- info@careermakers.edu.np
- +977 1 4423870
Sotalol
Koray Arica, MD
- Clinical Assistant Professor
- Department of Anesthesiology
- SUNY Downstate Medical Center
- Brooklyn, New York
Oval window Cochlea: this snail-like structure contains the structures for hearing blood pressure for infants safe 40 mg sotalol. The middle compartment is a triangular duct (called the cochlear duct) filled with endolymph; the outer two compartments are filled with perilymph blood pressure medication new zealand cheap sotalol 40 mg free shipping. Cochlear duct (with endolymph) Perilymph Resting on the floor (called the basilar membrane) of this duct is the organ of Corti blood pressure chart for 14 year old sotalol 40 mg buy line, the hearing sense organ arrhythmia treatment algorithm 40 mg sotalol purchase otc. What we can hear depends on how loud a sound is (the volume) as well as its pitch hypertension patho discount sotalol 40 mg with visa. Human ears can respond to sounds having a pitch between 20 Hz (vibrations per second) and 16,000 Hz. For example, cats can hear sounds up to 60,000 Hz, and bats can detect frequencies as high as 120,000 Hz. Hairs Tectorial membrane the organ of Corti consists of a layer of epithelium (composed of sensory and supporting cells). Thousands of hair cells project from this epithelial layer and are topped with a gelatin-like membrane called the tectorial membrane. Movement here stimulates the hairs of the organ of Corti to send nerve impulses along the cochlear nerve. Anything that interferes with the transmission of vibrations to the inner ear will result in a hearing loss. For example, fluid in the middle ear (as a result of an infection, cold, or allergies), impacted cerumen, or a foreign body will all block the transmission of vibrations. A more serious type of conductive hearing loss is otosclerosis, a condition in which the auditory ossicles fuse together. This type of hearing loss most often results from the death of hair cells in the organ of Corti, usually a result of frequent exposure to sustained loud noise (such as that experienced by factory workers and musicians). Once the hairs are damaged, they never grow back, making this type of hearing loss permanent. This arrangement allows each canal to be stimulated by a different movement of the head. Within each ampulla is a mound of hair cells topped by a gelatinous cone-shaped cap called the cupula. The lightweight cupula floats in the endolymph that fills the semicircular canals. Cupula Hair cells Utricle Inside the vestibule are two sense organs: the utricle and saccule. The tips of the hair cells are covered by a gelatin-like material; embedded throughout the gelatin material are heavy mineral crystals called otoliths. The semicircular canals are primarily concerned with the speed and direction of head movements (dynamic equilibrium). In contrast, the utricle and saccule share responsibility for detecting the position of the head when the body is stationary and also for the sense of acceleration when moving in a straight line (such as when riding in a car). Gravitational force When the head rotates, the endolymph inside the ampulla lags behind. When the movement stops, the endolymph swirls past the cupula, bending it in the process. This pulls on the hair cells, stimulating nearby nerve receptors to send a signal to the brain via the vestibular nerve. The brain interprets the information and triggers the responses necessary for maintaining balance when the head or body is suddenly moved. Inside the vestibule, the otoliths remain level on the hair cells when the head is level, causing minimal stimulation. When the head tilts (or when the entire body moves forward), the membrane and the otoliths shift, stimulating the hair cells. Accessory Structures of the Eye Eyebrow: Perhaps the most significant role of eyebrows is to enhance facial expressions, aiding in nonverbal communication. Eyelids (palpebrae): Formed primarily by the orbicularis oculi muscle covered with skin, the upper and lower eyelids protect the eye from foreign bodies and block light when closed to allow for sleeping. Lateral canthus Medial canthus Palpebral fissure: this is the opening between the lids. Lower eyelid Tarsal glands: these glands, which lie along the thickened area at the edge of the eye (called the tarsal plate), secrete oil to slow the evaporation of tears and help form a barrier seal when the eyes are closed. Eyelashes: these hairs along the edges of the eyelids help keep debris out of the eye. Conjunctiva: the conjunctiva is a transparent mucous membrane that lines the inner surface of the eyelid and covers the anterior surface of the eyeball (except for the cornea). It is very vascular, which becomes apparent when eyes are "bloodshot," a result of dilated vessels in the conjunctiva. Upper eyelid Lacrimal Apparatus the lacrimal apparatus consists of the lacrimal gland and a series of ducts (which are also called tear ducts). Lacrimal gland: this small gland secretes tears that flow onto the surface of the conjunctiva. Furthermore, tears contain a bacterial enzyme called lysozyme that helps prevent infection. Nasolacrimal duct: this passageway carries tears into the nasal cavity (which explains why crying or watery eyes can cause a runny nose). Ducts Lacrimal punctum: this tiny pore at the end of each lacrimal canal drains tears into the lacrimal canals and nasolacrimal duct. This group of muscles-called extrinsic muscles because they reside outside the eyeball-moves the eye. Intrinsic muscles, which will be discussed later in this chapter, regulate the size of the pupil and change the shape of the lens. Superior rectus Medial rectus Lateral rectus Four recti (or "straight") muscles move the eye up, down, medially, and laterally. Ultraviolet wavelengths lie just above this spectrum, while infrared wavelengths lie just below it. Some animals, though, can detect ultraviolet light, making colors visible that humans are blind to . Also, certain snakes, including rattlesnakes, have a second set of "eyes" that sense infrared radiation, allowing them to spot prey in their vicinity. It lies within the bony orbit of the skull and is partially surrounded by a layer of fat. Three layers of tissue form the surface of the eye, while the inside is divided into two fluid-filled chambers. Tissue Layers the eye is formed by three layers of tissue A fibrous outer layer (consisting of the sclera and cornea) A vascular middle layer (consisting of the choroid, ciliary body, and iris) A neural inner layer (consisting of the retina, optic nerve, and blood vessels) Fibrous Outer Layer the sclera-formed from dense connective tissue- is the outermost layer of the eye. Most of the sclera is white and opaque; it forms what is called "the white of the eye. The cornea is a transparent extension of the sclera in the anterior part of the eye. It sits over the iris (the colored portion of the eye) and admits light into the eye. Vascular Middle Layer the iris is a ring of colored muscle; it works to adjust the diameter of the pupil (the central opening of the iris) to control the amount of light entering the eye. The ciliary body is a thickened extension of the choroid that forms a collar around the lens. The choroid is a highly vascular layer of tissue that supplies oxygen and nutrients to the retina and sclera. Inside the retina are photoreceptors called rods and cones that are stimulated by light rays to produce an electrical or chemical signal. The retina can be viewed by using a hand-held instrument called an ophthalmoscope to look through the pupil to the back of the eye. The center point of the retina, as seen through an ophthalmoscope, is a patch of cells called the macula lutea. Most of the cones are concentrated here, making this the area that produces the sharpest vision. Nerve fibers leave the retina at this point, converging to become the optic nerve. Venule Arteriole 218 That Makes Sense Remember: the eye consists of three spaces: the anterior chamber, the posterior chamber, and the posterior cavity. To identify your own blind spot, draw a large dot on the left side of a 3" x 5" card and an "X" on the right. At some point, the dot will disappear as it falls on the blind spot of your left eye. Chambers and Fluids the eye is actually a fluid-filled sphere divided into two main cavities. This cavity is further divided into an anterior chamber (anterior to the iris) and a posterior chamber (posterior to the iris but anterior to the lens). The lens is a transparent disc of tissue just behind the pupil, between the anterior and posterior cavities. Anterior chamber Canal of Schlemm Posterior chamber the ciliary body secretes aqueous humor that fills the anterior cavity. The fluid flows from the posterior chamber, through the pupil, and into the anterior chamber of the anterior cavity. The posterior cavity is the larger cavity lying posterior to the lens and anterior cavity. Life lesson: Glaucoma Damage to retina and optic nerve Pressure inside eye Normally, the production of aqueous humor by the ciliary body equals the rate of absorption through the canal of Schlemm. If the canal of Schlemm becomes obstructed, aqueous humor accumulates first in the anterior chamber and then in the posterior chamber, causing pressure within the entire anterior cavity to build. Rising pressure in the anterior cavity forces the lens backward, driving the vitreous body against the choroid, which, in turn, obstructs blood flow to the retina and optic nerve. Left untreated, cells in the retina die, the optic nerve atrophies, and blindness may result. Although glaucoma can be easily diagnosed during a routine eye exam, it remains a leading cause of blindness. Later symptoms include a narrowed field of vision and colored halos around artificial lights. While glaucoma can be treated with drugs or surgery, any resulting vision loss is permanent. Light must enter the eye and focus on the retina to produce a tiny, upside-down image of the object being viewed. The photoreceptors in the retina (rods and cones) must convert that image into nerve impulses. Formation of a Retinal Image For a retinal image to form, light rays entering the eye must be bent, or refracted, so they focus on the retina. Also, if the object being viewed is near rather than far away, other eye adjustments are required. Specifically, the eyes must converge on the object being viewed, the pupils must constrict and the lens must change its curvature (accommodation). However, the curved surface of the cornea refracts most of the light entering the eye. Refraction Light rays entering the eye must be bent so they focus precisely on the retina. When light rays strike a substance at an angle other than 90°-such as when light rays strike the curved edge of the cornea-the light rays bend. Light rays that strike the center of the cornea pass straight through, while light rays that strike off-center, where the cornea is curved, are bent toward the center. Lens Retina Fovea Cornea Convergence Proper vision requires the light rays from an object to fall on the same area of each retina. Convergence lines up the visual axis of each eye toward the object so that the light rays fall on the corresponding spots on each retina. Light rays from distant objects are almost parallel, meaning the eyes require little adjustment. Therefore, the eyes must move inward, or converge, on the object to align the visual axis with the light rays. If the eyes fail to converge, light rays from the object will fall on different parts of each retina, resulting in double vision (diplopia). The lenses bend light rays before they reach the cornea so that, by the time the rays reach the back of the eye, they focus on the retina to produce clear vision. The following figures illustrate normal vision as well as common refractive errors. Emmetropia: When light rays focus on the retina without the need of a corrective lens, normal vision results. Myopia (nearsightedness): When light rays focus in front of the retina instead of directly on it, distant objects appear blurry while those up close are clear. This condition, called myopia, occurs if the eyeball is too long or the cornea has more curvature than normal. Hyperopia (farsightedness): When light rays focus at a point behind the retina, objects up close appear blurry. Called hyperopia, this condition occurs if the eyeball is too short or the cornea is flatter than normal. Astigmatism: Astigmatism results from an uneven or asymmetrical curvature of the cornea, causing light to be focused unevenly. People with astigmatism have difficulty viewing fine detail in objects up close as well as at a distance. Presbyopia: With age, the lens loses flexibility-interfering with its ability to change shape-and the focusing muscles in the eye weaken.
