 months of escalating dosing (Table 36. One additional child in the oral immunotherapy group withdrew secondary to an allergic reaction associated with dosing after the oral food challenge at 10 months but before the challenge at 22 months. In these 22 subjects, the median percentage of doses per subject with any symptoms decreased after year 2 compared to before year 2 (0. Adverse events were reported in three subjects during the desensitization period, and one of these subjects discontinued. Similar findings are reported in several other studies, although most are just observational in nature [4557]. Adverse reactions were categorized as those occurring during the initial escalation day, the buildup phase, and the home dosing phase. Twenty of 28 patients between the ages of one and 16 years, who completed all phases of the study, were included. This study used a maintenance dose of just 300 mg of peanut protein, far lower than the 10002000 mg doses used in many subsequent studies. The probability of having any symptoms after a buildup phase dose was 46%, with a risk of 29% for upper respiratory and 24% for cutaneous symptoms. The authors conclude that subjects were more likely to have significant allergic symptoms during the initial escalation day when they were under close supervision rather than during other phases of the study and that allergic reactions with home doses are rare. These include (1) concurrent illness, (2) suboptimally controlled asthma, (3) timing of dose administration after food ingestion (fewer reactions when doses taken with food), (4) physical activity following dosing, and (5) dosing during menses. In the intent to treat analysis, 29 of 37 (78%) had sustained unresponsiveness 4 weeks after stopping treatment (300 mg arm: 17/20 [85%]; 3000 mg arm: 12/17 [71%]). Treatment was required in 25% of events, with most requiring only antihistamines and only one reaction requiring epinephrine. One subject had anaphylaxis requiring epinephrine at home that occurred while playing basketball 16 hours after the dose. In the intervention arm, 47% (n = 9) of subjects experienced clinically relevant adverse reactions during the initial-day escalation (none in the placebo arm), and clinically relevant symptoms occurred during the buildup phase after 1. None of the placebo subjects required treatment during initialday escalation or buildup dosing. The most common treatment was antihistamines, but 18 events required epinephrine administration (all occurred at home). They report that she did not have any adverse reaction during either stage of the desensitization. Two months later, he developed cough, wheezing, breathing difficulty, and hives while playing soccer after eating wheat. He was advised to avoid exercise after eating wheat-containing foods; however, he had a similar reaction while running around at home after eating wheat bread for breakfast. He was again advised to avoid eating wheat prior to exercise, and no further episodes were reported. One patient had a reaction during maintenance, which was felt to be related to exercise and was treated with antihistamines and corticosteroids. The study had four phases: rush (5 days in the hospital), long-term buildup, maintenance, and 2 weeks of complete avoidance. Buildup occurred over 4 months with a goal maintenance dose of 2000 mg of wheat protein. Subjects continued their wheat dose for 3 months (maintenance phase 1) and were then advised to eat wheat daily with no restrictions (maintenance phase 2). Of the 100 patients enrolled, 43% of subjects discontinued therapy at some point during the study. The proportion of participants with symptoms was similar during all three phases of the study (buildup: 70% [43% were moderate or severe], maintenance phase 1: 78% [35% were moderate or severe], maintenance phase 2: 72% [24% were moderate or severe]). Omalizumab was then continued for an additional 8 weeks following initial dose escalation. Subjects reached maintenance dose of 4000 mg protein per allergen at median of 18 weeks. There was one severe reaction that required epinephrine (during home maintenance dosing). Forty-eight patients were enrolled, 36 were randomized to omalizumab and 12 received placebo for 16 weeks. Similarly, maintenance was reached as early as 12 weeks in the omalizumab group and 20 weeks in the placebo group. This fact does provide considerable optimism about its potential role for its routine use in clinical practice in the future. However, given the profile of adverse events outlined in this chapter, it is clear that the picture is not universally positive. Adverse events are common, sometimes severe, and certainly occur with greater frequency than in patients who simply follow a strict avoidance diet. No specific biomarkers-for example, baseline challenge results, specific IgE or IgG4 levels, or skin test size-can accurately predict adverse events or response to therapy. These patients may be at greatest risk in that they have a false sense of security about future reactions. All investigators remain hopeful that adverse events can be significantly reduced in the future with newer techniques and the coadministration of immunomodulators, such as anti-IgE. In the end, a balance between risk/benefit will become clearer, primarily based on long-term outcomes. If long-term tolerance is achievable in a large number of patients, some adverse events may be justifiable. However, if reactions continue to occur after years of therapy, and the transient nature of the desensitization makes lifetime treatment necessary, the balance between risk/ benefit becomes far less clear. Allergen immunotherapy for IgE-mediated food allergy: A systematic review and metaanalysis. Oral tolerance, food allergy, and immunotherapy: Implications for future treatment. Sublingual immunotherapy for peanut allergy: Clinical and immunologic evidence of desensitization. Sublingual immunotherapy for peanut allergy: A randomized, double-blind, placebo-controlled multicenter trial. A pilot study of omalizumab to facilitate rapid oral desensitization in high-risk peanut-allergic patients. Possible recurrence of symptoms after discontinuation of omalizumab in anti-IgE-assisted desensitization to egg. Martorell Calatayud C, Muriel Garcia A, Martorell Aragones A, De La Hoz Caballer B. Specific oral tolerance induction in food allergy in children: Efficacy and clinical patterns of reaction. Safety and predictors of adverse events during oral immunotherapy for milk allergy: Severity of reaction at oral challenge, specific IgE and prick test. Primary eosinophilic gastrointestinal disorders in children who have received food oral immunotherapy. Garcia Rodriguez R, Mendez Diaz Y, Moreno Lozano L, Extremera Ortega A, Gomez Torrijos E. Eosinophilic esophagitis after egg oral immunotherapy in an adult with egg-allergy and egg-bird syndrome. Early oral immunotherapy in peanut-allergic preschool children is safe and highly effective. Long-term treatment with egg oral immunotherapy enhances sustained unresponsiveness that persists after cessation of therapy. Oral immunotherapy for egg allergy: A double-blind placebo-controlled study, with postdesensitization follow-up. Individualized IgE-based dosing of egg oral immunotherapy and the development of tolerance. Low-dose oral immunotherapy using low-egg-allergen cookies for severe egg-allergic children reduces allergy severity and affects allergen-specific antibodies in serum. Specific oral tolerance induction in paediatric patients with persistent egg allergy. Food allergy in children: Results of a standardized protocol for oral desensitization. Oral desensitization in children with milk and egg allergies obtains recovery in a significant proportion of cases. Efficacy and safety of high-dose peanut oral immunotherapy with factors predicting outcome. Oral immunotherapy for the treatment of peanut allergy: systematic review of six case series studies. Novel baseline predictors of adverse events during oral immunotherapy in children with peanut allergy. A case of wheatdependent exercise-induced anaphylaxis after specific oral immunotherapy. Oral immunotherapy in children with IgE-mediated wheat allergy: Outcome and molecular changes. Wheat oral immunotherapy was moderately successful but was associated with very frequent adverse events in children aged 618 years. Safety and feasibility of oral immunotherapy to multiple allergens for food allergy. Patel University of South Florida Morsani College of Medicine Linda Cox Nova Southeastern University Richard F. The immunotherapy and allergy skin test forms also should be sufficiently detailed to enable all physicians to make treatment decisions. The purpose of these guidelines is to optimize the practice of clinical allergy through objective, scientific, and reproducible documentation and standardization of skin testing and immunotherapy procedures. The intended outcome is enhanced safety, accuracy, and efficacy of allergy diagnostic testing and allergy immunotherapy treatment. Physicians may use these forms as a template and customize them for their practice, while maintaining the basic information recommended in the published guidelines. Utilization of these forms will encourage uniformity of allergy skin testing and immunotherapy procedures and improve the safety and accuracy of allergy care. This will help facilitate continuity of patient care if there is a transfer or change that could potentially affect allergy services, such