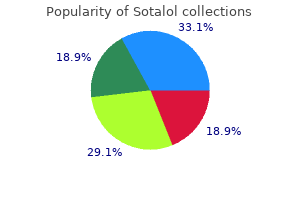
If filling is stopped and the pressure returns to baseline blood pressure ziac purchase discount sotalol, then the compliance is not impaired hypertension with bradycardia 40 mg sotalol buy free shipping. A number of "pop-off " mechanisms can make bladder compliance appear better than it actually is blood pressure checker order sotalol 40 mg with amex. Examples of this would be vesicoureteral reflux blood pressure chart in pdf cheap sotalol 40 mg line, which basically means bladder pressure is being transferred to the reflexing renal unit that blood pressure chart download excel 40 mg sotalol overnight delivery, over time will be harmful to the upper tract. Another example is a large bladder diverticulum that may provide a protective effect on the upper tract. It may only become apparent when outlet resistance is increased, which can be demonstrated during filling cystometry by occluding the urethra. During the voiding phase, the bladder neck should be open and the urethra should be relaxed and free of strictures, diverticula, or filling defects. Furthermore, it is well-known that many women can void to completion without a significant rise in detrusor pressure. Other causes included pelvic organ prolapse, external compression, urethral diverticulum, and urethral stricture. This is because of its ability not only to capture the detrusor pressure/uroflow parameters, but also to localize the level of obstruction. If the patient has no history suggestive of neurogenic bladder, the condition is termed dysfunctional voiding. Urodynamic Findings Uroflowmetry: Patient voided 118 mL in 22 sec with a postvoid residual of 40 mL. Although the voided volume was less than 150 mL, the uroflow parameters were all within the normal range. The first sensation of bladder filling occurred at a volume of 20 mL, desire to void at 61 mL, and strong desire to void at 303 mL. Because the first sensation occurred at a very low volume, impaired bladder sensation was excluded. Urodynamic stress incontinence was demonstrated at a volume of 150 mL with a cough leak point pressure of 96 cm H2O. The filling phase of the study demonstrated a stable detrusor with normal bladder compliance. There is an increase in the intraabdominal pressure, which reflects an additional Valsalva effort during voiding. Pertinent in her medical history is a motor vehicle accident with subsequent pelvic fracture that was fixed with a plate and screws. Vaginal examination revealed urethral hypermobility, an exposed piece of the polypropylene mesh in the left vaginal sulcus, no pelvic organ prolapse, negative empty supine stress test, and no vaginal atrophy. The urethra is a little distorted, probably related to the previous pelvic fracture and/or previous sling procedure. Note the minimal rise in detrusor pressure, with a good urine flow secondary to a significant Valsalva effort. In addition, neurogenic bladder, which could have resulted from pelvic nerve damage, was ruled out. During the course of her disease, she had developed urge urinary incontinence that was complicated by paraplegia and limited mobility. On examination, the patient was wheelchairbound with an otherwise normal body habitus. Pelvic examination was unremarkable; the urethra was normal and the Foley catheter was noted to be draining clear urine. Focused neurologic examination was positive for paraplegia, with what appeared to be a normal pudendal nerve sensory distribution. The patient ultimately underwent excision of the exposed sling and insertion of a synthetic retropubic sling. Bladder compliance improved toward the end of the study after the bladder had emptied. The disease affects mostly the cervical spinal cord but can also affect the brain and other spinal cord segments. The goals of treating patients with suspected neurogenic bladder are to keep the patient dry, maintain sufficient bladder emptying, and avoid neurogenic bladderrelated complications. No pressure flow study could be performed because the patient had involuntarily emptied her bladder during filling. Fluoroscopy Cystogram showed a small bladder volume, open bladder neck during filling, and leakage of contrast through the urethra. Note good flow with minimal rise in detrusor pressure and significant Valsalva effort. The patient has an indwelling Foley catheter that, when used for long periods, has known associated risks of infection, encrustation, and potential for development of bladder cancer. The indwelling urethral catheter also carries risk for urethral erosion, fistula, and worsening of leakage. A suprapubic tube could be considered as an alternative with the advantage of avoiding the urethra, but the patient may still continue to leak through the urethra. Furthermore, the suprapubic tube carries similar risks for recurrent urinary tract infection, encrustation, and bladder mucosal changes. Based on this complicated situation, different forms of urinary diversion (continent and incontinent) were discussed with the patient because this would assure tubeless drainage and hence avoid the indwelling catheterrelated complications. Because she had reasonable manual dexterity, the patient elected to proceed with a continent urinary diversion. Given the small bladder capacity and right vesicoureteral reflux, bladder augmentation was concomitantly performed. Because there were also concerns about constant urethral leakage postoperatively, an obstructive rectus fascia sling was also placed. She has a history of cervical cancer treated with hysterectomy and pelvic irradiation 22 years ago. She had been tried on different antimuscarinic medications without significant improvement. Notice the rise in detrusor pressure during filling with no concomitant rise in the abdominal pressure. On examination, the patient was moderately obese and, although she was able to walk, she frequently used a wheelchair. Discussion Urinary incontinence after pelvic irradiation can have multiple etiologies. Detrusor damage and/or urethral stricture secondary to urethral fibrosis and scarring may result in urinary retention with overflow urinary incontinence. Finally, in patients who develop extensive tissue necrosis after radiation, vesicovaginal fistula may develop, resulting in severe continuous urine leakage. Also, the Interstim lead was seen in a normal position, which excludes technical factors as an explanation for failure of neuromodulation. The patient was counseled about different options and ultimately underwent a transverse colon conduit. The transverse colon was used in this case to avoid the possibly of using irradiated small bowel. Urodynamic Findings Uroflow study: this study was not done because the patient had an indwelling Foley catheter. There was also evidence of gradually increasing detrusor pressure (although of low amplitude) with filling suggesting poor bladder compliance. Case 