as a move to a new location, a new physician, or new nursing staff. The goal of both guidelines is to improve the quality of allergy skin testing and reduce undesirable variation by documenting the results in an objective, scientific, and reproducible manner. The completed allergy skin test form should provide enough information to allow other physicians to understand the type of test and the manner in which it was performed. These variables can influence the interpretation of the allergy skin test results. Therefore, it is important to include details about these variables on the allergy skin test form. The key purpose of the allergy skin test report is to convey information about the test results. The two most commonly used methods of reporting allergy skin test results are as follows: Quantitative results are reported as measurement of the longest diameter of wheal and diameter of erythema/flare or the longest diameter and the widest perpendicular diameter (orthogonal) in millimeters. The mean wheal diameter and actual area can be calculated from these measurements. The latter are not generally used in clinical practice, primarily because the calculation requires more time than simply recording a measurement. The key to scoring must be included and must be based on measurement of wheal and flare. One of the limitations of the semiquantitative scoring method is that it fails to provide specific information about the degree of skin test reactivity. Reporting the skin test response in millimeters of the longest diameters of the wheal and erythema/ flare may provide more specific information. The longest diameter of the skin test response correlated with the actual area in a study that compared computer-determined areas of 50 skin test responses with measured skin test responses [14]. The sums and products of orthogonal diameters also highly correlated with the actual areas but added little to the correlation of the longest diameter. This study also compared area and longest diameter measurements of prick skin test responses applied by different persons and found significant differences in the area measurements between testers, which were not found when longest diameter measurements were compared.
A special note Turner syndrome Turner syndrome results from complete or partial loss of the X chromosome with a prevalence of approximately 0 diabetes insipidus complications buy discount losartan. Turner syndrome is the most common cause of premature ovarian failure; thus diabetes y sexualidad buy losartan mastercard, conception and pregnancy can be challenging and may require enhanced reproductive techniques blood glucose daily log sheet buy losartan pills in toronto. Consequently diabetes testing supplies commercial cheap losartan line, Turner patients often undergo preconception counseling which is an ideal time to assess the potential risk to the aorta during pregnancy diabetes in dogs how to inject losartan 25 mg buy without a prescription. Pregnant Turner patients with a normal sized aorta and without any of the aforementioned risk factors should have aortic imaging assessment at least once during pregnancy, generally around 20 weeks gestation [73]. If aortic dilatation or any risk factors for dissection are present, then aortic imaging assessment is recommended every one to two months [73]. The exact prevalence of the disease is unknown, but it is estimated to afflict roughly 1500 individuals in the United States [74]. These serious complications are typically a result of an arterial, uterine, or intestinal rupture [74]. Given the extreme fragility of the connective tissue and the vasculature, surgical intervention is discouraged in this patient population unless life-threatening circumstances arise [61,77]. Given that surgery is discouraged for all but the most concerning vascular finding [61,77,78], there is debate as to whether or not these patients should undergo routine imaging. Some experts have argued against pursuing imaging since intervention is discouraged and results will only increase patient anxiety [79]. Causes of death included three aortic ruptures (two of which occurred at term delivery and the third one week after an uncomplicated cesarean section), iliac artery rupture following a mechanical fall at 33 weeks gestation and wound dehiscence after a cesarean section at 36 weeks gestation. With the exception of third- and fourth-degree lacerations occurring during vaginal delivery, too few events occurred in this study population to allow for assessment of which mode of delivery resulted in the fewest complications. Many experts either discourage pregnancy [81] or suggest that it is contraindicated [77]. Despite the lack of imaging guidelines, it would be reasonable to consider a comprehensive imaging assessment of the entire arterial vasculature prior to or in the early stages of pregnancy in an effort to try and foresee any issues that might develop during the pregnancy and formulate potential plans for intervention. Findings from this initial assessment could guide further surveillance throughout the pregnancy and early postpartum period. During the actual delivery process, caution should be taken with use of retractors so as to avoid damage to adjacent bowel and soft arterial clamps are recommended [61]. Furthermore, care should be utilized to avoid damage to the arterial wall during suture placement [79]. As with the other aortopathies, close follow-up is warranted in the postpartum period. Aortic dissection has been documented to occur in patients as young as 3 months [89,90] and mean age of death in the initial series was 26. General adult guidelines suggest intervening on the aortic root, ascending aorta, and aortic arch if the dimension is >4. Postoperatively continuing clinical follow-up and imaging surveillance is warranted given the risk for aortic aneurysm formation both proximal and distal to grafts as well as coronary artery button aneurysm formation that can occasionally progress enough to warrant surgical repair [96]. The available literature has reported 217 pregnancies occurring in 85 patients [97]. Of these pregnancies, there were 3 (1%) maternal deaths and 15 (7%) severe complications including aortic and vertebral artery dissection, uterine rupture, and postpartum hemorrhage. Of the three mortalities, one was attributed to a type A aortic dissection that occurred three weeks postpartum, the second was due to subarachnoid hemorrhage resulting from bilateral vertebral artery dissection occurring in the postpartum period, and the third death occurred suddenly immediately after delivery with an unknown diagnosis. Recommendations for management As with the other aortopathies, management of the patient should begin prior to conception and involve a team of subspecialty experts. The patient should also be made aware that prior surgical repair of an aortic aneurysm does not preclude aortic complications from developing during pregnancy or during the postpartum period [98,99]. Prenatal diagnosis to confirm the presence of a causative mutation can be performed preimplantation or via amniocentesis of chorionic villus sampling [91]. Prior to conception, the entire vascular system from head to pelvis should be assessed. Some experts have advocated for early delivery via cesarean section so as to avoid increased intra-abdominal pressure [91], whereas others note the risk of increased intra-abdominal pressure could be mitigated with instrumental assistance (forceps or vacuum) during the second stage of labor [97]. In such an instance, manual techniques to attain hemostasis should be considered instead of the use of ergometrine or prostaglandin analogues due to the risk of developing hypertension and the resultant hemodynamic stress on the vasculature. Regardless of the type of mutation, the resultant histopathological changes of the aorta are similar including reticulin fragmentation, loss of elastin, and mucopolysaccharide deposition [28,32,46]. Specifically, this study of 52 women and a total of 137 pregnancies reported eight (6%) aortic dissections with half of these occurring during the third trimester and the other half occurring within the first two weeks after delivery [105]. Six of the eight dissections involved the ascending thoracic aorta, three of these caused maternal mortality. Importantly, half of the patients with ascending thoracic aortic dissections dissected at an aortic caliber less than 5. Emergent cesarean section was performed with concomitant ascending thoracic aorta replacement with aortic valve resuspension and aortic arch reconstruction. The descending thoracic and abdominal aortic dissection was managed conservatively. It is therefore imperative that a comprehensive medical history of any patient contemplating pregnancy includes questions regarding a family history of aortic aneurysm/dissections. Acute aortic syndromes during pregnancy the risk of acute aortic syndromes, defined as aortic dissection, intramural hematoma, or symptomatic penetrating atherosclerotic ulcer, during pregnancy is increased in the patient with an underlying aortopathy. Details regarding presentation, diagnosis, and treatment for acute aortic syndromes are beyond the scope of the current discussion, and instead, this section focuses on pearls for management of the pregnant patient. In general, when the pregnant patient with an acute aortic syndrome presents, pharmacologic therapy should be initiated promptly to