4: Female Urethral Stricture A 49-year-old female was referred with a diagnosis of a urethral stricture with high postvoid residual volumes and symptoms of urgency and frequency. She had received multiple urethral dilations in the past in an attempt to relieve the urethral stricture. She was eventually kept on daily self-urethral calibration, noting that she could not urinate Fluoroscopy the scout film showed the Interstim lead to be in a good position. Note also the position of the Interstim lead and the leakage per urethra on the cystogram. The diagnosis of urethral stricture had been made on urethroscopy, noting urethral bleeding when an attempt was made to advance the scope through the stricture. The patient was counseled about the need for suprapubic tube insertion as a temporary measure for her urine retention. This would allow healing of the urethra and a more precise evaluation could then be performed. Possible clues are obstructive voiding symptoms in a patient who has a history of urethral trauma, urethral infections, or urethral surgery. Oftentimes, as in this case, a cystoscope cannot pass through the stricture and therefore does not provide details about the proximal extent of the stricture. A retrograde urethrogram could be attempted but is technically difficult in females and has a low clinical yield. Evaluation of the proximal part of the urethra can be obtained with a voiding cystogram or antegrade cystoscopy by passing a scope through the suprapubic tube tract. The study confirmed that the patient has good detrusor contractility and normal bladder compliance and capacity. Because she had previously undergone multiple urethral dilations that failed to correct the stricture urethral, reconstruction using a vaginal skin flap was performed. There was no uroflow study or postvoid residual obtained because the patient had a suprapubic catheter in place. This phase of the study was normal with normal cystometric capacity, bladder sensation, and compliance. The voiding cystogram confirmed a dilated bladder neck and proximal part of the urethra with narrowing at the distal part. Voiding cystogram shows an open bladder neck, dilated proximal urethra, and narrow distal urethra. These are characteristics of bladder outlet obstruction secondary to urethral stricture. Ambulatory urodynamics have their greatest value in patients in whom conventional urodynamics are not suitable or are unable to reproduce the symptoms in question. In 2000, the International Continence Society published guidelines for the performance of ambulatory urodynamics (van Waalwijk van Doorn et al. Patients are then instructed on how to accurately record symptoms and how to identify catheter displacement and hardware failure. Most ambulatory urodynamic systems employ microtip transducer catheters that allow the most mobility. These are placed transurethrally to record bladder pressure and transrectally to record abdominal pressure. These catheters are firmly secured to the patient and connected to a portable recording device. Some systems contain a third channel that can be used for measuring urinary leakage, via an absorbent electronic nappy pad (Robertson and Neil, 1996). Practically speaking, it is most useful when standard urodynamics are inconclusive and diagnosis and treatment are uncertain. Ambulatory urodynamics have been most commonly used to diagnose the cause of urinary incontinence but also has been used in patients with outlet obstruction and neuropathic voiding dysfunction. One large study by Patravoli (2007) involved the review of 422 patients who underwent ambulatory urodynamic studies over a 12-year period. In 77% of symptomatic women with normal cystometry, ambulatory urodynamics diagnosed the cause of incontinence and provided clear and added value. What was not clear, however, was what was actually meant by clear added value and how treatment was effected. A smaller study (Pannek and Pieper 2008) noted similar findings, but a more useful interpretation of those findings was reported. Thus ambulatory studies were clinically useful in only about half the patients who underwent them. When a diagnosis was made on ambulatory studies, successful treatment was established in 42% of patients. However, when ambulatory urodynamics were not helpful and patients were treated by clinical symptoms, 33% were treated successfully. In summary, ambulatory urodynamics have not become a popular testing modality in the United States. Although they may be useful in select patients where conventional urodynamics are not diagnostic, the information obtained should affect treatment, counseling, and or follow-up. Because of a lack of easy access to this form of equipment at the present time, most centers using this are performing it on a research basis. These studies remain difficult to interpret, time-consuming, and at times technically challenging. Finally, the data obtained from ambulatory urodynamics must always be weighed against the fact that, for many findings (both normal and abnormal), standards for interpretation have not yet been established. It provides the advantages of combining anatomic and functional evaluation of complex symptoms using fluoroscopy and contrast media. Although the test provides invaluable data in certain clinical situations, the benefit of the test should be balanced against the cost, invasiveness, radiation hazards, and the involved morbidity. The standardisation of terminology of lower urinary tract function: report from the Standardisation Subcommittee of the International Continence Society. Disposable (infant) surface electrocardiogram electrodes in urodynamics: a simultaneous comparative study of electrodes. Urodynamic differences between dysfunctional voiding and primary bladder neck obstruction in women. Comparison of urodynamic findings in women with anatomical versus functional bladder outlet obstruction.
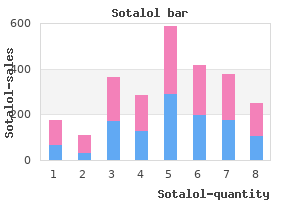
Rare petechiae are seen in normal patients arrhythmia basics generic sotalol 40 mg visa, especially on the posterior wall and trigone blood pressure norms chart 40 mg sotalol buy mastercard, caused by cystoscope trauma blood pressure medication weight loss buy generic sotalol online. In contrast blood pressure medication impotence safe 40 mg sotalol, interstitial cystitis patients have at least 10 to 20 glomerulations per field of vision blood pressure higher at night cheap sotalol 40 mg line. These ulcers appear as velvety red patches or linear cracks with a granulating base and surrounding vascular congestion. They are usually translucent with a villous appearance but can become large enough to partially fill the urethral lumen. Cystitis cystica consists of clear mucosal cysts usually found in multiple areas over the bladder base. The cysts are formed by single layers of subepithelial transitional cells, which degenerate with central liquefaction. Cystitis glandularis has a similar appearance to cystitis cystica, but the cysts are not clear, and they have a less uniform contour. In cystitis glandularis, however, there is involvement of multiple layers, including the mucus-producing glandular epithelium. Both lesions are associated with chronic irritation of the bladder mucosa and are commonly surrounded by marked inflammation. The association of cystitis glandularis with adenovillous carcinoma of the bladder has led to the belief that cystitis glandularis may be a precursor of adenocarcinoma. A proposed metaplastic transformation from epithelial hyperplasia through cystitis glandularis and finally to adenocarcinoma is based on a case presented by Shaw et al. There have been two subsequent reports of transformation of cystitis glandularis to adenocarcinoma. Transitional cell carcinoma is the most common histologic type, followed by adenocarcinoma and squamous cell carcinoma. Transitional cell carcinoma is usually induced by a carcinogen; tobacco, dyes, and organic chemicals are known carcinogens for the transitional epithelium. Cystoscopic appearance is variable, depending on histologic type and grade, but usually reveals a raised lesion with a villous feathery or papillary appearance. Superficial transitional cell carcinoma may be multicentric or may have associated carcinoma in situ. Carcinoma in situ can be disturbingly inconspicuous, often mimicking the macules or plaques of infectious cystitis. Vesical and ureteral structural variations may be anatomic or functional anomalies. Auxiliary ureteral orifices are examples of rare anatomic anomalies that are indicative of renal collecting anomalies. When present, they often enter the vesical wall slightly superior to the trigone and in near proximity to the other ureteral orifice. Ureteroceles are caused by laxity of the distal ureteral lumen, with herniation into the vesical cavity during efflux. Trabeculations are smooth ridges that become evident with distention of the bladder to volumes approaching maximum cystometric capacity. They appear as interlaced cords of different diameters with intervening sacculations. They represent hypertrophied detrusor musculature associated with detrusor overactivity and functional or anatomic bladder obstruction. A bladder diverticulum can occur when high intravesical pressure produces an enlargement of the intervening sacculations. The thick muscular band that creates the neck varies in diameter and gives way to outpouchings of bladder mucosa. The interior of the diverticulum has been reported to be the site of neoplasm in approximately 7% of cases. They may also occur after vaginal hysterectomies, urologic procedures, vaginal mesh procedures, radiation, cancer, and obstetric trauma. Posthysterectomy fistulas are usually located in the bladder base superior to the interureteric ridge, corresponding to the level of the vaginal cuff. In the immediate postoperative state, the surrounding mucosa is edematous and hyperemic; in later stages, the mucosa has a smooth appearance. In contrast, vesicoenteric fistulas uniformly have a surrounding inflammatory reaction, often with bulbous edema, and the fistulous tract is not discernible in two-thirds of cases. Bladder calculi may result from urinary stasis or the presence of a foreign body, or an inflammatory exudate may coalesce and serve as a nidus for stone formation. They can become attached to small areas of exposed mesh, slings, or nonabsorbable sutures. Stones have extremely variable cystoscopic appearances in terms of color, size, and shape but generally have an irregular surface. Foreign bodies and stones are usually accompanied by varying degrees of general or localized inflammatory reaction. The direct examination of the female bladder with elevated pelvis: the catheterization of the ureters under direct inspection, with and without elevation of the pelvis. Flexible fiber optic and rigid-rod lens endoscopy of the lower urinary tract: a prospective controlled comparison. The contribution of urethrocystoscopy to a combined urodynamic and urethrocystoscopic evaluation of urinary incontinence in women. Supine urethroscopic and standing cystometry as screening methods for the detection of detrusor instability. Predictive value of urethroscopy as compared to urodynamics in the diagnosis of genuine stress incontinence. Summary of the National Institute of Arthritis, Diabetes, Digestive and Kidney Diseases workshop on interstitial cystitis, National Institute of Health, Bethesda, Maryland, J Urol. The focus of this chapter is on describing the radiologic studies used in clinical practice and research by radiologists and pelvic floor specialists. Plain Film of the Abdomen the plain abdominal radiograph may be used as a primary study or as a scout film in anticipation of contrast media. Pelvic floor disorders include a broad array of interrelated clinical conditions that include urinary incontinence, pelvic organ prolapse, fecal incontinence, sensory abnormalities, and defecatory dysfunction. Bothersome symptoms may also stem from anatomic anomalies such as a urethral diverticulum, a paravaginal mass, or a surgical implant. In addition to a thorough clinical evaluation, multiple imaging modalities are now available to guide the clinician to the appropriate diagnosis and management. Beyond its clinical application, advanced imaging technology has an increasingly important role in our quest to understand the pathophysiology of pelvic 182 Retrograde and Antegrade Pyelography Retrograde pyelography is performed to evaluate the ureters and intrarenal collecting system. In retrograde pyelogram, the contrast medium is injected into the upper urinary tract through a cone-tipped catheter placed at cystoscopy under fluoroscopic guidance. This approach is associated with a higher infection rate than antegrade pyelography and may be contraindicated in women with a known allergic reaction to contrast media or recent lower urinary tract trauma or surgery. The large amount of contrast medium injected and the pressure applied during retrograde pyelogram may result in anastomotic leak and extravasation, with systemic absorption of the contrast. This approach involves placing a small-gauge needle into the renal pelvis; it is rarely performed for diagnostic indications only and is usually performed only when there is another indication for percutaneous puncture of the kidney. A flexible 20- or 22-gauge needle is inserted into the collecting system under ultrasound or fluoroscopic control after administration of intravenous contrast medium. An obstructed renal collecting system should be decompressed before contrast medium is injected, to avoid overdistention and urosepsis. Additional procedures, such as attempts at antegrade ureteral stenting, can then be performed to temporarily or permanently relieve the obstruction. To