reduce the double-product and then the patient should be transferred emergently to a tertiary referral center to allow multidisciplinary care and urgent or emergent intervention if needed [44]. Continuous fetal heart rate monitoring is essential in order to detect heart rate decelerations which are suggestive of fetal malperfusion and/or hypoxemia [106]. Stanford type B aortic dissections, those commencing distal to the left subclavian artery, are generally managed medically as long as the patient is stable without organ compromise and fetal perfusion is maintained. Unfortunately, the use of cardiopulmonary bypass during pregnancy carries up to a 5% maternal and a 30% fetal mortality rate [109]. Fetal viability is generally accepted to be around 24 weeks, so if a type A dissection occurs prior to this time, the fetus should remain in utero [110]. However, after this period, particularly once 30 weeks gestation has been reached, a cesarean section with concomitant aortic repair is recommended in the pregnant patient with a type A aortic dissection [44]. If cardiac surgery is required during pregnancy, the use of normothermic, high pressure, high flow cardiopulmonary bypass should be used when possible in order to reduce the risk of fetal hypoxia and vasoconstriction [110]. Our understanding of the various aortopathies continues to evolve, and we expect these advancements to further refine our approach to the pregnant patient with aortopathy. However, we anticipate that the fundamental approach of careful clinical evaluation, multidisciplinary care, and rigorous follow-up will continue to be essential in caring for these complex patients. Subcommittee on Reporting Standards for Arterial Aneurysms, Ad Hoc Committee on Reporting Standards, Society for Vascular Surgery and North American Chapter, International Society for Cardiovascular Surgery. Regression equations for calculation of Z scores of cardiac structures in a large cohort of healthy infants, children, and adolescents: an echocardiographic study. Normal limits in relation to age, body size and gender of two-dimensional echocardiographic aortic root dimensions in persons 15 years of age. Giant cell arteritis presenting with aortic aneurysm, normal erythrocyte sedimentation rate, and normal C-reactive protein. Measurement of aortic diameters and detection of asymptomatic aortic aneurysms in a mass screening program using a mobile helical computed tomography unit. Body-surface adjusted aortic reference diameters for improved identification of patients with thoracic aortic aneurysms: results from the populationbased Heinz Nixdorf Recall study. Thoracic aortic aneurysm and dissection: increasing prevalence and improved outcomes reported in a nationwide population-based study of more than 14,000 cases from 1987 to 2002. Ascending aortic dilatation associated with bicuspid aortic valve: pathophysiology, molecular biology, and clinical implications. Cell lineages and tissue boundaries in cardiac arterial and venous poles: developmental patterns, animal models, and implications for congenital vascular diseases. Aortic dilatation patterns and rates in adults with bicuspid aortic valves: a comparative study with Marfan syndrome and degenerative aortopathy. Pattern of ascending aortic dimensions predicts the growth rate of the aorta in patients with bicuspid aortic valve. Vascular matrix remodeling in patients with bicuspid aortic valve malformations: implications for aortic dilatation. Structural abnormalities of great arterial walls in congenital heart disease: light and electron microscopic analyses. Bicuspid aortic valves are associated with aortic dilatation out of proportion to coexistent valvular lesions. Features and predictors of ascending aortic dilatation in association with a congenital bicuspid aortic valve. Natural history of ascending aortic aneurysms in the setting of an unreplaced bicuspid aortic valve. Effect of aortic aneurysm replacement on outcomes after bicuspid aortic valve surgery: validation of contemporary guidelines. Frequency of cardiovascular events in women with a congenitally bicuspid aortic valve in a single community and effect of pregnancy on events. Outcome of pregnancy in patients with bicuspid aortic valve a study of 89 patients. Developed in Collaboration With the American Society of Echocardiography, Heart Rhythm Society, International Society for Adult Congenital Heart Disease, Society for Cardiovascular Angiography and Interventions, and Society of Thoracic Surgeons. Long-term risk for aortic complications after aortic valve replacement in patients with bicuspid aortic valve versus Marfan syndrome. Further delineation of aortic dilation, dissection, and rupture in patients with Turner