determine whether a cystotomy or fistula repair has healed, the bladder is filled slowly with contrast medium, and then is drained. Contrast from extraperitoneal leakage usually forms an irregularly shaped mass around the defect and remains there for a relatively long time. Contrast that has leaked from an intraperitoneal defect diffuses into the abdominal cavity and is rapidly absorbed through the peritoneal cavity. It can also be used during surgery to help expand and identify urethral diverticula and to test the integrity of repairs Cystography Cystography is frequently performed to detect bladder injury after trauma, to diagnose fistulas between the bladder and the adjacent organs, and to confirm that a cystotomy or bladder fistula has healed after surgical repair. This study requires a Tratner catheter, which has two balloons, with an opening in the lumen of the catheter between the two balloons for contrast injections. The distal balloon is placed into the bladder, and the proximal (sliding) balloon is positioned just outside the external urethral meatus. Video-Cystourethrography Video-cystourethrography combines a fluoroscopic voiding cystourethrogram with simultaneous intravesical, intraurethral, and intra-abdominal pressures and urine flow rate. Some controversy exists regarding the indications for video-cystourethrography and whether it should be performed routinely or selectively. Urethra Vagina Anal canal Symphysis Ultrasound Ultrasound offers real-time evaluation that can be obtained in an office setting and is well tolerated by patients. Other important advantages include the absence of ionized radiation, the wide availability, and acceptable cost-effectiveness. Recent advances in three-dimensional (3D) ultrasonography allow the clinician to simultaneously view axial, transverse, and coronal views and construct an accurate 3D image of the pelvic structures. Four-dimensional (4D) imaging involves real-time acquisition, providing an insight into functional anatomy and the changes that take place with straining and Valsalva maneuver. The diagnostic potential of 3D and 4D modalities is currently under investigation; once validated, it may become an important component in urogynecologic and urologic practice. Several ultrasound techniques are available for evaluation of the lower urinary tract and pelvic floor. These include transabdominal (T-A), transvaginal (T-V), perineal (also referred to as translabial), introital, and transrectal approaches. Bladder Uterus Cranial Ampulla recti Cul de sac A Techniques Perineal and Introital Ultrasonography For dynamic assessment, the T-V approach may exert a compressive effect on the lower urinary tract. Therefore, to prevent distortion of the anatomy of the lower urinary tract by probes, perineal (translabial) and introital approaches are used. Both techniques can be performed with the patient in dorsal lithotomy, semireclining, or standing positions. The introital technique uses a sector endovaginal probe with a frequency between 5 and 7. The pressure exerted by the transducer should be kept low but sufficient to obtain good images with high resolution. The presence of a full rectum may impair diagnostic accuracy and sometimes necessitates a repeat assessment after defecation. The bladder volume should be fixed on examination: 300 mL for the evaluation of dynamic changes of the bladder neck and <50 mL for the assessment of bladder wall thickness. The bladder volume can be estimated by either a T-A or T-V approach, although accuracy is not reliable for bladder volumes <50 mL. Three-dimensional and 4D ultrasound technology allows a multiplanar display mode with visualization of cross-sectional planes. Four-dimensional imaging allows the real-time acquisition of ultrasound data, with the ability to store cine-loops, which makes it feasible to evaluate dynamic changes in the pelvic floor, such as during a Valsalva maneuver. T-V Ultrasonography T-V ultrasound is performed with the patient in the dorsal lithotomy position. The biplane electronic probe provides two-dimensional sagittal and axial sectional imaging of the anterior and posterior compartments. Transrectal Ultrasonography Transrectal ultrasound (also referred to as endoanal and endosonography) is performed with an intracavitary probe, similar to T-V ultrasound. The scan starts at the upper aspect of the puborectalis muscle and extends to the anal verge. Three-dimensional reconstruction allows visualization of the structures in different planes as well as better localization of masses, abscesses, or fistulas. Routine uses of ultrasound that have been most described in evaluating lower urinary tract and pelvic floor are listed in Box 13. A well-known sonographic finding in patients with overactive bladder is wavelike detrusor contractions accompanied by bladder neck opening. With a cutoff value of 5 mm, bladder wall thickness together with symptoms of overactive bladder had a sensitivity of 84% and specificity of 89% for detecting detrusor overactivity, compared with video-cystourethrography. The authors speculated that the increased bladder wall thickness in this disorder resulted from detrusor hypertrophy associated with increased isometric detrusor contraction, urethral sphincter volume, and urethral closure pressure. Ultrasonographic studies for stress incontinence have been used to provide quantitative measurements and qualitative descriptions of the lower urinary tract. The differences between resting and stress bladder neck angles yield the rotational angle, which represents urethral or bladder neck mobility in a similar way as the Q-tip test. No values are defined for normal bladder neck descent or urethral mobility, possibly because of methodologic variations such as patient position, bladder filling, quality of Valsalva maneuver, and measurements of bladder neck position. Whereas several studies have demonstrated that the position of the bladder neck in patients with stress incontinence is lower than those of continent women, an overlap exists between the groups. Bladder neck funneling also may be observed and is seen in women with both stress and urge incontinence. On some occasions, opening of the bladder neck may be followed by egress of urine, which is manifested as a hyperechoic flow from the bladder through the urethra on real-time scanning. Funneling may be seen in asymptomatic women; therefore, its significance is unclear. Bladder Abnormalities Abnormalities of the bladder wall include focal or generalized thickening, loss of integrity, and abnormal vascularity. Infection, pelvic radiation, pelvic surgery, bladder outlet obstruction, and neoplasm can cause bladder wall thickening. In patients with bladder outlet obstruction, thickened bladder wall with trabeculation or even formation of diverticulum and high postvoid residual urine volume may be displayed on ultrasonography.
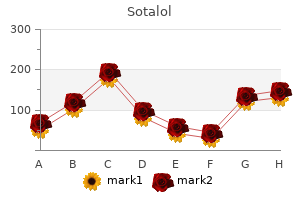
It does not slough off; rather blood pressure natural remedy cheap sotalol 40 mg online, it helps the functionalis layer regenerate each month heart attack history sotalol 40 mg purchase visa. The mons pubis is a mound of hair-covered adipose tissue overlying the symphysis pubis arteria 7ch generic 40 mg sotalol visa. Urethral opening the labium majus is one of two thick folds of skin and adipose tissue; hair grows on the lateral surfaces of the labia majora while the inner surfaces are hairless heart attack japanese order generic sotalol pills. The labia minora meet to form a hood of tissue called the prepuce over the clitoris heart attack 40 year old female cheap sotalol 40 mg line. The labium minus is a thinner, hairless fold of skin just inside each labium majus. The area inside the labia is called the vestibule; it contains the urethral and vaginal openings. Vaginal opening Anus Breasts Developing during puberty (as a result of stimulation by estrogen and progesterone), the breasts lie over the pectoralis major muscle. Each breast contains 15 to 20 lobules separated by fibrous tissue and adipose tissue. Each lobule consists of clusters of tiny, sac-like acini that secrete milk during lactation. Minute ducts drain the acini, merging to form larger ducts as they travel toward the nipple. Before reaching the nipple, the ducts enlarge slightly to form lactiferous sinuses. Sebum from these glands lubricates the areola, helping prevent dryness and cracking during nursing. Suspensory ligaments help support the breasts and also serve to attach the breasts to the underlying pectoralis muscles. Estrogen is the hormone responsible for producing the feminine physical changes that occur during puberty, such as the development of breasts; the deposition of fat beneath the skin of the hips, thighs, and buttocks; and the widening of the pelvis. Puberty tends to begin earlier in females than in males, at about age 9 or 10 as opposed to age 13. These changes, called the reproductive cycle, consist of two interrelated cycles: the ovarian cycle, which centers on changes in the ovaries, and the menstrual cycle, which focuses on changes in the uterus. Controlled by varying patterns of hormone secretion, the reproductive cycle averages 28 days in length; however, the length of the cycle can range from 20 to 45 days, depending upon the individual. Life lesson: Breast cancer Breast cancer affects one out of eight women and is one of the leading causes of cancer-related death. Most breast cancers begin in the ducts and, from there, can spread to other organs by way of the lymphatic system. Symptoms of breast cancer include a lump in the breast or armpit; redness, dimpling, or puckering of the skin of the breast; or drainage from the nipple. About 20% to 30% of women with breast cancer have a family history of the disease. Because many breast tumors are stimulated by estrogen, women who begin menstruating before age 12, as well as those who go through menopause after age 55, have an increased risk for the developing breast cancer. Women who have never had children or who had them only after age 30 also have an increased risk. Other risk factors include aging, excessive alcohol use, and exposure to radiation. Each oocyte (which is surrounded by follicular cells) reaches an early stage of meiosis before halting development. Many of these oocytes-also called primary follicles-degenerate during childhood. As the follicle develops, it secretes estrogen (which stimulates the thickening of the endometrium in the menstrual cycle) as well as small amounts of progesterone. The fimbriae of the fallopian tube sweep across the top of the ovary to catch the emerging oocyte. The corpus luteum secretes large amounts of progesterone and small amounts of estrogen. The progesterone causes the endometrium to continue to thicken and become more vascular, preparing it for pregnancy. This cycle involves the buildup of the endometrium (which occurs through most of the ovarian cycle) followed by its breakdown and discharge. The menstrual cycle is divided into four phases: the menstrual phase, proliferative phase, secretory phase, and premenstrual phase. Phases of the Menstrual Cycle Phase Menstrual Days 1 to 5 Activity the first day of noticeable vaginal bleeding is the first day of the menstrual cycle. Lasting from 3 to 5 days, menstruation occurs as the endometrium sheds its functional layer (the stratum functionalis). About day 6, rising levels of estrogen (secreted by the ovaries) stimulates the repair of the base layer as well as the growth of blood vessels. During this phase, the endometrium develops into a nutritious bed about 5 to 6 mm thick, just right for a fertilized ovum. The endometrium becomes ischemic and necrotic, causing it to slough off the uterine wall. Study the chart below to tie the activities of the two cycles together and to link each to the fluctuations in hormone levels. Called menopause, this stage of life is associated with declining estrogen and progesterone levels (as the remaining ovarian follicles are less responsive to gonadotropins). As a result of the declining hormone levels, the uterus, vagina, and breasts atrophy. Vaginal dryness can make intercourse uncomfortable and vaginal infections more common. Symptoms of menopause vary, although common symptoms include hot flashes and mood changes. Excitement · Blood flow to the genitals increases, causing the labia minora and majora to swell with blood. Orgasm · Muscles in the outer third of the vagina contract rapidly in a series of pulses. The following table summarizes some of the most common methods of contraception, beginning with the most effective methods and ending with the least effective. Barrier Methods · this form of contraceptive blocks sperm from entering or proceeding past the vagina. Because it is difficult to predict the time of ovulation, this method has a 25% failure rate. This method also has a high failure rate, both due to a lack of control as well as the fact the some sperm are present in pre-ejaculatory fluids. The first hormone secreted at the onset of puberty in both males and females is: a. The structure that secretes progesterone during the last half of the ovarian cycle is the: a. The seminal vesicles secrete fluid into the ejaculatory duct to help form the fluid portion of semen. The sustentacular (Sertoli) cells supply nutrients to sperm; they also secrete the hormone inhibin, which plays a role in the maturation and release of sperm. The bulbourethral gland supplies 5% of the fluid volume of semen, while the prostate supplies 30% (as opposed to the 65% supplied by the seminal vesicles). Progesterone is secreted by the corpus luteum to maintain the vascular endometrial lining. The myometrium is the muscular layer that contracts during the delivery of a fetus. The vestibule is the area between the labia that contains