syndrome. Aortopathies in adult congenital heart disease and genetic aortopathy syndromes: management strategies and indications for surgery. Repaired coarctation: a "cost-effective" approach to identify complications in adults. Recurrence risks in offspring of adults with major heart defects: results from first cohort of British collaborative study. Clinical practice guidelines for the care of girls and women with Turner syndrome: proceedings from the 2016 Cincinnati International Turner Syndrome Meeting. Effect of celiprolol on prevention of cardiovascular events in vascular EhlersDanlos syndrome: a prospective randomised, open, blinded-endpoints trial. Pregnancy-related deaths and complications in women with vascular EhlersDanlos syndrome. Early surgical experience with LoeysDietz: a new syndrome of aggressive thoracic aortic aneurysm disease. Clinical utility gene card for: hereditary thoracic aortic aneurysm and dissection including next-generation sequencing-based approaches. Importance of the clinical recognition of LoeysDietz syndrome in the neonatal period. Recent advances in understanding Marfan syndrome: should we now treat surgical patients with losartan Valve-sparing aortic root reconstruction in children, teenagers, and young adults. Pregnancy after aortic root replacement in LoeysDietz syndrome: high risk of aortic dissection. Reduced penetrance and variable expressivity of familial thoracic aortic aneurysms/ dissections. The disease is most common in Asian countries, with increasing reports in Europe, Africa, the Middle East, and North America. In Japan, the annual incidence is about 150 cases/yr, whereas in the United States, the overall annual incidence is estimated at 13 cases/yr [1]. The disease affects mostly women in their childbearing years with reports ranging ratios from 49: 1 female to male predominance [2,6,7]. The median age of diagnosis has been 26 years old, but varies slightly based on ethnicity [810]. Clinical features Clinical presentation has been described as two or three phases [11]. The early stage is an inflammatory period with granulomatous arteritis of the aorta and its branches. The symptoms in this phase can be subtle or overt and include fever, malaise, weight loss, night sweats, polyarthralgia, or arthritis. Subsequent phases include vascular inflammation that results in vessel tenderness or pain. Arteritic changes including intimal proliferation, degeneration of medial elastic fibers, and vasa vasorum compromise lead to narrowing that can result in occlusion. These changes can also cause aneurysm formation with possible risk of dissection [1]. There maybe arterial collaterals that form due to chronicity of occlusions, and this can result in insidious onset of symptoms, and often may appear "asymptomatic. One study described juveniles had a delay in diagnosis four times that of adults [9]. In addition to being aware of these symptoms, it is critical to understand, that asymptomatic disease progression is not uncommon. Patients often present with new onset hypertension, asymmetric blood pressure readings, or vascular bruits. One should take care to do a thorough vascular exam, as well as palpate the carotids for tenderness. It has been noted that physical exam has great specificity (7198%), but poor sensitivity (1450%) for diagnosis [12]. Secondary complications include renovascular hypertension, aortic regurgitation, abdominal or myocardial ischemia, heart failure, cerebrovascular accidents, and pulmonary hypertension.
Buy generic losartan 25 mg online. 3 in 10 people with diabetes don't know they have it.
References
- Juel C, Bangsbo J, Graham T, et al. Lactate and potassium fluxes from human skeletal muscle during and after intense, dynamic, knee extensor exercise. Acta Physiol Scand. 1990;140(2):147- 159.
- DiFurio MJ, Auerbach A, Kaplan KJ. Well-differentiated fetal adenocarcinoma: rare tumor in the pediatric population. Pediatr Dev Pathol 2003;6:564-7.
- Wells DL, Allen JM. Ventriculoperitoneal shunt infections in adult patients. AACN Adv Crit Care. 2013;24:6-12; quiz 13-14.
- Bartuli A, Landolfo A, Pirozzi N, et al. Severe chylomicronemia syndrome (CHS) with neonatal onset successful treatment of cardiac failure with plasmapharesis. J Inherit Metab Dis 2002;25(Suppl 1):161.
- Hug EB, Loredo LN, Slater JD, et al. Proton radiation therapy for chordomas and chondrosarcomas of the skull base. J Neurosurg 1999;91(3):432-439.
- Coleman, A.J., Choi, M.J., Saunders, J.E., Leighton, T.G. Acoustic emission and sonoluminescence due to cavitation at the beam focus of an electrohydraulic shock wave lithotripter. Ultrasound Med Biol 1992;18:267-281.
- Seegulam ME, Ratner L. Integrase inhibitors effective against human T-cell leukemia virus type 1.