openings to the urethra and vagina. Birth control pills do not act to change the acidity of the vagina for the purpose of killing sperm. Discuss the process of fertilization, including when and where it occurs and how the egg prevents fertilization by more than one sperm. Summarize the process of implantation and the changes that occur in the blastocyst. Name the three germ layers and identify the major organs and tissues arising from each. Identify the three stages of labor and describe the actions, as well as the duration, of each stage. The instant that occurs, the fertilized egg begins a series of changes that, amazingly, transforms a single cell into a fully developed human being. Consider: from that one cell come 100 trillion cells-cells that, in turn, evolve into tissues as diverse as skin, nerves, and blood, and organs as varied as the kidneys, brain, and heart. Indeed, from one cell come not just your physical body but also your mind, your emotions, and your intellect. The process of human development, from conception until birth, is perhaps the most fascinating and miraculous aspect of human life. Sperm enter the female reproductive tract when the male ejaculates, releasing approximately 100 million sperm into the vagina. Once there, the sperm actively swim toward the fallopian tubes, drawn forward on a mission to fertilize an egg. The acidity of the vagina destroys many of the sperm; others fail to make it through the cervical mucus; finally, white blood cells in the Site of uterus destroy still more. Sperm can remain viable within the female reproductive tract for as long as six days. Because it takes 72 hours for the egg to reach the uterus, fertilization typically occurs in the distal third of the fallopian tube. Keep in mind that this is a "time lapse" view of fertilization: although many sperm assist with fertilization, only one sperm actually enters the egg. Granulosa cells 2 Due to the efforts of multiple sperm, a path through the zona pellucida eventually results, allowing a single sperm to penetrate. As soon as this happens, the egg undergoes changes that bar any other sperm from entering. The nucleus of the sperm (which has 23 chromosomes) fuses with the nucleus of the egg (which also has 23 chromosomes), creating a single cell with 46 chromosomes. After about 18 hours in a temperaturecontrolled environment, the eggs are examined. If fertilization has occurred, the eggs are kept in an incubator for 2 or 3 more days to allow them to grow into the 8- or 16-cell stage. If implantation occurs, the pregnancy test is positive and the pregnancy proceeds. The mitotic divisions continue, with each division doubling the number of cells, until the zygote arrives at the uterus. The following illustration portrays this sequence of events, beginning with ovulation and ending with implantation of a fertilized egg. Three to four days after fertilization, the morula enters the uterine cavity, where it floats for two or three days. Blastomere First mitosis Morula Blastocyst Inner cell mass Trophoblast Ovary Ovum Implantation 4 As the morula continues to divide, a hollow cavity forms; the morula is now called a blastocyst. The blastocyst consists of an outer layer of cells (the trophoblast) and an inner cell mass. The trophoblast eventually forms the placenta while the inner cell mass becomes the embryo. As the blastocyst attaches to the endometrium, it continues to change rapidly as it moves toward becoming an embryo. As these outer cells penetrate the endometrium, the inner cell mass separates from the trophoblast, creating a narrow space called the amniotic cavity. Some of the cells on the interior portion of the embryonic disc multiply to form another cavity, called the yolk sac. Meanwhile, the rapidly growing endometrium covers the top of the blastocyst, burying it completely. The embryonic disc gives rise to three layers, called germ layers, which produce all the organs and tissues of the body. Germ layers: Each germ layer gives rise to specific organs, a process called organogenesis. Ectoderm Mesoderm Endoderm Develops into the epidermis, nervous system, pituitary gland, optic lens, and salivary glands. Develops into the epithelial lining of the digestive and respiratory tracts, parts of the bladder and urethra, thyroid and parathyroid glands, liver, and thymus. Two key events occur during the next six weeks: the germ layers differentiate into organs and organ systems, and several accessory organs emerge to aid the developing embryo. The accessory organs include four extraembryonic membranes-the amnion, chorion, allantois, and yolk sac-as well as the placenta and umbilical cord. Extraembryonic Membranes the amnion is a transparent sac that completely envelops the embryo. The amnion is filled with amniotic fluid, which protects the embryo from trauma as well as changes in temperature. The volume remains stable because the fetus also regularly urinates into the amniotic sac. Developing placenta Uterus Chorionic villus the allantois serves as the foundation for the developing umbilical cord. Amniotic cavity the chorion-the outermost membrane-surrounds the other membranes. In the area of the umbilical cord, the chorion forms what will become the fetal side of the placenta. The yolk sac produces red blood cells until the sixth week, after which this task is taken over by the embryonic liver. Besides contributing to the formation of the digestive tract, the yolk sac provides nutrients and handles waste disposal.
Sotalol 40 mg fast delivery. New Recall Issued On Blood Pressure Heart Failure Medications.
References
- Holick MF, Krane SM, Potss JT Jr. Calcium, phosphate and bone metabolism: Calcium-regulating hormones. In: Fauci A, Harrison TR, eds. Harrisonis Principles of Internal Medicine. 14th ed. New York: McGraw-Hill, New York, 1998.
- Hendry WF, Hughes L, Scammell G, et al. Comparison of prednisolone and placebo in subfertile men with antibodies to spermatozoa. Lancet 1990; 335:85-88.
- Sala F, Manganotti P, Tramontano V, Bricolo A, Gerosa M. Monitoring of motor pathways during brain stem surgery: what we have achieved and what we still miss? Neurophysiol Clin. 2007;37(6): 399-406.
- Stepniakowski K and Egan BM. Additive effects of obesity and hypertension to limit venous volume. Am. J. Phys. 1995;268:R562-R568.
- Houlden H, King RH, Muddle JR, et al. A novel RAB7 mutation associated with ulcero-mutilating neuropathy. Ann Neurol. 2004;56(4):586-590.
- Clark VE, Erson-Omay EZ, Serin A, et al. Genomic analysis of non-NF2 meningiomas reveals mutations in TRAF7, KLF4, AKT1, and SMO. Science 2013; 339:1077-1080.
- Shawki HB, Muhammed SM, Reda AN, Abdulla TS, Ardalan DM. Pulmonary lymphangioleiomyomatosis. Saudi Med J 2007;28(1):131-4.
- Slabaugh, T.K., Machaidze, Z., Hennigar, R., Ogan, K. Monitoring radiofrequency renal lesions in real time using contrast-enhanced ultrasonography: a porcine model. J Endourol 2005;19:579-583.